Simple Solutions for Breath Malodor
A thorough understanding of the pathogenesis of breath malodor, as well as strategies for its assessment and management arm clinicians with the tools needed to address this common problem.
This course was published in the January 2015 issue and expires January 31, 2018. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Discuss the epidemiology and pathogenesis of breath malodor.
- Identify the classifications of breath malodor.
- List the strategies for assessing this common problem.
- Explain solutions for managing breath malodor.
Halitosis, bad breath, and oral malodor are terms used for breath malodor. While a matter of semantics, recognizing the difference between bad breath and oral malodor is important. The former may have origins in sites other than the mouth, while oral malodor starts in the oral cavity. Dental professionals play the greatest role in managing oral malodor, which is the primary focus of this review.
The semantic argument for the use of the terms halitosis, bad breath, and oral malodor is of clinical relevance because oral malodor is a restrictive term that should not be confused with odor arising from recent food ingestion, smoking, alcohol consumption, extraoral sources, or psychological conditions. Oral malodor should also not be confused with morning breath malodor, which is generally transient upon waking, arises from decreased salivary flow during sleep, and generally disappears after breakfast and morning oral hygiene regimens. Oral malodor is the most common form of halitosis and is associated mainly with the presence of volatile sulfur compounds that have a particularly acrid smell and are produced by oral bacteria.1–3
Oral malodor is considered a symptom rather than the outcome of a specific pathologic process. Surprisingly, this important and often debilitating condition continues to be poorly understood and is generally overlooked by the dental profession. Despite a large body of literature on the topic, little is known about oral malodor’s epidemiology and impact on quality of life. There are few, if any, evidence-based systematic reviews with meta-analyses on the management of oral malodor.
![Halitosis]() EPIDEMIOLOGY
EPIDEMIOLOGY
The incidence of chronic breath malodor is poorly understood. The incidence of halitosis ranges from 2% to 30% of the world’s population, according to a number of studies.4–7 Evidence indicates that 25% to 40% of the population of industrialized countries experience this condition.8 Nearly 90% of breath malodor cases arise from the oral cavity and are associated with poor oral hygiene, gingivitis, periodontitis, dental caries, and tongue coatings.8 Of the remaining cases, sinus or gastrointestinal problems account for around 5%, and other etiologies (5%) account for the remainder.8
CLASSIFICATION
A classification for breath malodor originally described in Japan in 1999 by Miyazaki et al9 was subsequently presented in English by Yaegaki and Coil.10 This classification categorizes breath malodor as temporary, intraoral, extraoral, pseudo, or halitophobia (Table 1). Such classifications support rational treatment decisions based on the overall diagnosis of the condition. Of these conditions, the most important distinction is between intraoral and extraoral breath malodor, as these represent the presence of legitimate breath malodor. Intraoral breath malodor is used to describe those cases where the source of the problem can be found within the oral cavity, including tongue coating and pathologic conditions, such as gingivitis, periodontitis, ulcers, and dental caries. Extraoral breath malodor is subdivided into bloodborne and nonbloodborne. The terms pseudhalitosis and halitophobia describe conditions in which patients believe they have breath malodor, but no such condition can be confirmed following clinical assessment. The condition of temporary breath malodor is generally associated with consuming various types of food or drink or tobacco use.
PATHOGENESIS
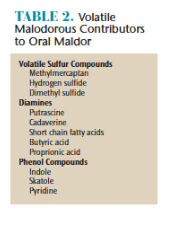
Oral malodor is caused principally by the degradation of organic material by some of the anaerobic bacteria associated with periodontal diseases.11–13 These bacteria produce the bad smell, which is composed of volatile sulfur compounds, diamines, and phenyl compounds (Table 2).3,14 Of these, the volatile sulfur compounds have been most extensively studied and include methylmercaptan, hydrogen sulfide, and dimethyl sulfide. Evidence suggests that oral malodor is associated with elevated levels of methylmercaptan and hydrogen sulfide, while breath malodor from nonoral sources may be associated with dimethyl sulfide—another volatile sulfur compound.15
The bacteria mostly responsible for the production of methylmercaptan and hydrogen sulfide are associated with the subgingival biofilm present in gingivitis and periodontitis, although they are also found on the dorsum of the tongue. Some studies have suggested that, in addition to periodontal diseases, oral malodor is directly related to the total bacterial load in both saliva and tongue coatings.16,17
ASSESSMENT
A thorough history, both medical and dental, is an essential starting point when assessing patients for breath malodor. The medical history should include questions relating to current medications, nasal and sinus conditions, snoring and sleep apnea, mouth breathing, throat infections, tonsilloliths, and an assessment of ingestion of foods that may contribute to breath malodor.
The dental history should focus on whether general dental care has been maintained through regular dental visits and oral hygiene practices, including frequency of tooth brushing and the use of other oral hygiene aids, such as dental floss, interdental cleaning aids, mouthrinses, and tongue cleaners/scrapers. Specific questions relating to the oral malodor must also be addressed, such as how long the problem has been present, whether it is worse at a particular time of day, and whether anyone has commented on the problem.
Following the initial interview, both an oral evaluation and breath analysis are required.18 The oral evaluation should include an assessment of the tonsils, oral debris, caries, exposed pulps, extraction wounds, interdental food impaction, gingivitis, periodontitis, necrotizing periodontal conditions, peri-implantitis, pericoronitis, and recurrent oral ulcerations.
An assessment of tongue coating is also an integral part of the oral assessment for breath malodor. An index for assessing tongue coatings has been used in which the dorsum of the tongue is divided into six sections (Figure 1).19 The presence of any tongue coating is then graded and recorded for each of the sections. If there is no coating present, a score of 0 is given; a light-thin coating is given a score of 1; and a heavy-thick coating is given a score of 2. A score is thus calculated by adding all six section scores, obtaining a total score that ranges from 0 to 12.
An assessment of the quantity and quality of saliva is also important. A consequence of reduced saliva and dry mouth is increased bacterial growth due to the absence or reduction of the antibacterial properties of saliva. With the increased bacterial load, there is an associated increase in the release of volatile sulfur compounds and, thus, an increase in oral malodor.
After the oral examination, a breath odor evaluation is conducted. There are numerous ways in which this can be done, including organoleptic (smelling patient’s exhaled breath) or the use of instruments.
INSTRUMENTAL ASSESSMENT

While there are many methods for assessing breath malodor, instrumental analysis for the presence of volatile sulfur compounds is recommended because it provides a degree of objective assessment.20,21 A variety of devices are available, but one is able to distinguish the three major volatile sulfur compounds (hydrogen sulfide, methylmercaptan, and dimethyl sulfide) associated with halitosis. Sample collection is achieved by placing a disposable syringe in the mouth with the lips sealed for 30 seconds, with the contents then injected into a chromatograph. Analysis takes 8 minutes, after which a printout is produced depicting the levels of the three volatile sulfur compounds. This provides immediate assessment of whether the source of the oral malodor is likely due to the oral cavity or elsewhere.
MANAGEMENT
The treatment options for breath malodor can be divided into six categories (Table 3).10,18 Temporary, intraoral, and pseudo halitosis can be managed by oral health care professionals. However, both extraoral halitosis and halitophobia will require the assistance of physicians, psychiatrists, and psychologists.
Oral malodor is suspected if elevated levels of hydrogen sulfide and methylmercaptan are present. Conversely, an extraoral source of breath malodor is likely if dimethyl sulfide readings are high.15 Once a diagnosis of oral malodor (as distinct from breath malodor) is made, treatment of the oral condition can commence. Ideally, this will be cause-related, involving a multistep approach. If temporary breath malodor is suspected, then assessment and management of dietary components are essential to eliminate the intake of smelly foods, such as garlic, onions, and alcohol. This initial aspect of management should be followed for all five breath malodor classifications. In addition, all dental diseases—including gingivitis, periodontitis, ulcers, and dental caries—must be diagnosed and effectively managed.
The overriding principle for management of intraoral breath malodor is reducing the bacterial burden. An effective and regular oral hygiene regimen (brushing and interdental cleaning) must be instituted and include twice- daily tongue cleaning.20,22,23 Due to the potential damage to the tongue surface, some authors do not recommend tongue scraping and prefer gentle brushing with a small, soft-bristle brush.10 Use of a proven antibacterial toothpaste is recommended.
 Rendering malodorous gases nonvolatile should also be an aim in the management of oral malodor and can be achieved through several means. Increasing saliva flow boosts the solubility of volatile sulfur compounds and can lead to some reduction in the malodor. Drinking water frequently can reduce malodor for an hour. Mouthrinses may be of some value. The adjunctive use of antiseptic mouthrinses is essential to ensure a satisfactory outcome in the management of oral malodor.24,25 While chlorhexidine remains the gold standard for chemical plaque control, it is best used short-term. Emerging evidence suggests that formulations with cetylpyridinium chloride, zinc ions, or essential oils may be helpful.26–29 These formulations work by reducing the overall bacterial load and also have a dilution effect on the malodor. The addition of zinc is particularly interesting because it appears to have both an antibacterial effect and the ability to neutralize volatile sulfur compounds.30 Therefore, mouthrinses and toothpastes containing zinc are emerging as helpful tools in the management of oral malodor.
Rendering malodorous gases nonvolatile should also be an aim in the management of oral malodor and can be achieved through several means. Increasing saliva flow boosts the solubility of volatile sulfur compounds and can lead to some reduction in the malodor. Drinking water frequently can reduce malodor for an hour. Mouthrinses may be of some value. The adjunctive use of antiseptic mouthrinses is essential to ensure a satisfactory outcome in the management of oral malodor.24,25 While chlorhexidine remains the gold standard for chemical plaque control, it is best used short-term. Emerging evidence suggests that formulations with cetylpyridinium chloride, zinc ions, or essential oils may be helpful.26–29 These formulations work by reducing the overall bacterial load and also have a dilution effect on the malodor. The addition of zinc is particularly interesting because it appears to have both an antibacterial effect and the ability to neutralize volatile sulfur compounds.30 Therefore, mouthrinses and toothpastes containing zinc are emerging as helpful tools in the management of oral malodor.
Probiotics have been proposed as useful adjuncts in the management of both intraoral and extraoral breath malodor.31 The use of probiotics for oral malodor is based on the bacterial origin of this condition.32 Thus, controlling the reappearance of odiferous bacteria following conventional mechanical cleaning by the introduction of nonodiferous, commensal bacteria to colonize the oral cavity is an attractive proposal.32 To date, the results of studies investigating the use of probiotics as an adjunctive aid for management of oral malodor have been equivocal and are not universally accepted as a proven method to control oral malodor.33,34
The use of agents that merely mask the offensive smell of oral malodor are generally of limited value. These agents include mouthrinses, sprays, lozenges, and chewing gums. While these will most likely have short-term effects, they are not a definitive treatment and may delay correct diagnosis.
An extraoral source of breath malodor is usually suspected if dimethyl sulfide readings are high.15 In these cases, additional assessment and tests are required. If deemed appropriate, referral to a physician specializing in management of nasal, throat, or gastrointestinal abnormalities may also be required. These may also be accompanied by blood tests for kidney insufficiency, liver insufficiency/dysfunction, and metabolic diseases.
CONCLUSION
The management of oral malodor is not the most glamorous aspect of dentistry, but it is a fascinating and important aspect of patient care. For many patients, oral malodor is a significant problem that affects their quality of life. Through the use of modern technology and the increased understanding of the role certain bacteria play in oral malodor, the management of this condition is becoming more predictable.
REFERENCES
-
- Delanghe G, Ghyselen J, Feenstra L, van Steenberghe D. Experiences of a Belgian multidisciplinary breath odour clinic.Acta Otorhinolaryngol Belg. 1997;51:43–48.
- Delanghe G, Ghyselen J, van Steenberghe D, Feenstra L. Multidisciplinary breath-odour clinic. Lancet. 1997;350:187.
- Tonzetich J. Production and origin of oral malodor: a review of mechanisms and methods of analysis. J Periodontol. 1977;48:13–20.
- Söder B, Johansson B, Söder PO. The relation between foetor ex ore, oral hygiene and periodontal disease. Swed Dent J. 2000;24:73–82.
- Miyazaki H, Sakao S, Katoh Y, Takehara T. Correlation between volatile sulphur compounds and certain oral health measurements in the general population. J Periodontol. 1995;66:679–684.
- Liu XN, Shinada K, Chen XC, Zhang BX, Yaegaki K, Kawaguchi Y. Oral malodor related parameters in the Chinese general population. J Clin Periodontol. 2006;33:31–36.
- Nadanovsky P, Carvalho LB, Ponce de Leon A. Oral malodour and its association with age and sex in a general population in Brazil. Oral Dis. 2007;13:105–109.
- Zalewska A, Zatoñski M, Jabłonka-Strom A, Paradowska A, Kawala B, Litwin A. Halitosis–a common medical and social problem. A review on pathology, diagnosis and treatment. Acta Gastroenterol Belg. 2012;75:300–309.
- Miyazaki H, Arao M, Okamura K, et al. Tentative classification of halitosis and its treatment needs (Japanese). Niigata Dental Journal. 1999;32:7–11.
- Yaegaki K, Coil JM. Examination, classification, and treatment of halitosis; clinical perspectives. J Can Dent Assoc. 2000;66:257–261.
- Loesche WJ, Kazor C. Microbiology and treatment of halitosis. Periodontol 2000. 2002;28:256–279.
- Persson S, Edlund MB, Claesson R, Carlsson J. The formation of hydrogen sulfide and methyl mercaptan by oral bacteria. Oral Microbiol Immunol. 1990;5:195–201.
- McNamara TF, Alexander JF, Lee M. The role of microorganisms in the production of oral malodor. Oral Surg Oral Med Oral Pathol. 1972;34:41–48.
- Scully C, Greenman J. Halitology (breath odour: aetiopathogenesis and management). Oral Dis. 2012;18:333–345.
- Tangerman A, Winkel EG. Volatile sulfur compounds as the cause of bad breath: a review. Phosphorous, Sulfur and Silicon. 2013;188:396–402.
- Tonzetich J, Kestenbaum RC. Odour production by human salivary fractions and plaque. Arch Oral Biol. 1969;14:815–827.
- De Boever EH, Loesche WJ. Assessing the contribution of anaerobic microflora of the tongue to oral malodor. J Am Dent Assoc. 1995;126:1384–1393.
- Seemann R, Conceicao MD, Filippi A, et al. Halitosis management by the general dental practitioner—results of an international consensus workshop. J Breath Res. 2014;8:017101.
- Winkel EG, Roldán S, Van Winkelhoff AJ, Herrera D, Sanz M. Clinical effects of a new mouthrinse containing chlorhexidine, cetylpyridinium chloride and zinc-lactate on oral halitosis. A dual-center, double-blind placebo-controlled study. J Clin Periodontol. 2003;30:300–306.
- Dadamio J, Laleman I, De Geest S, et al. Usefulness of a new malodour-compound detection portable device in oral malodour diagnosis. J Breath Res. 2013;7:046005.
- Laleman I, Dadamio J, De Geest S, Dekeyser C, Quirynen M. Instrumental assessment of halitosis for the general dental practitioner. J Breath Res. 2014;8:017103.
- van den Broek AM, Feenstra L, de Baat C. A review of the current literature on management of halitosis. Oral Dis. 2008;14:30–39.
- Outhouse TL, Al-Alawi R, Fedorowicz Z, Keenan JV. Tongue scraping for treating halitosis. Cochrane Database Syst Rev. 2006;2:CD005519.
- Quirynen M, Zhao H, Soers C, et al. The impact of periodontal therapy and the adjunctive effect of antiseptics on breath odor-related outcome variables: a double-blind randomized study. J Periodontol. 2005;76:705–172.
- Quirynen M, Zhao H, van Steenberghe D. Review of the treatment strategies for oral malodour. Clin Oral Investig. 2002;6:1–10.
- Young A, Jonski G, Rölla G. Combined effect of zinc ions and cationic antibacterial agents on intraoral volatile sulphur compounds (VSC). Int Dent J. 2003;53:237–242.
- Winkel EG, Roldán S, Van Winkelhoff AJ, Herrera D, Sanz M. Clinical effects of a new mouthrinse containing chlorhexidine, cetylpyridinium chloride and zinc-lactate on oral halitosis. A dual-center, double-blind placebo-controlled study. J Clin Periodontol. 2003;30:300–306.
- van Steenberghe D, Avontroodt P, Peeters W, et al. Effect of different mouthrinses on morning breath. J Periodontol. 2001;72:1183–1191.
- Fine DH, Furgang D, Sinatra K, Charles C, McGuire A, Kumar LD. In vivo antimicrobial effectiveness of an essential oil-containing mouth rinse 12 h after a single use and 14 days’ use. J Clin Periodontol. 2005;32:335–340.
- Dadamio J, Van Tournout M, Teughels W, Dekeyser C, Coucke W, Quirynen M. Efficacy of different mouthrinse formulations in reducing oral malodour: a randomized clinical trial. J Clin Periodontol. 2013;40:505–513.
- Burton JP, Chilcott CN, Moore CJ, Speiser G, Tagg JR. A preliminary study of the effect of probiotic Streptococcus salivarius K12 on oral malodour parameters. J Appl Microbiol. 2006;100:754–764.
- Teughels W, Van Essche M, Sliepen I, Quirynen M. Probiotics and oral healthcare. Periodontol 2000. 2008;48:111–147.
- Masdea L, Kulik EM, Hauser-Gerspach I, Ramseier AM, Filippi A, Waltimo T. Antimicrobial activity of Streptococcus salivarius K12 on bacteria involved in oral malodour. Arch Oral Biol. 2012;57:1041–1047.
- Suzuki N, Yoneda M, Tanabe K, et al. Lactobacillus salivarius WB21—containing tablets for the treatment of oral malodor: a double-blind, randomized, placebo-controlled crossover trial. Oral Surg Oral Med Oral Pathol Oral Radiol. 2014;117:462–470.
From Dimensions of Dental Hygiene. January 2015;13(1):56–58,61.


 EPIDEMIOLOGY
EPIDEMIOLOGY