
Ensure the Safe Use of Digital Radiography
Digital imaging offers many benefits, but it also poses infection control challenges that must be addressed.
The more than century-old method of using conventional film to obtain radiographic images is being replaced by digital imaging in most clinical settings.1,2 Introduced to dentistry in 1987, digital imaging offers many advantages compared to traditional film. It reduces patient exposure to radiation by 50% to 90%.3–6 Digital radiography also enhances image quality due to its superior gray-scale resolution and it offers immediate image acquisition for rapid interpretation and evaluation.3–7 In addition, digital imaging imparts environmental benefits as it eliminates the need for film and processing chemicals, particularly the foil backings used in film and the silver from X-ray fixers.3–7
While providing these advantages, digital imaging has also created new infection control challenges. Unlike film packets, which must be disposed of completely, intraoral image receptors in digital radiography are reusable. Therefore, these image receptors are a potential source of contamination, even though they are contained in a plastic barrier.8–10
This article reviews the current infection control protocols for digital intraoral radiography use established by the United States Centers for Disease Control and Prevention (CDC).
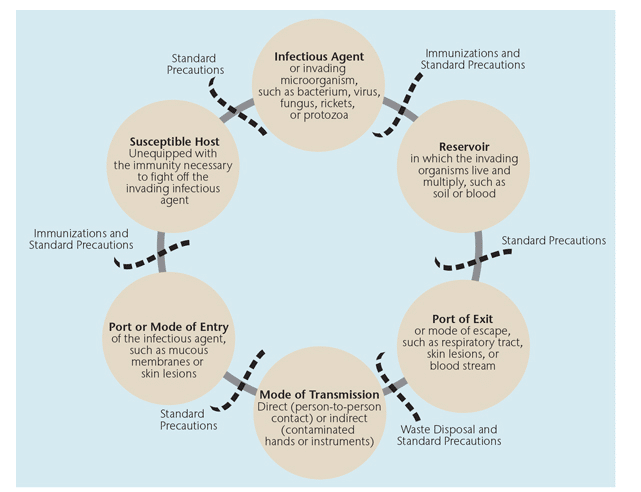
CHAIN OF DISEASE TRANSMISSION
The CDC released Guidelines for Infection Control in Dental Health-Care Settings—2003 to reduce or eliminate the risk of patient and clinician exposure to pathogens during the delivery of dental care.11 These guidelines should be observed in conjunction with the practices and procedures required for worker protection by the Occupational Safety and Health Administration (OSHA).12 Effective infection control in health care settings involves complying with recommendations to reduce the risk of transmission. They rely on the use of universal precautions in the treatment of all patients—regardless of their infectious disease status—to disrupt the chain of disease transmission. Standard precautions seek to reduce the risk of transmitting pathogens that can be spread by blood or other body fluids, excretions, or secretions.11–14

To better understand asepsis in the dental setting, a review of disease transmission principles is necessary. Disease transmission results from the interaction of an agent, host, and environment in a process involving six related links. The six links in this chain of disease transmission include:
- Infectious agent or invading microorganism, such as bacterium, virus, fungus, rickets, or protozoa
- Reservoir in which the invading organisms live and multiply, such as soil or blood
- Port of exit or mode of escape from the reservoir, such as respiratory tract, skin lesions, or blood stream
- Mode of transmission—direct, through person-to-person contact; or indirect, through an intermediate vehicle, such as contaminated hands or instruments
- Port or mode of entry of the infectious agent into the new host, such as mucous membranes or skin lesions
- Susceptible host unequipped with the immunity necessary to fight off the invading infectious agent3–7,14,15
Effective infection control strategies prevent disease transmission by interrupting one or more links in this chain. Figure 1 illustrates the chain of disease transmission and the interventions necessary to prevent transmission.3–7,14,15
INFECTION CONTROL PROTOCOL
Infection control procedures for digital radiography assume that all body fluids (except sweat) have the potential to be infectious, and they focus on reducing risks related to three of the six links of disease transmission—port of exit, transmission, and port of entry. Specifically, protective barriers, waste disposal, and disinfection help contain secretions or droplets from the oral cavity, inhibit contamination of devices, and prevent contact between contaminated devices and patients/clinicians.
Infection control procedures for digital radiography can be divided into three categories:
- Before radiographic exposure
- During radiographic exposure
- After radiographic exposure
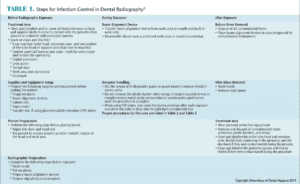
Table 1 lists the steps to achieve infection control in dental radiography for each of these categories.
Infection control protocols for digital intraoral radiography require additional considerations due to the use of reusable supplies. The CDC guidelines discuss the importance of using single-use disposable barriers to prevent contamination of nonremovable parts or supplies that cannot be appropriately cleaned and disinfected. Personal protective equipment should be worn when taking images and when handling contaminated receptors to prevent cross-contamination and limit the exposure of dental health care personnel.11,12,14,16 In film-based imaging, cross-contamination is prevented by complete disposal of the packaging. In digital intraoral radiography, however, the risk of cross-contamination is increased because the intraoral image receptors (sensors) are reusable. Studies have shown that receptors contained in a plastic barrier remain a potential source of contamination due to defects in the integrity of the plastic barrier and failure to remove the sensors from the plastic barrier effectively.8–10 In one study, barrier perforations occurred in 44% to 51% of the plastic sheaths.8 According to Hokett et al,8 these tears may have occurred when placing or removing the sensor from the plastic sheath. Consequently, the handling of these receptors requires additional precautions.
There are three different types of image receptors used in digital radiography:
- Charged-coupled device (CCD) sensor
- Complementary metal oxide semiconductor (CMOS)/active pixel sensor (APS)
- Photostimulable phosphor (PSP) plate 3–7
CCD sensors and CMOS/APS are wired and PSP is wireless. As none of these receptors can be heat sterilized, they must be covered with a Food Drug and Administration-approved single-use disposable plastic barrier in order to avoid cross-contamination.3–7 These plastic barriers are carefully removed to maintain asepsis and are discarded between patients.
Sensors, though protected by a plastic barrier while in the oral cavity, must still be handled carefully. Contamination of the intraoral receptors may occur during sensor preparation (cleaning, disinfecting, and packaging) and during processing. The most likely source of contamination is contact between the intraoral sensors with oral fluids during the removal process (eg, contact of the sensor with contaminated gloves).8–10 Table 2 and Table 3 include the necessary steps for handling digital intraoral sensors during processing, including manufacturer recommendations.
SUMMARY
During exposure of radiographs, the potential to cross-contaminate equipment and environmental surfaces with blood and saliva is high if aseptic techniques are not practiced. For this reason, regardless of the type of radiographic imaging used, clinicians should review and practice the guidelines and concepts of infection control. Radiographic equipment, such as tube heads, control panels, and receptors, should be protected with plastic barriers that are changed after each patient. Because digital intraoral sensors are reused, they also require complete coverage with disposable, single-use plastic barriers in order to prevent cross-contamination—with special attention taken during the processing stage. Receptors must be carefully removed from the disposable plastic barrier to avoid cross-contamination, and they must be cleaned and disinfected after use.8–10,14 To help practitioners reduce the risk of infection and cross-contamination in dental radiography, companies are constantly designing new devices (eg, X-ray sleeves, barrier envelopes, cleaning and disinfecting wipes, and alcohol-soaked wipes). Clinicians should continue to seek out the most current research and products to provide the most aseptic techniques in dental radiography.
REFERENCES
- Van der Stelt PF. Filmless imaging: the uses of digital radiography in dental practice. J Am Dent Assoc. 2005;136:1379–1387.
- State of New York Bill A8073-2011. Requires Dentists and Dental Hygienists to use Digital Radiography on Patients under the Age of 18. Available at: open.nysenate.gov/legislation/bill/A8073-2011. Accessed February 17, 2015.
- Iannucci JM, Howerton LJ. Dental Radiography: Principles and Techniques. 4th ed. St. Louis: Saunders Elsevier; 2012.
- Frommer HH, Stabulas-Savage JJ. Radiology for the Dental Professional. St. Louis: Mosby; 2011. D
- Thomson EM, Johnson ON. Essentials of Dental Radiography for Dental Assistants and Hygienists. 8th ed. Upper Saddle River, NJ: Pearson Education; 2012.
- Darby ML, Walsh P. Dental Hygiene: Theory & Practice. 4th ed. St Louis: Saunders Elsevier; 2015.
- Wilkins EM. Clinical Practice of the Dental Hygienist. 11th ed. Philadelphia: Lippincott Williams & Wilkins; 2013.
- Hokett SD, Honey JR, Ruiz F, Baisden MK, Hoen MM. Assessing the effectiveness of direct digital radiography barrier sheaths and finger cots. J Am Dent Assoc. 2000;131:463–437.
- MacDonald DS, Waterfield JD. Infection control in digital intraoral radio – graphy: evaluation of microbiological contamination of photostimulable phosphor plates in barrier envelopes. J Can Dent Assoc. 2011;77:b93.
- Kuperstein AS. Defective plastic infection-control barriers and faulty technique may cause PSP plate contamination used in digital intraoral radiography. J Evid Based Dent Pract. 2012;12:46–47.
- Kohn WG, Collins AS, Cleveland JL, et al. Guidelines for infection control in dental health-care settings—2003. MMWR Recomm Rep. 2003;52(RR-17):1–61.
- Occupational Safety & Health Administration. Infectious Diseases. Available at: osha.gov/SLTC/healthcarefacilities/infectious_diseases.html. Accessed February 17, 2015.
- World Health Organization. Infection Control. Available at: who.int/ topics/infection_control/en. Accessed February 17, 2015.
- Centers for Disease Control and Prevention. Preventing Healthcare- Associated Infections. Available at: cdc.gov/HAI/prevent/prevention.html. Accessed February 17, 2015.
- Centers for Disease Control and Prevention. Chain of Infection. Available at: cdc.gov/ophss/csels/dsepd/ss1978/lesson1/section10.html. Accessed February 17, 2015.
- American Dental Association Council on Scientific Affairs. The use of dental radiographs: update and recommendations. J Am Dent Assoc. 2006;137:1304–1312.
From Dimensions of Dental Hygiene. March 2015;13(1):26,28,30,32–33

