Essential Tools for Increasing Health Literacy
How to improve patients’ understanding of health care communication.
This course was published in the February 2012 issue and expires February 2015. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Define health literacy.
- Discuss why health literary is important.
- Identify strategies for improving written and verbal communication.
Dental hygienists are fascinated by the oral cavity and undergo extensive education on the science of dental health. To us, reading a brochure about periodontal diseases may seem like light reading. But how do our patients feel? Reviewing and understanding provided materials on oral health may equate to reading Greek for our patients. Dental hygienists may be hampered in their efforts to improve patients’ oral health if their degree of health literacy is not ascertained and addressed.
Health literacy is defined as the degree to which individuals have the capacity to obtain, process, and understand basic health information and services needed to make appropriate health decisions.1,2 Health literacy is based on a person’s ability to read, listen, analyze, and make decisions in health care situations.4 The 2010 United States Surgeon General’s Report identified health literacy as an important component of health communication, medical product safety, and oral health.3 Many factors impact health literacy: communication skills of both the patient and the health care professional, current knowledge level about health/medical topics, culture, demands of the health care system, and the context of the situation.
The impact of health literacy is farreaching—affecting people’s ability to navigate the health care system; engage in self-care practices and disease prevention; fill out medical and insurance forms; and understand basic math concepts such as how to calculate drug dosages, interpret test results, or read food labels.
Table 1. Levels of Literacy9
Below Basic: Only the most simple and concrete literacy skills are obtained
Basic: Skills necessary to perform everyday simple literacy activities
Intermediate: The ability to perform moderately challenging activities
Proficient: Skills necessary to perform more complex and challenging activities
Since the 1990s, the American Medical Association has been promoting the link between low health literacy and poor health outcomes, noting that health literary is a greater predictor of health than age, income, employment status, education level, or race.4 In some instances, health care providers may assume their patients understand their own health status, and what is being explained to them. Research, however, has shown that the number of Americans with limited health literacy is near 90 million.3-5 Thus, health care providers need to improve their ability to provide medical information in order to adequately address the health literacy problem.5
Why is Health Literacy Important?
It has been reported that nine out of 10 adults (16 years and older) have difficulty understanding and using health information.7 Low health literacy has been linked to poor health outcomes, increased rates of hospitalization, more medication errors, less compliance with treatment, and limited use of preventive services.8-10 In the technology age, patients have access to a multitude of sources for health care information, including the Internet, television, magazines, and materials provided by health care providers. Whether patients are able to accurately assess and process the information is an important question.
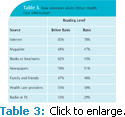
 Patients receive most information about prevention efforts and maintaining or improving oral health in the written format (Table 3).9 Whether in magazines, patient brochures, prescription bottles, food labels, patient instructions, or on the Internet, a large segment of the adult population is unable to adequately obtain, process, or understand basic health information.7 NAAL found that adults with a below basic literacy level were least likely to access health information from print and nonprint sources.7 Individuals with basic or below basic literacy levels may not have the knowledge or ability to follow instructions, make decisions regarding their health, adopt health promoting behaviors, fill out medical and insurance forms, or provide adequately informed consent.
Patients receive most information about prevention efforts and maintaining or improving oral health in the written format (Table 3).9 Whether in magazines, patient brochures, prescription bottles, food labels, patient instructions, or on the Internet, a large segment of the adult population is unable to adequately obtain, process, or understand basic health information.7 NAAL found that adults with a below basic literacy level were least likely to access health information from print and nonprint sources.7 Individuals with basic or below basic literacy levels may not have the knowledge or ability to follow instructions, make decisions regarding their health, adopt health promoting behaviors, fill out medical and insurance forms, or provide adequately informed consent.
High Risk Groups
There is a wide range of demographics affected by low health literacy. Older adults (65 years and older) were found to have the lowest health literacy scores in comparison to other groups–23% fell in the below basic literacy range.7,8 One-third of American adults have difficulty reading and following through on health-related information.9 Even people at the intermediate or proficient literacy levels can still have difficulty comprehending medical jargon and technical aspects of health information. Comprehension levels are about two or more grade levels below reading or education level, and when a person is under stress, the level drops even lower.10 Research has shown that populations most often impacted include: individuals with limited education, older adults, those with lower socioeconomic status, individuals with limited English proficiency, and racial and ethnic minorities.2,10
Improving Understanding of Health Information
With almost half of the adult population in the US reading at the 5th grade to 8th grade level, health information in written form may be beyond the comprehension of many patients. There are some basic tools that health care providers can apply to improve the readability and comprehension of written materials and the comprehension verbal communication (Table 4).
A verbal tool for assessing whether the patient has understood and retained the communicated information is called the “teach-back” method. This literary technique confirms whether patients understand what you have said by having them repeat the information in their own words back to you. It also provides an assessment of comprehension and clarification of the information presented.11 For example, a dental hygienist might ask a patient: “Tell me what you will share with your wife today regarding the changes in your self-care regimen,” or “What will you tell your brother about how to care for your surgical site?”
The teachback technique allows the health care provider to determine if there are any gaps or incorrect information retained by the patient, and provides the patient with an opportunity to correct and reinforce the comprehension of the material. Additional tips to use when speaking to patients include: maintain eye contact; use nonmedical language; be specific; limit key points to no more than four; use pictures, drawings, or models to help convey messages; repeat and/or summarize both in the beginning at the end; use a positive tone; involve the patient; and cover the material slowly and thoroughly.12,13
Table 5. Formulas Used to Test the Readability of Text
Flesch-Kincaid Readability Test: www.readabilityformulas.com/flesch-grade-level-readability-formula.php
Fry Readability Graph: www.readabilityformulas.com/fry-graph-readability-formula.php
Gunning Fog Index: www.readabilityformulas.com/gunning-fog-readability-formula.php
Simple Measure of Gobbledygook Readability Formula: www.readabilityformulas.com/smog-readability-formula.php
Testing Readability
There are many formulas available to test the readability of a document, including the Flesch-Kincaid Readability Test, the Fry Readability Graph, the Gunning Fog Index, and the Simple Measure of Gobbledygook Readability Formula (Table 5). Software programs are also available that provide readability statistics, but plain language experts do not consider these tests reliable.
They determine the readability of text based on the average number of syllables per word and average words per sentence, and do not take into account the design of the document. Comprehension levels are also not accounted for when using any of the various tests, only the grade level that the document is written in. Readability formulas alone do not guarantee that a document is understandable, and they should be used in conjunction with other methods to improve the readability of text.
There are some basic techniques to improve the readability of documents, including: reducing the number of words per sentence, using words with single or double syllables instead of multiple syllables, avoiding the passive voice, and using “everyday” language.14
Getting Involved
Health literacy is an important concern—especially to those involved with health screenings, promotion, intervention, and management. Dental hygienists are in a unique position to screen and educate adults who may be vulnerable to low literacy. Therefore, they must communicate oral health information in a method that will be understood, regardless of a patient’s literacy level. Developing strategies to bridge the gap in oral health care communication will help patients better manage their oral conditions—ultimately leading to improved oral and systemic health.
REFERENCES
- US Department of Health and Human Services. Healthy People 2010. 2nd ed. Washington, DC: US Government Printing Office; 2000.
- Institute of Medicine. Health Literacy: a Prescription to End Confusion. Washington, DC: National Academies Press; 2004.
- US Department of Health and Human Service. Health Communication and Health Information Technology. Available at: www.healthypeople.gov/2020/topicsobjectives2020/objectiveslist.aspx?topicId=18. Accessed January 25, 2012.
- National Network of Libraries of Medicine. Health Literacy. Available at: www.nnlm.gov/outreach/consumer/hlthlit.html. Accessed January 25, 2012.
- American Medical Association. Health Literacy. Available at: www.ama-assn.org/ama/pub/about-ama/ama-foundation/our-programs/public-health/health-literacy-program.page. Accessed January 25, 2012.
- Cutilli CC, Bennett IM. Understanding the health literacy of America: results of the National Assessment of Adult Literacy. Orthop Nurs. 2009;28:27-34.
- Kutner M, Grenberg E, Jin Y, Paulsen C. The Health Literacy of America’s Adults: Results from the 2003 National Assessment of Adult Literacy. Available at: www.nces.ed.gov/pubs2006/2006483.pdf. Accessed January 25, 2012.
- Marcus EN. The silent epidemic–the health effects of illiteracy. N Engl J Med. 2006;355: 339-341.
- National Center for Education Statistics. National Assessment of Adult Literacy. Available at: www.nces.ed.gov/naal/index.asp. Accessed January 25, 2012.
- Centers for Disease Control and Prevention. Simply Put–A Guide For Creating Easy-To-Understand Materials. Available at: www.cdc.gov/healthliteracy/pdf/Simply_Put.pdf. Accessed January 27, 2012.
- Schillinger D, Piette J, Grumbach K, et al. Closing the loop: physician communication with diabetic patients who have low health literacy. Arch Intern Med. 2003;163:83-90.
- Rudd RE, Anderson JE, Oppenheimer S, Nath C. Health literacy: an update of public health and medical literature. In: Comings JP, Garner B, Smith C, eds. Review of Adult Learning and Literacy. Mahwah, NJ: Lawrence Erlbaum Associates Inc; 2007:175-204.
- Centers for Disease Control and Prevention. Health Literacy. Available at: www.cdc.gov/healthliteracy. Accessed January 25, 2012.
- Barzel R. A Way with Words: Guidelines for Writing Oral Health Materials for Audiences with Limited Literacy 2008. National Maternal and Child Oral Health Resource Center. Available at: www.cda.org/library/pdfs/awaywithwords.pdf. Accessed January 25, 2012.
From Dimensions of Dental Hygiene. February 2012; 10(2): 64-67.
5