The Growing Popularity of Tooth Whitening
The dental team must be well-versed in tooth whitening options, from over-the-counter products to in-office treatments, as more and more consumers seek a whiter, brighter smile.
Tooth whitening has enjoyed a tremendous increase in popularity in recent years and is now one of the most common cosmetic procedures performed in contemporary dental practice. According to the American Dental Association’s 2003 nationwide public opinion survey of more than 1,000 adults, patients asked their dentists about tooth whitening more frequently than any other dental topic. Nearly 20% of patients inquired about tooth whitening in 2003, compared to just 11% in 2001. In addition, 29% of patients used whitening products at home—nearly triple the number who reported using such products in 2001.1 Whitening is an effective, conservative treatment option for a wide range of tooth discolorations, including fluorosis, age-related yellowing, tobacco staining, and darkening caused by medications such as tetracycline and minocycline.2,3
Today’s consumers can choose from three basic approaches to tooth whitening: professionally-administered in-office bleaching; professionally-dispensed, self-applied at-home bleaching using custom-fitted trays (nightguard vital bleaching) or polyethylene strips; or self-directed whitening using over-the-counter (OTC) dental bleaching products. With proper case selection and execution, each method is capable of producing satisfactory results.4
The History of Tooth Whitening
Tooth whitening techniques are not new to dentistry. Bleaching has been used to lighten teeth since the mid-1800s. In 1850, Dwinnell5 described the use of chloride of lime to bleach nonvital teeth. Over the next several decades, other bleaching agents, including oxalic acid, etherperoxide (Pyrozone), and hydrogen peroxide, were introduced.6 Although the mechanism of action is not fully understood, tooth color change is believed to occur as a result of the breakdown of organic pigment by an oxidizing agent, eg, peroxide compounds. Because of its low molecular weight, hydrogen peroxide diffuses easily through enamel and dentin. In dentin, hydrogen peroxide molecules, which are highly unstable, release oxygen to form free radicals, which, in turn, attack the pigmented organic molecules of the dentin. As their carbon double bonds are broken (oxidized), the pigments lighten from their original yellow color to almost colorless. Similarly, the lightening of darker discolorations caused by ingestion of chromagenic agents such as fluoride or tetracycline occurs by the same oxidative process.6,7
By the early 1900s, in-office “power bleaching,” using 35% hydrogen peroxide activated by a heat or light source, was well accepted for lightening vital teeth. This technique remains in use today. To reduce the potential for pulpal irritation, high intensity heat lamps have been replaced by light- or chemically-activated catalysts. Results are usually immediately noticeable, although they may be somewhat unpredictable. Moreover, in-office bleaching can often require multiple treatment sessions and, even without high heat, the high concentrations of peroxide may cause pulpal or soft tissue irritation, resulting in patient discomfort, either during or after the procedure.6, 8,9
In 1989, Haywood and Heymann10 introduced nightguard vital bleaching (NGVB), or “dentist-prescribed at-home bleaching,” using 10% carbamide peroxide in custom-fitted trays as an alternative to the in-office technique. NGVB’s safety and effectiveness are well established.11-15 Because lower concentration peroxide compounds are used, the potential for adverse side effects when compared to the in-office procedure is greatly reduced. Pulpal sensitivity is common, but is generally mild and subsides with the termination of treatment. Clinical results, both short- and long-term as well as patient acceptance, have been outstanding. NGVB remains the benchmark against which all other whitening techniques are measured.
The OTC Option
In addition to professionally administered in-office and NGVB procedures, many OTC bleaching products are available for consumer purchase. In recent years, some major pharmaceutical companies have entered the OTC market. As a result, at least some of the OTC bleaching products currently available represent marked improvements in technology and efficacy over earlier products. Most notable among the newer products are whitening strips, which contain a thin (0.1-0.2 mm) gel layer of 6.5% or 14% hydrogen peroxide4, 16-18 and paint-on gels containing 18% carbamide peroxide or 19% sodium percarbonate.19,20 The whitening strips contain only 100 to 200 mg of gel (13-14 mg of hydrogen peroxide)—less than half the amount used in some tray-based systems. The higher gel concentration enhances peroxide diffusion through enamel, thus improving the whitening effect, while the lowered gel volume reduces the possibility of soft tissue irritation.16,17 A growing body of literature suggests that these products can be quite effective.21-23 OTC bleaching agents may indeed be a viable and satisfactory treatment option for many patients. Nevertheless, a comprehensive examination and diagnosis by a dental professional remains the safest way to determine the best course of treatment from among the ever expanding and often confusing list of available products.24 The web version of this article features a table detailing the concentrations of commonly used tooth whitening agents.
Dentists and dental hygienists must be aware of the potential for patients to combine prescription and OTC products and even to misuse bleaching products in their quest for the perfect smile. Indiscriminate use may result in increased thermal sensitivity and/or soft tissue irritation. In addition, the teeth may become noticeably lighter than adjacent resin composite or porcelain restorations, which may necessitate the replacement of otherwise acceptable restorations to re-establish optimal esthetics. Therefore, the dental health care team should advise patients of possible adverse effects and caution them against over-using both prescription and OTC products.25
Case Presentation
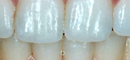
 This 17-year-old patient sought vital tooth whitening about 1 year following completion of his orthodontic treatment (Figure 1). His clinical presentation suggested a very mild generalized diffuse fluorosis. Overall base shade approximated Vita A-2, with the maxillary canines and first premolars exhibiting increased saturation, approaching Vita A-3. In-office bleaching was not considered, primarily because of scheduling difficulties and the potential for inducing pulpal sensitivity in relatively young teeth. Whitening strips were considered but, in this case, the maxillary canines required selective bleaching prior to lightening the entire arch; whitening strips do not lend themselves well to selective application on individual teeth. Therefore, NGVB was chosen. However, since the patient still wears removable orthodontic retainers while sleeping, his orthodontist was consulted prior to initiating treatment. With permission to wear his orthodontic retainer and bleaching tray on alternating nights, a scalloped bleaching tray was fabricated and 10% carbamide peroxide dispensed. To ensure a slightly tighter fit and thus limit tooth movement, facial reservoirs were not included in the tray design. During the first week, the patient applied bleaching gel to only teeth #5, #6, #11, and #12. After the canines and first premolars were lightened to match the central and lateral incisors, the entire arch was lightened further. After 4 weeks of overnight wear (wearing his bleaching tray and orthodontic retainer on alternate nights) and occasional daytime wear (2-3 hours per application), the upper teeth were lightened to approximately Vita B-1 shade (Figure 2). Treatment could have been completed more quickly if the patient had used his bleaching tray on consecutive nights. However, the risk of orthodontic shifting was too significant to warrant abandoning his orthodontic retainer for more than 24-48 hours at a time. The patient was able to wear the maxillary bleaching tray simultaneously with his mandibular orthodontic retainer with no discomfort. With the maxillary arch completed, the patient has begun a similar regimen to lighten the mandibular arch.
This 17-year-old patient sought vital tooth whitening about 1 year following completion of his orthodontic treatment (Figure 1). His clinical presentation suggested a very mild generalized diffuse fluorosis. Overall base shade approximated Vita A-2, with the maxillary canines and first premolars exhibiting increased saturation, approaching Vita A-3. In-office bleaching was not considered, primarily because of scheduling difficulties and the potential for inducing pulpal sensitivity in relatively young teeth. Whitening strips were considered but, in this case, the maxillary canines required selective bleaching prior to lightening the entire arch; whitening strips do not lend themselves well to selective application on individual teeth. Therefore, NGVB was chosen. However, since the patient still wears removable orthodontic retainers while sleeping, his orthodontist was consulted prior to initiating treatment. With permission to wear his orthodontic retainer and bleaching tray on alternating nights, a scalloped bleaching tray was fabricated and 10% carbamide peroxide dispensed. To ensure a slightly tighter fit and thus limit tooth movement, facial reservoirs were not included in the tray design. During the first week, the patient applied bleaching gel to only teeth #5, #6, #11, and #12. After the canines and first premolars were lightened to match the central and lateral incisors, the entire arch was lightened further. After 4 weeks of overnight wear (wearing his bleaching tray and orthodontic retainer on alternate nights) and occasional daytime wear (2-3 hours per application), the upper teeth were lightened to approximately Vita B-1 shade (Figure 2). Treatment could have been completed more quickly if the patient had used his bleaching tray on consecutive nights. However, the risk of orthodontic shifting was too significant to warrant abandoning his orthodontic retainer for more than 24-48 hours at a time. The patient was able to wear the maxillary bleaching tray simultaneously with his mandibular orthodontic retainer with no discomfort. With the maxillary arch completed, the patient has begun a similar regimen to lighten the mandibular arch. 
Future Considerations
Few innovations in dentistry have generated as much positive public interest as at-home tooth whitening. Topically applied peroxide-based bleaching is the most conservative option for the treatment of discolored teeth. With appropriate evaluation, case selection, and patient compliance, clinical success is reasonably predictable. Although the longevity of their effects has not yet been firmly established, the newer OTC products offer much promise. Their primary limitations may be a shorter duration of effect prior to shade relapse and an inability to lighten darker teeth as quickly or thoroughly as higher concentration products. Manufacturers, however, are unlikely to increase OTC peroxide concentrations unless desensitizing agents, such as fluoride or potassium nitrate, are incorporated into product formulations as has been done for many tray-based whitening products. Nevertheless, the public appears willing to accept OTC products as lower cost alternatives to professionally administered procedures.
OTC whitening products, however, will not replace professionally-directed in-office whitening and NGVB procedures. OTC products will meet the needs of many, but not all, patients. Still others will simply prefer to have their teeth whitened professionally. Regardless, OTC products will generate increased interest and motivate patients to consult with their dentists and dental hygienists regarding bleaching and other cosmetic concerns. This will create opportunities for the dental health care team to educate and advise patients of the most appropriate means to achieve their esthetic goals.
 |
Disclaimer: The opinions expressed in this article are the private views of the author and should not be construed as reflecting official policies of the US Navy, Department of Defense or US Government.
References
- Berry J. What do they think? ADA survey offers up the scoop on your patients. ADA News. April 19, 2004:1-8.
- Haywood VB. Nightguard vital bleaching: current concepts and research. J Am Dent Assoc. 1997;128:19S-25S.
- Haywood VB. Frequently asked questions about bleaching. Compend Cont Educ Dent. 2003;24:324-338.
- Gerlach RW, Zhou X. Vital bleaching with whitening strips: summary of clinical research on effectiveness and tolerability. J Contemp Dent Pract. 2001;2:1-15.
- Dwinnell WW. Ninth annual meeting of American Society of Dental Surgeons, article X. Am J Dent Sci. 1850;1:57-61.
- Haywood VB, Berry TG. Natural tooth bleaching. In: Summit JB, Robbins JW, Schwartz RS, eds. Fundamentals of Operative Dentistry: A Contemporary Approach. 2nd ed. Chicago: Quintessence Publishing Company, 2001;401-426.
- Albers H. Lightening natural teeth. ADEPT Report. 1991;2(1):1-24.
- Barghi N. Making a clinical decision for vital tooth bleaching: at-home or in-office? Compend Cont Educ Dent. 1998;19 831-838.
- Perdigão J, Baratieri LN, Arcari GM. Contemporary trends and techniques in tooth whitening: a review. Pract Proc Aesthet Dent. 2004;16:185-192.
- Haywood VB, Heymann HO. Nightguard vital bleaching. Quintessence Int. 1989; 20:173-176.
- Haywood VB, Leonard RH Jr, Nelson CF, Brunson WD. Effectiveness, side effects, and long-term status of nightguard vital bleaching. J Am Dent Assoc. 1994;125:1219-1226.
- Li Y. Toxicological considerations of tooth bleaching using peroxide-containing agents. J Am Dent Assoc. 1997;128:31S-36S.
- Leonard RH Jr, Bentley C, Eagle JC, Garland GE, Knight MC, Phillips C. Nightguard vital bleaching: a long-term study on efficacy, shade retention, side effects, and patients’ perceptions. J Esthet Restor Dent. 2001;13:357-369.
- Ritter AV, Leonard RH Jr, St Georges AJ, Caplan DJ, Haywood VB. Safety and stability of nightguard vital bleaching: 9 to 12 years post-treatment. J Esthet Restor Dent. 2002;14:275-285.
- Leonard RH Jr, Haywood VB, Caplan DJ, Tart ND. Nightguard vital bleaching of tetracycline-stained teeth: 90 months post treatment. J Esthet Restor Dent. 2003;15:142-152.
- Gerlach RW, Sagel PA. Vital bleaching with a thin peroxide gel: the safety and efficacy of a professional-strength hydrogen peroxide whitening strip. J Am Dent Assoc . 2004; 135(1): 98-100.
- Gerlach RW, Barker ML. Professional vital bleaching using a thin and concentrated peroxide gel on whitening strips: an integrated clinical summary. J Contemp Dent Pract . 2004; 5(1): 1-17.
- Gerlach RW. Whitening paradigms revisited: Introduction of a thin and concentrated peroxide gel technology for professional tooth whitening. Compend Contin Educ Dent. 2004;25(Suppl):4-8.
- Nathoo S, Stewart B, Zhang YP, et al. Efficacy of a novel, nontray, paint-on 18% carbamide peroxide whitening gel. Compend Contin Educ Dent. 2002;23(Suppl):26-31.
- Barlow A, Gerlach RW, Date RF, et al. Clinical response of two brush-applied peroxide whitening systems. J Clin Dent. 2003;14:59-63.
- Brunton PA, Ellwood R, Davies R. A six-month study of two self-applied tooth whitening products containing carbamide peroxide. Oper Dent. 2004;29:623-626.
- Sagel PA, Landrigan WF. A new approach to strip-based tooth whitening: 14% hydrogen peroxide delivered via controlled low dose. Compend Contin Educ Dent. 2004; 25(Suppl):9-13.
- Swift EJ Jr, Miguez PA, Barker ML, Gerlach RW. Three-week clinical trial of a 14% hydrogen-peroxide, strip-based bleaching system. Compend Contin Educ Dent. 2004;25(Suppl ):27-32.
- Haywood VB. New bleaching considerations compared with at-home bleaching. J Esthet Restor Dent. 2003;15:184-187.
- Christensen GJ. Are snow-white teeth really so desirable? J Am Dent Assoc. 2005; 136:933-935.
From Dimensions of Dental Hygiene. Nov 2005;3(11):30-31.

