
Radiography Revelations
How the use of panoramic radiography may help identify calcified carotid artery atheromas.
Hardening of the arteries or atherosclerosis is a common inflammatory disorder of immunological origin.1 Atherosclerotic plaques are caused by the build up of fat, cholesterol, and other substances in the walls of the arteries.2 Atherosclerotic disease can occur along the walls of the common carotid artery near its bifurcation. This arterial stenosis, or constriction, has been explored as one of many risk factors for stroke.3 When these types of atherosclerotic lesions become significantly calcified, they can sometimes be seen on a panoramic radiograph.4
From 2005 to 2006, 29.5 million panoramic radiographs were taken in American dental practices. 5 Although not recommended as a primary means of identifying and evaluating carotid artery calcification, the American Dental Association Council on Scientific Affairs asserts that panoramic radiographs taken during the dental appointment should also be evaluated for this condition. Although there is considerable debate about the significance of calcified carotid artery atheromas, oral health practitioners should be able to recognize them on a panoramic radiograph, understand associated risk factors, educate patients, and refer patients to their primary care physician for appropriate examination and follow-up.1,2,6,7
BACKGROUND
Cerebrovascular accident (stroke) is a specific type of cardiovascular disease affecting the arteries leading to and within the brain. Stroke can occur when a blood vessel carrying oxygen and nutrients to the brain becomes compromised and circulation is impeded. Strokes are defined either as an ischemic attack, where a vessel becomes blocked, or as an intracerebral hemorrhage, where a blood vessel in the brain bursts and the blood leaks into the brain. Deprived of necessary oxygen, brain tissue necrosis can begin.8 Each year, approximately 795,000 people experience a new or recurrent stroke, making it the fourth leading cause of death in the United States. Of all strokes, 87% are ischemic and 10% are intracerebral hemorrhage.9
RISK FACTORS
Accelerated atherosclerosis exacerbates the prevalence of stroke and a number of other conditions, including coronary artery disease, heart failure, and peripheral arterial disease.10 Diabetes mellitus, obesity, high blood pressure, smoking, alcoholism, chronic renal disease, and menopause are high-risk conditions associated with atherosclerosis. Sedentary lifestyle, stress, radiotherapy of the head and neck, obstructive sleep apnea syndrome, advanced age, and male gender are also related to a lesser degree.11
Diabetes is a powerful and independent risk factor for coronary artery disease, stroke, and peripheral artery disease. A major complication of this metabolic disease is accelerated atherosclerosis and microvascular disease.12–14 This complex disease is often diagnosed among those older than 40 with metabolic and vascular manifestations. Patients with poorly controlled diabetes tend to develop an advanced form of vascular disorder—affecting both small blood vessels (microvascular disease) and large blood vessels (macrovascular disease).15,16 Macrovascular disease characterized by atherosclerotic changes is the major cause of morbidity and mortality in type 2 diabetes.15,16 Effects include angina and myocardial infarction, gangrene in the lower extremities, and carotid artery-associated stroke. Atherosclerosis of the cervical portion of the carotid artery in people with type 2 diabetes is caused by associated hyperglycemia, hyperlipidemia, and hypertension.15,16
A national epidemic in the US, obesity may increase the level of triglycerides and low density lipoproteins (LDL) in the blood. Blood levels of high density lipoproteins (HDL) may be reduced. Resulting accumulation of fatty substances on vascular walls increases susceptibility to atherosclerosis.1
Increased arterial pressure has deleterious effects on the endothelium. Hypertension-induced atherosclerosis is related to an increase in LDL in the intimae (endothelial wall). These LDLs promote or exacerbate endothelial dysfunction.17 Associated inflammation of the vascular endothelial lining plays a major role in the origin and development of atherosclerosis and arterial hypertension.18
Cigarette smoking is a major risk factor for stroke.19 Chronic smoking is associated with functional and structural vascular changes that contribute to the development of plaque formation and rupture observed in stroke.20 Smoking may increase the risks of damage to arterial wall lining and raise the risk of arterial contractions that reduce the blood supply to the tissues by elevating carbon monoxide in the blood. Smoking increases LDL cholesterol and reduces HDL cholesterol.21
Alcohol consumption may affect cardiovascular health negatively or positively. This cause-effect association differs by stroke subtype—slightly lowering the risk of ischemic stroke, but raising the risk of hemorrhagic stroke.22 Hypertension and coagulation disorders caused by alcohol use, as well as alcohol’s anticoagulant effects, may increase the risk of hemorrhagic stroke.23 Heavy alcohol consumption is associated with a high prevalence of atheromatous plaques. Conversely, slight to moderate intake of alcohol appears to increase HDL cholesterol, decrease LDL cholesterol, inhibit platelet function, decrease coagulation activity, and increase fibrinolysis activity.24
Atherosclerosis is a common feature of chronic kidney disease. Chronic renal disease promotes hypertension and dyslipidemia and increases the risk of endothelial dysfunction and progressive atherosclerosis. 25 Arterial calcification, a complication of end-stage renal disease, is a strong predictor of cardiovascular disease.26,27 A high prevalence of carotid artery calcification on dental panoramic radiographs has been reported on end-stage renal disease patients undergoing hemodialysis and renal transplant.27 Higher mortality rates among these patients may be associated with an increased occurrence of occlusive lesions and generalized atherosclerosis.27
As women age, risk factors for atherosclerosis may increase, including poor lipid profile and weight gain. Menopausal decrease in estrogen levels has been linked to endothelial dysfunction and susceptibility to associated adverse vascular changes.1 Studies have reported the risk of stroke resulting from atherosclerosis of the carotid artery increases in post-menopausal women.28,29 Reduced levels of circulating estrogen are associated with an increase in hepatic lipase activity and a decrease in LDL catabolism. Atherogenic risk factors observed in post-menopausal women include an increase in total cholesterol levels, decrease in HDL levels, increase in thrombic tendency, and the occasional development of insulin resistance.29,30
Although associated with the process of aging, atherosclerosis may be seen in younger individuals with elevated cholesterol.31 A number of factors can injure the vascular endothelium including abnormal metabolic, hypertensive, or nutritional events and both viral and bacterial infection. Pathology occurs when the inflammatory environment promotes an accumulation of LDL cholesterol and superimposition of calcium deposits in the intimate layer of the endothelium. Platelets, T lymphocytes, macrophages, smooth muscle cells, adhesion molecules and genetic components then interact, forming atheromatous plaque.1,32
RECOGNITION AND REFERRAL
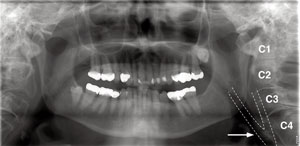
Calcified plaques (atheromas) formed at the bifurcation of the internal and external carotids can be seen on panoramic radiography. The image of the atheroma may appear as an irregular-shaped radiopaque mass or as a radiopaque vertical line located approximately 2.5 cm posterior to inferior and posterior to the angle of the mandible, adjacent to the space between vertebrae C3 and C4 (Figure 1). This anatomical region is frequently viewable in the properly positioned panoramic radiograph.33 Panoramic radiographs should not be taken as the primary screening tool for this condition. Because many panoramic radiographs are taken each year to facilitate diagnosis of dental conditions, secondary findings of calcification in field of view should not be ignored.6
Over the past two decades, the significance of panoramic radiographs in the diagnosis of calcified carotid atheroma artery as a risk for stroke has been highly discussed and remains controversial. Although digital imaging offers the ability to adjust brightness and contrast and zoom in on specific areas, studies have been conducted using both digital and conventional film-based technology. While panoramic radiography may have a function in identifying an atheroma, it is not useful in determining the exact location and degree of occlusion.2 Considered the “gold standard” of noninvasive diagnostic techniques, ultrasonography is necessary to determine calcification and stenosis of extracranial carotid vasculature in patients with atherosclerotic disease.3
The current literature does not draw a consistent correlation between calcified carotid atheroma and occurrence of stoke. Mupparapu et al performed a critical review of the literature using 11 databases to evaluate evidence linking calcified carotid artery atheroma seen in panoramic radiographs to increased precipitation of stroke. Their findings indicate that “panoramic radiography may demonstrate that carotid artery atheromas calcify over time, but that there is little evidence-based information that [such atheromas] are risk predictors for the diagnosis of cerebrovascular disease”.7 Thus, the utility of using panoramic radiographs to detect calcified carotid atheromas is limited due to the high potential for false positive.7 More case-controlled or cohort studies that include control subjects are needed to prove the association between calcified carotid atheroma and occurrence of stoke, as well as the significance of panoramic radiographs as a diagnostic tool.7
Some authors suggest that clinicians should not estimate the risk of stroke with incidental finding of atheroma in the carotid artery alone, but rather consider a more comprehensive set of factors such as age, smoking, cholesterol levels, and hypertension to assess a patient’s risk for stroke.7 Dental hygienists review their patients’ health histories on a regular basis, which provides an opportunity to recognize and offer counseling on many of the oralsystemic risk factors noted above.
By understanding and examining these risk factors, in addition to observing the possible association of radiographic findings and atherosclerotic disease, oral health clinicians may be better able to identify patients at high risk of experiencing stroke and refer them accordingly to minimize the incidence cerebrovascular accidents. Strong, active interprofessional partnerships may offer patients who are at increased risk the most ideal care.
CASE REPORT
A 78-year-old woman who was receiving regular comprehensive dental care expressed concern about the appearance of her severely crowded anterior dentition, which also created significant challenges during oral self-care. No other dental concerns were reported. The patient’s health history indicated hypertension, overweight, and elevated cholesterol levels, which were controlled by diet and medication. Family history revealed maternal death due to cerebrovascular accident. A panoramic radiograph, taken in anticipation of orthodontic consultation, revealed bilateral radiopaque nodules in the area of the carotid bifurcation (Figure 2).
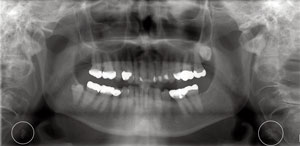
Given the patient’s health history and combined risk factors, the general dentist consulted with a maxillofacial radiologist. The resulting radiographic interpretation confirmed bilateral appearance of calcification in the carotid area. Further evaluation was recommended as such calcifications might suggest atheromas in the carotid arteries. Collateral, unrelated radiographic findings indicated external resorption in the coronal aspect of impacted 16 and 32, degenerative joint disease in the cervical spine, and temporomandibular joints within normal limits. After examination, the patient’s primary care physician advised that, although carotid bruits (sound of blood pulsing heard over the carotid artery area while listening with a stethoscope) were noted, no other symptoms were present, thus no further treatment was recommended. Two years later, in consultation preliminary to minor surgery, bruits were again found by the patient’s general surgeon. Follow-up carotid ultrasound study was recommended.
Subsequent test results noted moderate plaque bilaterally in the internal carotid arteries with 50% to 70% stenosis. The patient continued to be asymptomatic. Noting the patient’s combined risk factors, family history, and ultrasound findings, the surgeon recommended a 6-month follow-up. The patient was advised that if blockage increased and/or symptoms developed, the placement of a stent might be recommended.
CONCLUSION
Among dental hygiene’s core competencies are health promotion and disease prevention.34 Dentists and dental hygienists are trained to recognize high risk groups and individual risk factors through medical history and oral and systemic findings. As members of the health care team, they play an important role in developing strategies to help patients achieve and maintain optimum oral and systemic health. Recognition of panoramic findings related to carotid artery calcification, in combination with associated systemic risk factors, is important. Findings should be explored with patients to determine the need for referral to a physician for definitive diagnosis, treatment, and follow-up as needed. As with all developing research, oral health care providers should continue to follow ongoing literature in this area in order to make the best possible evidence-based interprofessional referrals on behalf of their patients.
REFERENCES
- Guimarães Henriques JC, Kreich EM, Helena Baldani M, Luciano M, Cezar de Melo Castilho J, Cesar de Moraes L. Panoramic radiography in the diagnosis of carotid artery atheromas and the associated risk factors. Open Dent J. 2011;5:79–83.
- Manzi FR, Bóscolo FN, de Almeida SM, Haiter Neto F. Panoramic radiography as an auxiliary in detecting patients at risk for cerebrovascular accident CVA: a case report. J Oral Sci. 2003;45:177–180.
- Madden RP, Hodges JS, Salmen CW, et al. Utility of panoramic radiographs in detecting cervical calcified carotid atheroma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103:543–548.
- Friedlander AH, Garrett NR, Chin EE, Baker JD. Ultrasonic confirmation of carotid artery atheromas diagnosed via panoramic radiography. J Am Dent Assoc. 2005;136:635–640.
- The 2005-2006 Survey of Dental Services Rendered. Chicago: American Dental Association; 2007:35.
- American Dental Association Council on Scientific Affairs. The use of dental radiographs: update and recommendations. J Am Dent Assoc. 2006;137:1304–1312.
- Mupparapu M, Kim IH. Calcified carotid artery atheroma and stroke: a systematic review. J Am Dent Assoc. 2007;138:483–492.
- American Heart Association/American Stroke Association. About Stroke. Available at: www.strokeassociation.org/ STROKEORG/ AboutStroke/ AboutStroke_ UCM_308529_SubHomePage.jsp Accessed November 1, 2012.
- Roger VL, Go AS, Lloyd-Jones DM, et al. Heart disease and stroke statistics–2011 update: a report from the American Heart Association. Circulation. 2011;123:e18–e209.
- Schiffrin EL, Lipman ML, Mann JF. Chronic kidney disease: effects on the cardiovascular system. Circulation. 2007;116:85–97.
- Friedlander AH, Cohen SN. Panoramic radiographic atheroms portent adverse vascular events. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103:830–835.
- Schwartz CJ, Valente AJ, Sprague EA, Kelley JL, Cayatte AJ, Rozek MM. Pathogenesis of the atherosclerotic lesion. Implications for diabetes mellitus. Diabetes Care. 1992;15:1156–1167.
- Stamler J, Vaccaro O, Neaton JD, Wentworth D. Diabetes, other risk factors, and 12-yr cardiovascular mortality for men screened in the Multiple Risk Factor Intervention Trial. Diabetes Care. 1993;16:434–444.
- Basta G, Schmidt AM, De Caterina R. Advanced glycation end products and vascular inflammation: implications for accelerated atherosclerosis in diabetes. Cardiovasc Res. 2004;63:582–592.
- Friedlander AH, Maeder LA. The prevalence of calcified carotid artery atheromas on the panoramic radiographs of patients with type 2 diabetes mellitus. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;89:420–424.
- Andersson DKG, Svardsudd K. Long-term glycemic control relates to mortality in type II diabetes. Diabetes Care. 1995;18:1534–1543.
- Dilic M, Dzubur A, Kusljugic Z, Balic S, Pepic E. Correlation of arterial hypertension and type 2 diabetes mellitus with type of polyvascular atherosclerotic disease. Med Arh. 2010;64:264–268.
- Trepels T, Zeiher AM, Fichtlscherer S. The endothelium and inflammation. Endothelium. 2006;13:423–429.
- Wolf PA, D’Agostino RB, Kannel WB, Bonita R, Belanger AJ. Cigarette smoking as a risk factor for stroke. The Framingham Study. JAMA. 1988;259:1025–1029.
- Kumagai M, Yamagishi T, Fukui N, Chiba M. Long-term cigarette smoking increases the prevalence of carotid artery calcification seen on panoramic dental radiographs in male patients. Tohoku J Exp Med. 2007;212:21–25.
- Pistoia F, Cipollone F, Ferri C, Sarà M, Sudano I, Desideri GB. Cyclooxygenase and atherosclerosis: a smoking area. Curr Pharm Des. 2010;16:2567–2571.
- Ronksley PE, Brien SE, Turner BJ, Mukamal KJ, Ghali WA. Association of alcohol consumption with selected cardiovascular disease outcomes: a systematic review and meta-analysis. BMJ. 2011;342:d671.
- Reynolds K, Lewis B, Nolen JD, Kinney GL, Sathya B, He J. Alcohol consumption and risk of stroke: a meta-analysis. JAMA. 2003;289:579–588. Wakabayashi I. Associations between alcohol drinking and multiple risk factors for atherosclerosis in smokers and nonsmokers. Angiology. 2010;61:495–503.
- Koike M, Nitta K. Chronic kidney disease and atherosclerosis. Nihon Rinsho. 2011;69:144–150.
- Blacher J, Guerin AP, Pannier B, Marchais SJ, London GM. Arterial calcifications, arterial stiffness, and cardiovascular risk in end-stage renal disease. Hypertension. 2001;38:938–942.
- Kansu O, Ozbek M, Avcu N, Genctoy G, Kansu H, Turgan C. The prevalence of carotid artery calcification on the panoramic radiographs of patients with renal disease. Dentomaxillofac Radiol. 2005;34:16–19.
- Rothwell PM, Slattery J, Warlow CP. Clinical and angiographic predictors of stroke and death from carotid endarterectomy: systematic review. BMJ. 1997;315:1571–1577.
- Friedlander AH. The physiology, medical management and oral implications of menopause. J Am Dent Assoc. 2002;133:73–81.
- Kritz-Silverstein D, Barrett-Connor E, Wingard DL. Hysterectomy, oophorectomy, and heart disease risk factors in older women. Am J Public Health. 1997;87:676–680.
- Tuzcu EM, Kapadia SR, Tutar E, et al. High prevalence of coronary atherosclerosis in asymptomatic teenagers and young adults: evidence from intravascular ultrasound. Circulation. 2001;103:2705–2710.
- Hansson GK. Atherosclerosis—an immune disease: the Anitschkov Lecture 2007. Atherosclerosis. 2009;202:2–10.
- Damaskos S, Griniatsos J, Tsekouras N, et al. Reliability of panoramic radiograph for carotid atheroma detection: a study in patients who fulfill the criteria for carotid endarterectomy. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;106:736–742.
- ADEA competencies for entry into the allied dental professions as approved by the 2011 ADEA House of Delegates. Available at: www.adea.org/about_adea/governance/Documents/ADEA%20Competencies%20for%20Entry%20into%20the%20Allied%20Dental%20Professions.pdf. Accessed November 19, 2012.
From Dimensions of Dental Hygiene. December 2012; 10(12): 50–54.

