The Caries Balance
With an in-depth understanding of the caries process, dental hygienists can lead the fight to reduce or eliminate caries.
The dental hygienist should be at the forefront of caries prevention and intervention in the dental office and in the community. Understanding the caries process is essential to perform this role. Dental hygienists should be major players in driving a cross disciplinary approach to caries risk assessment and caries management with the goal of significantly reducing the prevelance of dental decay in our population. Comprehensive knowledge and the application of this knowledge to practice are necessary for this result.
Caries is a transmissible bacterial infection. Caries progress or reversal is determined by the balance between pathological and protective factors. Pathological factors include acid-producing bacteria, fermentable carbohydrates, and reduced salivary function. Protective factors include salivary components, fluoride together with calcium and phosphate to remineralize the lesion, and antibacterial therapy. The hygienist can provide education, participate in caries risk assessment, and provide therapy and follow-up for successful control of caries.
Dental caries is a transmissible bacterial infection, yet we do not deal with the infection in our management of dental decay. Conventional oral hygiene is simply not enough in many instances. Remineralization is our natural repair mechanism for carious lesions, provided they are not cavitated. Fluoride therapy enhances this repair process. However, if the bacterial challenge is too high, our efforts at repair are overcome and caries progresses to a cavity. This simple concept is the caries balance.
During the 1960s and 1970s, the fluoridation of water supplies in the United States reduced dental caries prevalence considerably.1 In the 1970s and 1980s, the almost universal use of fluoride-containing dentifrices brought further reductions in decay.2 During this same period, the acceptance of fluoride and remineralization in the dental office, together with fluoride topicals and sealant applications, made a major impact. However, we all know that millions of hours are spent annually in the United States placing restorations to “fix” caries.
Many people continue to get caries and some children and adults have a continual caries problem in spite of our preventive efforts.3,4 In these high risk individuals, we need to deal with the bacterial infection if the preventive measures are to be effective. We need a paradigm shift in our approach.
Bacterial Infection
The primary requirement for dental decay is the presence of acid-producing (acidogenic) bacteria. The bacteria need a substrate of fermentable carbohydrates to feed on to produce the acids that dissolve our tooth mineral.5,6 Certain species of bacteria have gone in and out of favor as the culprit over recent decades. It is now well established that multiple species are involved. We have all heard of Steptococcus mutans and, during the 1980s, this was proposed as the only causative agent by several sources.6 Efforts were considerable in studying this species and its many strains, in finding a vaccine, genetically altering the species, and trying to find ways to eliminate it.7
The key point, however, is that multiple species are involved, especially the mutans streptococci group and the lactobacillus species.5,8The mutans streptococci group includes several species of which S. mutans and S. sobrinus are the two most common that appear in human plaque. S. sobrinus does not occur as commonly as S. mutans but when it does, it is associated with high caries individuals.
Several lactobacillus species are associated with dental caries—both coronal and root caries. It was previously thought that lactobacilli colonized when cavities had already formed but several clinical studies have shown that lactobacilli are strongly associated with caries progression before the observation of cavities.5,8 Further, in patients with cavities, the lactobacilli are present in the remainder of the mouth after restorations are completed and continue to thrive and produce acids to cause future caries. These acidogenic bacteria only occupy about 1% or less of the total flora in the plaque. That such a small fraction of the bacteria present can cause such major problems is amazing.

The progression of caries.
The bottom line is that multiple species of acidogenic bacteria cause dental caries and the predominant groups identified so far are the mutans streptococci and the lactobacilli. Actinomyces species and some yeasts have also recently been suggested. From a practical therapeutic perspective, this means we need to use a broad spectrum antibacterial to reduce or eliminate these acidogenic bacteria in order to control caries in patients with a high bacterial loading.
Studies in the 1970s showed that specific strains of S. mutans are transmitted from mother to child.7,10,11 This conclusion was confirmed in the 1980s by DNA technology.7,12 It has taken 20 years for us to accept this conclusion and to start thinking about the source of the pathogenic (cariogenic, ie, caries-causing) bacteria that colonize the mouth. Studies have now established that early colonization, even before the teeth erupt, can occur in infants by transmission from the mother or caregiver. Transmission from child-to-child and adult-to-adult has also been reported for S. mutans. Presumably the same is also the case for lactobacilli. Children who are colonized early have more decay later.13,14 From a preventive perspective, we should target mothers and caregivers with high caries risk and control their bacteria, and, in the case of pregnant mothers, even before a child is born.
Fermentable Carbohydrates
The acidogenic bacteria described above can metabolize carbohydrates consumed by humans. They derive energy from them, just as we do, but the byproduct of their metabolism is organic acid. Common fermentable carbohydrates are glucose, sucrose, fructose, and cooked starch. Sucrose is particularly bad because the mutans streptococci can produce extracellular polysaccharides from sucrose that sticks the plaque together and also provides a food source for the bacteria between the times when eating provides that source.
Frequency of ingestion is the key factor rather than total amount of carbohydrate ingested. Every time we ingest one or more of these carbohydrates, the acidogenic bacteria produce acids, such as lactic, acetic, formic, or propionic acids, that within minutes lower the pH in the plaque and dissolve some tooth mineral. So snacking throughout the day and night produces multiple acid attacks. Substitution of the fermentable carbohydrates by noncariogenic sweeteners, such as aspartame, sorbitol, or xylitol, can play a big part in reducing the acid challenge to the teeth. Chewing gum enhances salivary function, helps neutralize any acids present, and promotes remineralization.
Salivary Dysfunction
The saliva is a very complex fluid that contains calcium and phosphate necessary for remineralization, proteins that keep calcium in solution, proteins and lipids that form the protective pellicle on the tooth surface, antibacterial proteins and immunoglobulins, and components that buffer and neutralize the acids produced by the bacteria.15 When salivary function is reduced or eliminated by disease or radiation therapy, all of these protective functions are reduced or lost and rampant caries can result.16
In some patients, the reduction in salivary function is the primary determinant of caries progression for them. The protective factors in the saliva have become insufficient to overcome the challenge. Many medications have hyposalivatory side effects. In patients who take multiple medications that markedly reduce saliva flow, such as tranquilizers, antihypertensives, and mood altering medications, this is particularly important and a key factor to look for in assessing caries risk.
Demineralization and Remineralization
Demineralization is the loss of mineral (calcium and phosphate) from the tooth as a result of attack by the acids produced by the acidogenic bacteria described above. Remineralization is the natural repair process that replaces some of the mineral lost during the formation of a carious lesion. The mineral that is replaced is less soluble than the original mineral. Fluoride inhibits demineralization and enhances remineralization.5,17
The mineral in our teeth and bones is called carbonated hydroxyapatite. It is a complicated calcium phosphate with many other ionic substitutions. The carbonate is an impurity that is included during the formation of the mineral because the fluids of our body are saturated with bicarbonate. The mineral crystal structure is weakened and is acid soluble as a result. The enamel crystals are small, long, and packed tightly together to form the physically strong coating on our teeth. Some protein and lipid is present that sticks these crystals together. Dentin has much smaller crystals that are even more acid soluble and have a much higher protein content that gives it the flexibility and strength to support the tooth function.
The acids produced in the plaque diffuse easily into the tooth—dissolving calcium and phosphate as they go. The calcium and phosphate diffuse out of the tooth and, if this process continues long enough, a cavity results. This is demineralization and leads to the formation of a carious lesion. Fluoride applied topically via dental products such as toothpaste, mouthrinse, or office applied gel or foam markedly inhibits demineralization if present at the time of the acid challenge.5,18
|
|
|
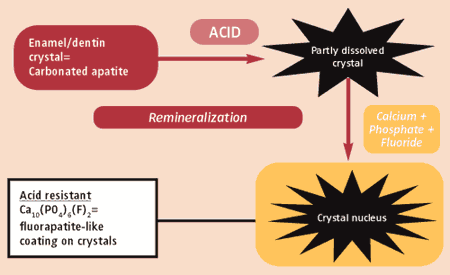
FIGURE 1. Schematic representation of demineralization and remineralization as the basis for the process of dental caries. |
Up until the point of cavitation, the process can be reversed by calcium and phosphate from the saliva traveling into the tooth and crystallizing onto the partially dissolved crystal remnants in the subsurface carious lesion. This is remineralization.
If fluoride is present in the plaque it travels with the calcium and phosphate and speeds up this crystal growth. Further, the new surface that is formed on the crystal excludes carbonate, preferentially includes fluoride, and is much less acid soluble. The “fluorapatite-like” veneer is what the acid sees next time it penetrates and cannot dissolve it, causing the acid to pass on deeper before finding a susceptible site (see Figure 1). Fluoride that enhances remineralization comes from topical sources such as drinking water, fluoride dentifrice, mouthrinse, office applied topical, or varnish.
The Caries Process
I proposed the caries balance concept as a simple way to look at the caries process and see whether it was progressing or reversing.5,19 The most important components are illustrated in Figure 2. The pathological factors are: 1) acidogenic bacteria, 2) frequency of ingestion of fermentable carbohydrates, and 3) salivary dysfunction. The three most important protective factors are: 1) salivary components and flow, 2) fluoride, calcium, phosphate, and remineralization, and 3) antibacterial therapy. Additional therapies, such as sealants, can be added to the protective factors.
|
|
| FIGURE 2. The caries balance. Schematic representation of the balance between pathological factors and protective factors in the maintenance or progression of dental caries. Modified from: Featherstone JDB. Prevention and reversal of dental caries: role of low level fluoride. Comm Dent Oral Epidemiol. 1999;27:31-40. Reprinted with permission from Blackwell Publishing Ltd. |
So what are the practical implications of this concept? The balance can be used to assess the risk of an individual developing caries in the future, to determine why the individual has caries now, or to drive a preventive or interventive program for the individual or even community.18,20 The balance between demineralization and remineralization is the key to progression or reversal of caries at any time. We can intervene to tip the balance.
Additional fluoride therapy will usually enhance remineralization, whereas in the case of high bacterial challenge, we need to apply aggressive antibacterial therapy to reduce the acidogenic bacterial loading in the mouth. Placing a restoration does not reduce the overall bacterial loading in the mouth.21 It certainly removes the bacteria from that specific cavity, but does little to help reduce the future bacterial challenge.
Chlorhexidine mouthrinse can be used to help with this. In the United States, we have 0.12% chlorhexidine gluconate.22 Studies suggest that daily mouthrinsing for 2 weeks substantially reduces the loading of mutans streptococci but they recolonize within a few weeks. Therefore, repeated treatments are necessary to control the bacterial infection. A useful regiment is to rinse daily for 1 week every month. This regimen enhances compliance and reduces the bacterial loading over several months.
Conclusion
Dental caries progression or reversal is determined by the balance between pathological and protective factors. Fluoride inhibits demineralization and enhances remineralization. Saliva is very important as a protective factor and salivary dysfunction is a common pathological factor. If the bacterial challenge is high, then protective factors may not be sufficient to overcome the demineralization process. Antibacterial therapy and intervention in the transmission of bacteria must become part of the standard of care in caries control and part of the tool chest of the dental hygienist. The dental hygienist should be responsible for educating patients, for delivering caries risk assessment, for providing preventive care, and being the front line person in the paradigm shift to reduce or eliminate dental caries.
References
- Newbrun E. Effectiveness of water fluoridation. J Public Health Dent. 1989;49:279-289.
- Jenkins GN. Recent changes in dental caries. Br Med J. 1985;291:1297-1298.
- Winn DM, Brunelle JA, Selwitz RH, et al. Coronal and root caries in the dentition of adults in the United States, 1988-1991. J Dent Res. 1986;75:642-651.
- Kaste LM, Selwitz RH, Oldakowski RJ, Brunelle JA, Winn DM, Brown LJ. Coronal caries in the primary and permanent dentition of children and adolescents 1-17 years of age: United States, 1988-1991. J Dent Res. 1996;75:631-641.
- Featherstone JDB. The science and practice of caries prevention. J Am Dent Assoc. 2000;131:887-899.
- Loesche WJ. Role of Streptococcus mutans in human dental decay. Microbiol Rev. 1986;50:353-380.
- Berkowitz RJ. Acquisition and transmission of mutans streptococci. J CalifDent Assoc. 2003;3:135-137.
- Leverett DH, Proskin HM, Featherstone JDB, et al. Caries risk assessment in a longitudinal discrimination study. J Dent Res. 1993;72:538-543.
- Krasse B. Biological factors as indicators of future caries. Int Dent J. 1988;38:219-225.
- Berkowitz RJ, Jordan HV, White G. The early establishment of Streptococcus mutans in the mouths of infants. Arch Oral Biol. 1975;20:171-174.
- Berkowitz RJ, Jordan HV. (1975) Similarity of bacteriocins of Streptococcus mutans from mother and infant. Archs Oral Biol. 1975;20:725-730.
- Caufield PW, Childers NK, Allen DN, Hansen JB. Distinct bacteriocin groups correlate with different groups of Streptococcus mutans plasmids. Infect Immun. 1985;48:51-56.
- Alaluusua S, Kleemola-Kujala E, Nystrom M, Evalahti M, Gronroos L. Caries in the primary teeth and salivary Streptococcus mutans and lactobacillus levels as indicators of caries in permanent teeth. Pediatr Dent. 1987;9:126-130.
- Alaluusua S, Renkonen OV. Streptococcus mutans establishment and dental caries experience in children from 2 to 4 years. Scand J Dent Res. 1983;91:453-457.
- Lamkin MS, Oppenheim FG. Structural features of salivary function. Crit Rev Oral Biol Med. 1993;4:251-259.
- Mandel ID. The role of saliva in maintaining oral homeostasis. J Am Dent Assoc. 1989;119:298-304.
- Ten Cate JM, Featherstone JDB. Mechanistic aspects of the interactions between fluoride and dental enamel. Crit Rev Oral Biology Med. 1991;2:283-296.
- Featherstone JDB. The caries balance: contributing factors and early detection. J Calif Denta Assoc. 2003;31:129-133.
- Featherstone JDB. Prevention and reversal of dental caries: role of low level fluoride. Community Dent Oral Epidemiol. 1999;27:31-40.
- Featherstone JDB, Adair SM, Anderson MH, et al. Caries management by risk assessment: consensus statement, April 2002. J Calif Denta Assoc. 2003;31:257-269.
- Featherstone JDB, Gansky SA, Hoover CI, Li L, Weintraub JA, White JM. Cariogenic bacteria trends in a randomized caries management clinical trial. J Dent Res. 2002;81:A-467. Abstract 3813.
- Anderson MH. A review of the efficacy of chlorhexidine on dental caries and the caries infection. J Calif Denta Assoc. 2003;31:211-214.