Preventing the Progression
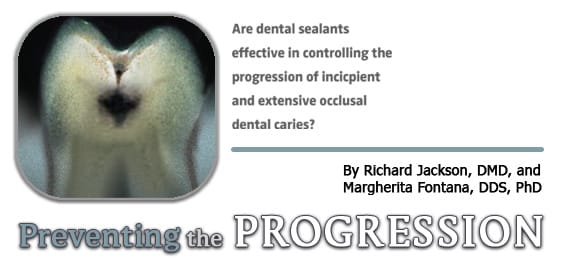
Are dental sealants effective in controlling the progression of incipient and extensive occlusal dental caries?
| To read the authors’ previous article on caries “Maximizing the Benefits of Sealants” by Richard Jackson, DMD, and Margherita Fontana, DDS, PhD, click here. |
The ability to accurately assess whether a carious lesion is static, advancing, or regressing is paramount to determining the best course of treatment. Dental sealants are an effective means for preventing the initiation of dental caries on occlusal surfaces, although the strength of the evidence concerning their true efficacy is open to debate.1-3 A survey of pediatric dentists indicated that among members of the American Academy of Pediatric Dentists, many different selection criteria are used when deciding if a dental sealant is the restoration of choice.4 The criteria include risk status, patient behavior, eruption status, surface status, and how the surface was evaluated clinically (visual/tactile, radiographically, and/or with transillumination).4 While 80% of the respondents indicated that they routinely seal caries-free and questionable occlusal surfaces, only 20% of the respondents reported sealing incipient occlusal caries.4 None indicated that they seal overt caries.4 Is the use of dental sealants a justifiable means of managing incipient caries?
THE CHANGING CARIES PROCESS
Continuing changes in dental caries epidemiology, especially in young children, has increased the practice of placing dental sealants to prevent occlusal dental caries.5-7 In the United States and other developed countries, the introduction and wide scale availability of fluoride from multiple sources, such as dentifrices, over-the-counter and prescription products, and communal water supplies, have resulted in a dramatic decline in the prevalence of smooth surface caries. In comparison to smooth surface caries, the prevalence of occlusal caries has actually increased.5 Because fluoride has its greatest effect on smooth surfaces and a lesser effect on occlusal caries, the percentage of surfaces that actually develop caries is now predominantly occlusal surfaces. Prior to the introduction of fluoride, there was a greater likelihood that caries would affect smooth surfaces as well.
 A second change in the caries process, again as a result of the wide availability of fluoride, is the substantial increase in the time necessary for a carious lesion to progress from early demineralization to frank cavitation.5-6 Clinically detectable carious lesions are increasingly recognized because of an evolving process in which the time a tooth is exposed to demineralizing conditions exceeds the time necessary for remineralization. Based on the environment of the oral cavity, lesions may progress, stabilize, or regress. Understanding the demineralization-remineralization process and identifying the factors that may contribute to it are very important in determining whether a lesion can be restored or if a more conservative treatment, such as placement of a dental sealant, is appropriate.5-6 However, despite their longtime availability, dental sealants do not have clearly established guidelines for their usage.4, 7-9
A second change in the caries process, again as a result of the wide availability of fluoride, is the substantial increase in the time necessary for a carious lesion to progress from early demineralization to frank cavitation.5-6 Clinically detectable carious lesions are increasingly recognized because of an evolving process in which the time a tooth is exposed to demineralizing conditions exceeds the time necessary for remineralization. Based on the environment of the oral cavity, lesions may progress, stabilize, or regress. Understanding the demineralization-remineralization process and identifying the factors that may contribute to it are very important in determining whether a lesion can be restored or if a more conservative treatment, such as placement of a dental sealant, is appropriate.5-6 However, despite their longtime availability, dental sealants do not have clearly established guidelines for their usage.4, 7-9
SEALING INCIPIENT DENTAL CARIES
While many dental practitioners recognize the value of placing dental sealants to prevent the initiation of occlusal dental caries, many feel much less comfortable placing a dental sealant to prevent further disease progression or to enhance disease regression. Many clinicians may opt for a minimally invasive restorative technique or a permanent restoration4, 8-10 despite the fact that a permanent restoration may result in the removal of a substantial amount of healthy tooth structure.11 Therefore, today’s practitioners are routinely faced with the dilemma of determining an appropriate level of care. This decision must be based not only on the actual clinical condition of the surface but also must consider many factors as part of a thorough risk assessment.10, 12 For example, a typical scenario may be: “Although my assessment of this patient is that she is at moderate risk of developing caries in the next few years, several occlusal lesions that I detected at her last visit appear to be progressing, albeit at a slow rate, and they have yet to cavitate. Should I seal these surfaces or place an amalgam restoration?” By definition, a noncavitated lesion has the potential to become arrested and, as a result, possibly remineralize over time given the proper environmental conditions. In this situation, the occlusal surface in question may be a good candidate for a dental sealant or other noninvasive therapy, especially if the patient resides in an area of adequate fluoride accessibility through multiple sources.
RESEARCH RESULTS
The rationale for sealing early incipient dental caries to prevent further progression of the clinical lesion is based a number of published clinical investigations.5-7 The results of these trials have led to the sealing of any fissural lesion confined to the enamel.6,13 Handelman concluded that “caries is inhibited and may in fact regress under intact sealants.” 14, 15 These conclusions were based on investigations conducted using radiographic and bacteriological studies to determine the possible therapeutic use of sealants on teeth that were carious. The data, collected over 2 years, indicated a significant decrease in bacterial counts in teeth that had been sealed with known lesions. Observations suggested that when the sealant remained intact, the lesions did not progress and, in some instances, actually regressed. In teeth where the sealant was partially lost, the pattern of caries progression was modified and did not mirror the rapid progression seen in teeth that were not sealed at all. The failed sealants were not as effective as those that remained intact but the partial retention of the sealant material was sufficient to at least slow the progression of the carious lesion. This finding is significant in cases where behavior management or acute medical conditions may necessitate the delay of definitive treatment.
In 1978, Going et al16 obtained bacteriological samples from teeth that had been sealed for 5 years and found an 89% reversal from a caries-active to a caries-inactive state. The definition of caries-active or inactive was dependent on the number of micro-organisms that were detected in the fissure over time. Going concluded that “these data confirm and extend previous observations that a limited number of cultivable organisms persist in some lesions, but their numbers are few, and they do not appear capable of continuing the destruction of tooth structure.”16
Heller et al17 found in 1995 that initially, sound surfaces were unlikely to become carious in 5 years and did not benefit greatly from the application of sealants. The study was conducted in a fluoridated community. There were, however, clear benefits in applying sealants to incipient caries to prevent further progression. Of the teeth with incipient lesions, 52% that were sealed did not show evidence of progression as compared to only 11% of those that did not receive sealant therapy. 
A recent 1-year clinical trial performed by Florio et al18 also substantiates the claim that placing dental sealants to treat incipient occlusal caries is beneficial. Out of 31 children (mean age 6 years + 6 months) with diagnosed occlusal caries, 98 first permanent molars were assigned to treatment. The three treatment groups included: the use of dental sealants (Group 1), fluoride varnish application (Group 2), and toothbrushing and the weekly use of 0.2% NaF mouthrinse (Group 3). The molars were assessed at baseline, 3, 6, 9, and 12 months through clinical and radiographic evaluation. After 12 months, the sealant group showed 100% arrestment of caries activity compared to 83.3% and 72.7% in groups 2 and 3. In terms of caries progression, Group 1 showed 0% progression, Group 2 showed 5.5%, and Group 3 showed 6.1%. The investigators concluded that while sealant placement had a negligible effect on disease progression, it was the most effective modality tested in reducing caries activity.
The concern with sealing more advanced lesions is that the potential for caries to advance when sealants are lost may be greater than with incipient lesions. A 10-year study by Mertz-Fairhurst et al 19 attempted to prove this hypothesis by evaluating bonded and sealed composite restorations placed directly over frank cavitated lesions extending into dentin. These were compared to sealed conservative amalgam restorations and conventional unsealed amalgam restorations. The teeth were carefully chosen prior to sealant placement, sealed, and then monitored a over a 10-year period. The baseline radiographic images clearly showed that the study teeth had large dentinal lesions. Soft carious material was excavated and a composite resin was placed over the remaining dentin and then sealed. The control groups included standard amalgam restorations and amalgams with a sealant. The results indicated without question that “active caries may become inactive and arrested if adequately sealed from the oral environment.”
In response to concerns on the placement of sealants over detectable enamel lesions, the American Academy of Pediatric Dentistry and the American Dental Association (ADA) issued policy statements.13,20 The ADA Council issued the following statement: “Historically, concern was expressed regarding the potential placement of sealants over known enamel carious lesions. However, substantial data have been collected indicating that lesions (both diagnosed and undiagnosed) at the base of the fissure are arrested by sealant application. Caries-causing bacteria trapped beneath intact resin do not regenerate and enamel lesions do not progress. The decision to use sealants on sites containing known enamel lesions is the responsibility of the dentist.”20 As noted by Feigal: “This position in favor of sealing early carious lesions should not be surprising. In retrospect, early caries have been watched and sealed for decades. When we view the low sensitivity and specificity of current fissure diagnostic methods, it is clear we have always misdiagnosed a significant number of fissures…”6
CONCLUSION
Many studies have supported the sealing of incipient lesions. The question remains as to whether clinicians can accurately judge the depth of a lesion. Is it necessary to differentiate whether the lesions are in the enamel versus those that have penetrated into dentin? Or rather should the decision to seal a tooth be based on if the lesion has led to surface cavitation? Clinicians must be able to differentiate the lesions that are progressing from those that are not because evidence supports the use of sealants regardless of the depth of the lesion, with the caveat that the tooth be monitored periodically to ensure the surface integrity is maintained. Prior to the placement of a dental sealant, the clinician must be able to not only detect evidence of dental caries but also diagnose the presence (activity) and risk of disease.
The placement of dental sealants is an effective means of preventing the initiation of occlusal caries and the evidence and opinions of many in the field agree that sealing incipient noncavitated occlusal caries is an acceptable management modality to arrest disease progression. For certain underprivileged population groups, this may be the only treatment modality available through public health programs.
REFERENCES
- Ahovuo-Saloranta A, Hiiri A, Norblad A, Worthington H, Makela M. Pit and fissure sealants for preventing dental decay in the permanent teeth of children and adolescents. Cochrane Database Syst Rev . 2004;3:CD001830.
- Bader J, Shugars D, Bonito AJ. A systematic review of selected caries prevention and management methods. Community Dent Oral Epidemiol . 2001;29:399-411.
- Mejàre I, Lingström P, Petersson L, et al. Caries-preventive effects of fissure sealants: a systematic review. Acta Odontol Scand . 2003;61:321-330.
- Primosch RE, Barr ES. Sealant use and placement techniques among pediatric dentists. J Am Dent Assoc . 2001;132:1442-1451.
- Adair SM. The role of sealants in caries prevention programs. J Calif Dent Assoc . 2003;31:221-227.
- Feigal RJ. The use of pit and fissure sealants. Pediatr Dent . 2002;24:415-422.
- Simonsen RJ. Pit and fissure sealants: review of the literature. Pediatr Dent . 2002;24:393-414.
- Angmar-Mansson BE, al-Khateeb S, Tranaeus S. Caries diagnosis. J Dent Educ . 1998;62:771-779.
- Clark DC, Berkowitz J. The relationship between the number of sound, decayed, and filled permanent tooth surfaces and the number of sealed surfaces in children and adolescents. J Public Health Dent . 1997;57:171-175.
- Dodds MW. Dilemmas in caries diagnosis—applications to current practice and need for research. J Dent Educ . 1993;57:433-438.
- Hassall D, Mellor A. The sealant restoration; indication, success and clinical technique. B Dent J . 2001;191:358-362.
- Bader JD, Shugars DA. Need for change in standards of caries diagnosis—epidemiology and health services research perspective. J Dent Educ . 1993;57:415-421.
- Originating Committee. Clinical guideline on pediatric restorative dentistry. Pediatric Dentistry Reference Manual 2004-2005 . 2005;(suppl):106-114.
- Handelman SL, Buonocore MG, Haseck DJ. A preliminary report on the effect of fissure sealants on bacteria in dental caries. J Prosthet Dent . 1972;27:390-392.
- Handleman SL, Washburn F, Wopperer P. Two-year report on sealant effect on bacteria in dental caries. J Am Dent Assoc . 1976;93:967-970.
- Going RE, Loesche WJ, Grainger DA, Syed SA. The viability of microorganisms in carious lesions five years after covering with a fissure sealant. J Am Dent Assoc . 1978;97:455-462.
- Heller KE, Reed SG, Bruner FW, Eklund SA, Burt BA. Longitudinal evaluation of sealing molars with and without incipient dental caries in a public health program. J Public Health Dent . 1995;55:148-1453.
- Florio FM, Pereira AC, Meneghim Mde C, Ramacciato JC. Evaluation of non-invasive treatment applied to occlusal surfaces. ASDC J Dent Child . 2001;68:326-331.
- Mertz-Fairhurst EJ, Curtis JW Jr, Ergle JW, Rueggeberg FA, Adair SM. Ultraconservative and cariostatic sealed restorative results at year 10. J Am Dent Assoc . 1998;129:55-66.
- American Dental Association. Treating caries as an infectious disease. J Am Dent Assoc . 1995;126:2-8, 15.
From Dimensions of Dental Hygiene. July 2006;4(7): 28, 30-31.

