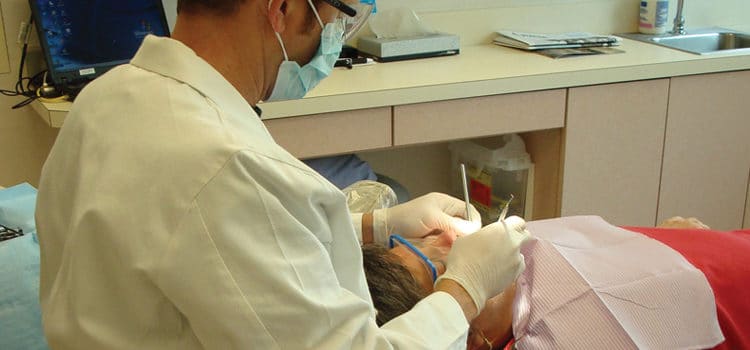
Seating, Positioning, and Lighting
Keep your body injury-free with these cornerstones of ergonomics.
 The oral cavity is challenging because it is small and narrow and limits dental hygienists’ field of vision. This encourages them to work in awkward, inflexible positions to facilitate a better visual working area.1,2 During the static posture, the body is forced to use half of its muscles to contract and hold the position. Prolonged endurance of static postures may result in musculoskeletal disorders (MSDs) such as chronic lower back pain, tension neck syndrome, muscle imbalances, joint hypomobility, spinal disk degeneration, and ultimately a career-ending injury.1,2
The oral cavity is challenging because it is small and narrow and limits dental hygienists’ field of vision. This encourages them to work in awkward, inflexible positions to facilitate a better visual working area.1,2 During the static posture, the body is forced to use half of its muscles to contract and hold the position. Prolonged endurance of static postures may result in musculoskeletal disorders (MSDs) such as chronic lower back pain, tension neck syndrome, muscle imbalances, joint hypomobility, spinal disk degeneration, and ultimately a career-ending injury.1,2
Dental hygienists may reduce the risk of developing MSDs by developing a healthy working posture. Clinicians should begin by evaluating their individual postures.3,4 Marklin et al completed a study to measure occupational postures of dentists and dental hygienists in which they observed the postures while the practitioners treated patients during 4-hour periods. This study found that the postures of the trunk, shoulders, and neck remained primarily static for the clinicians during treatment.5 To evaluate posture, a sophisticated assessment tool such as the Branson’s Posture Assessment Instrument (BPAI) may be used or a coworker can take pictures or video tape of the operator’s posture while working on patients throughout the day.4 Because many areas in the oral cavity are not easily accessible through direct vision, clinicians tend to turn their heads and bend and twist the back into an awkward position to help view. These continued extensions of the body place strain on the muscles and eventually lead to muscle imbalances.
When getting in a healthy posture, clinicians need to adjust their chairs first and then position the patient back. Dental hygienists often make the mistake of positioning their patients first and then positioning the operator stool.6 For the practitioner, the optimal sitting position is a neutral working posture, which allows for endurance and reduces the potential for overexertion and injury.7
The neutral working position encourages the clinician to sit with the back and the spinal cord straight, weight evenly balanced, forearms and thighs parallel to the floor, and the hips at a 90° angle. The seat height should be positioned low enough so you are able to rest the heels of your feet on the floor.11 Adjust the operator chair so that the hips are slightly higher than the knees and distribute weight evenly by placing both feet firmly flat on the floor. Do not sit on the edge of the chair. This can compress the backs of your thighs and reduce blood flow. Equally important, shoulders should be relaxed and parallel with the hips and the floor, while the elbows should remain close to the body.6,7
To maintain a straight back, adjust and use the lumbar support of the chair. Also, if the chair has arm rests, adjust them to support elbows in the neutral shoulder position; this will help to decrease neck and shoulder strain.
Patient/Operator Positioning
When seating a patient, a common mistake is for clinicians to place the patient’s chair height too high.6,8 This may cause the clinician’s shoulders to elevate and create an abduction of the arms, leading to abnormal position and tension in these muscle groups. Ideally the dental hygienist should adjust the patient’s headrest until the patient’s mouth is at the clinician’s elbow height; this results in the patient’s oral cavity being approximately 15 to 22 inches from the clinician’s eyes.7 Operators may vary placement of patients in a semi-supine position for mandibular procedures and in a supine position for maxillary procedures, or use a chin-up and chin-down method when working on different arches.9,11
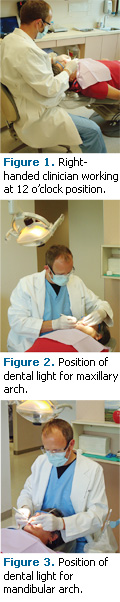
Varying positions shifts work to other muscle groups.6 Different positions also provide clinicians with more options for vision in the working area. When a patient is in normal supine position and the clinician, depending on dominance of hand, changes working position to gain better access into the oral cavity, the optimal range of movement for a righthanded clinician is 8 o’clock to 12 o’clock and 4 o’clock to 12 o’clock for left-handed practitioners. Clinicians should maintain the neutral working posture and operate in different locations around the oral cavity in order to gain better access.7,8 By using the clinician’s stool to navigate around the patient instead of bending and twisting, the dental hygienist can avoid static posture, gain better visual adjustments, and avoid MSDs. Figure 1 shows a right-handed clinician working at a 12 o’clock position.
Dental Light Positioning
The dental light is one of the most simple adjustments to make that can help prevent MSDs for dental hygienists. Poor and inadequate lighting can lead to eyestrain and headache.3 The dental light should be as far above the patient’s head as possible while within the easy reach of the clinician. When instrumenting in the maxillary arch, the dental light is best positioned above the patient’s chest, tilted so that the beam shines into the oral cavity at an angle (Figure 2).8 The dental light should be placed directly above the patient’s head when instrumenting on the mandibular arch (Figure 3), allowing for the beam to shine directly onto the working area.8
Co-axial headlights are another option for dental hygienists. When selecting a coaxial headlight, the adjustment of brightness, beam uniformity, and weight should be considered.
The correct lighting allows the clinician to see better without feeling the need to bend, twist, or turn. Sufficient lighting is another essential tool for preventing potential pain and compromising injury.
| Additional Tips |
| Remember correct posture, smart patient-operator positioning, and correct use of the dental light are significant allies in preventing MSDs. Other small day-to-day activities that can also aid in preventing pain and injury. Keep your instruments within reach so you’re not reaching and/or twisting repeatedly throughout the day.9 If you must reach for something, pivot from your hips, not your waist. Try to take periodic breaks so that your muscles are not kept in a static position for long periods throughout the working day. However, if taking mini-breaks are not feasible in your fastpaced office, try to stretch between patients and at the end of the day. Away from the office there are also activities that can help reduce the risk of getting MSDs such as strengthening and aerobic exercises. These exercises help by building and maintaining healthy muscle strength and tone. By practicing preventive measures you can reduce the chances of suffering from MSDs and continue to practice as a healthy dental hygienist.6,9 |
References
- Valachi B, Valachi K.Mechanisms Leading to musculoskeletal disorders in dentistry. J Am Dent Assoc. 2003;134:1344-1350.
- Finsen L, Christensen H, Bakke M. Musculoskeletal disorders among dentists and variation in dental work. Appl Ergon. 1998;29:119-125.
- Michalak-Turcotte C. Controlling dental hygiene work-related musculoskeletal disorders: the ergonomic process. J Dent Hyg. 2000;74:41-48.
- Simmer-Beck M, Branson B. Posture perfect. Dimensions of Dent Hygiene. 2005;3(5):14, 16-19.
- Marklin RW, Cherney K. Working postures of dentists and dental Hygienists. J Calif Dent Assoc. 2005;33:133-136.
- Valachi B, Valachi K. Preventing musculoskeletal disorders in clinical dentistry. J Am Dent Assoc. 2003;134:1604-1612.
- Wilkins E. Clinical Practice of the Dental Hygienist. 10th ed. Philadelphia: Lippincott Williams & Wilkins; 2008:85-97.
- Nield-Gehrig JS. Fundamentals of Periodontal Instrumentation and Advanced Root Instrumentation. 5th ed. Philadelphia: Lippincott Williams & Wilkins; 2004:14-41.
- Liskiewicz ST, Kerschbaum WE. Cumulative trauma disorders: an ergonomic approach for prevention. J Dent Hyg. 1997;71:162-167.
From Dimensions of Dental Hygiene. September 2008; 6(9):36-37.

