
More Efficacy, Less Pain
Stanley F. Malamed, DDS, talks to Dimensions about the latest developments in the delivery of local anesthetics.
Q. What were some of the more interesting early local anesthetics used, and how effective were they?
A. Cocaine (1885) and procaine (1904) were the earliest local anesthetics (LAs) used. Both are classified as ester-type LAs. The first injection of a local anesthetic was done in 1885 by the physician surgeon William Halsted, using a cocaine and epinephrine combination. It was hailed as a miracle drug permitting surgeons to perform painless surgery on a conscious patient for the first time. As time passed it became obvious that cocaine possessed other properties, such as addiction and cardiovascular stimulation, that were less than optimal. Indeed, Dr. William Halsted himself became addicted to cocaine, eventually having to leave the practice of medicine to undergo treatment for his addiction.
Procaine was synthesized in Germany by Alfred Einhorn and introduced under the proprietary name Novocain in 1905; it quickly became the most used local anesthetic in the world. The name Novocain, though proprietary, has become like Jello, Xerox, and Ping-Pong; it is commonly used to describe any dental anesthetic injection. Procaine with epinephrine remained the gold standard in local anesthesia until the introduction of the first amide anesthetic, lidocaine, in the late 1940s.
Compared to amide anesthetics, the esters were as a group less effective, slower in onset, and had a propensity toward allergenicity. Following the introduction of amide anesthetics, the use of esters in dentistry has ceased.
PAIN PERCEPTION
Q. “The shot” is often viewed as a source of pain and anxiety by patients. How much does anxiety contribute to the perception of pain?
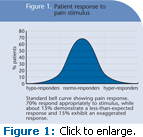
A. Anxiety has a lot to do with the perception of pain. When a nerve is stimulated, as with a curet, a nerve impulse is propagated and carried to the brain where it is interpreted by the patient. Give the same exact stimulation to 100 persons and you may get 100 different responses. Based on a bell-shaped curve, approximately 70% will respond appropriately to the stimulus (normo-responders) while about 15% will demonstrate a somewhat less than expected response (hypo-responders). The remaining 15%—the hyperresponders—will exhibit an exaggerated response to the same stimulus. Hyperresponders are fearful patients who typically jump when a stream of air is directed at them or who feel pain when their lips are gently touched by the dentist or dental hygienist.
Fear and anxiety lower the pain reaction threshold, the point at which a person will respond to a given stimulus as being painful. The problem is not the stimulus. It is the way the patient’s brain is interpreting it. The answer is simple—sedation, ie, distraction. Whether drugs are used to accomplish this (oral, inhalation [N2O-O2], intravenous, intranasal) or a headset with music or a movie on video, the goal is always the same. Take the patient’s mind away from what is happening in his or her mouth.
Q. What are some of the newer local anesthesia techniques used in dentistry that produce less anxiety and/or less pain?
 A. Computer-controlled local anesthetic delivery (C-CLAD) was introduced in 1998 and it allows the dentist or hygienist to provide painless delivery of LA to a patient in any area of the oral cavity, including the palate. The latest iteration of C-CLAD is the recently introduced STA (single tooth anesthesia).
A. Computer-controlled local anesthetic delivery (C-CLAD) was introduced in 1998 and it allows the dentist or hygienist to provide painless delivery of LA to a patient in any area of the oral cavity, including the palate. The latest iteration of C-CLAD is the recently introduced STA (single tooth anesthesia).
The periodontal ligament (PDL) injection (intraligamentary injection) permits the painless treatment of a single tooth in the mandible. (This technique is not used much in the maxilla because infiltration works quite well.) When administered with a CCLAD device, the PDL injection has a very high rate of success and is extremely comfortable for the patient.
Infiltration of LAs is rarely successful in the mandible of adults because the cortical plate of bone is too thick to permit diffusion into the nerve. Research shows that articaine HCl infiltrated into the buccal fold adjacent to the mandibular first molar has a high success rate providing pulpal anesthesia to the molars and premolars.1,2
Q. Does the delivery of an anesthetic agent through a C-CLAD help with adverse reactions?
A. Definitely yes. C-CLADs are designed to help make injections painless (or as close to painless as possible) while still delivering the local anesthetic drug in a safe (slow) manner regardless of the site of deposition. These devices are also used in medicine to help with the administration of local anesthetics in areas that are extremely painful like the heel of the foot and the skin in and around the eyes. Because these devices can aspirate blood and because they deposit the drug slowly, the risk of inadvertent intravascular injection is minimal.
C-CLADs appear less frightening to patients because they can’t see a traditional metal local anesthetic syringe. C-CLADs do require a needle, so there still remains the possibility of psychogenic reactions (eg, syncope, hyperventilation) should the patient see the needle.
Q. Are there new agents that are more effective than what has been used in the recent past?
A. I believe that articaine is more effective in the mandibular molars and premolars, whether administered by block (IANB, Gow-Gates) or mandibular infiltration.3-5 Articaine is a more lipid-soluble molecule than other LAs, thus explaining its higher success rate by mandibular infiltration.
LIMITING THE NUMBING EFFECT
Q A new agent that reverses the numbing effect of local anesthesia is now available. How does this product work?
A. Phentolamine mesylate* is a vasodilator that is injected into the site where the LA was administered at the start of dental treatment. Phentolamine mesylate dilates blood vessels in the area, thus increasing blood flow, which accelerates the diffusion of the LA out of the nerve and into the cardiovascular system where it is removed from the site. The duration of residual soft tissue anesthesia (eg, lip, tongue) is decreased by approximately 50%, so instead of remaining numb for another 4 hours after leaving the dental office, the patient senses the return of normal function in about 2 hours. Clinical trials demonstrated that 41% of patients had 100% return of sensation to the lower lip in 60 minutes after receiving the phentolamine mesylate injection. In the maxilla, 59% had full recovery of the lip in 60 minutes (compared with 7% and 12% for the controls).6,7
REFERENCES
- Malamed S. What’s new in local anaesthesia? SAAD Dig. 2009;25:4-14.
- Moore PA, Boynes SG, Hersh EV, et al. The anesthetic efficacy of 4 percent articaine 1:200,000 epinephrine: two controlled clinical trials. J Am Dent Assoc. 2006;137:1572-1581.
- Kanaa MD, Whitworth JM, Corbett IP, Meechan JG. Articaine buccal infiltration enhances the effectiveness of lidocaine inferior alveolar nerve block. Int Endod J. 2009;42:238-246.
- Robertson D, Nusstein J, Reader A, Beck M, McCartney M. The anesthetic efficacy of articaine in buccal infiltration of mandibular posterior teeth. J Am Dent Assoc. 2007;138:1104-1112.
- Mikesell P, Nusstein J, Reader A, Beck M, Weaver J. A comparison of articaine and lidocaine for inferior alveolar nerve blocks. J Endod. 2005; 31: 265-270.
- Laviola M, McGavin SK, Freer GA, et al. Randomized study of phentolamine mesylate for reversal of local anesthesia. J Dent Res. 2008; 87: 635-639.
- Hersh EV, Moore PA, Papas AS, et al. Reversal of soft-tissue local anesthesia with phentolamine mesylate in adolescents and adults. J Am Dent Assoc. 2008;139:1080-1093.
From Dimensions of Dental Hygiene. July 2009; 7(7): 22, 24.

