
On the Cutting Edge
Consistent and precise instrument sharpening is crucial to effective instrumentation and your own musculoskeletal health.
Are you satisfied with your sharpening results? Routine and accurate sharpening of manual instruments is one of the most important aspects of effective instrumentation. Sharpening can also help prevent musculoskeletal problems1 associated with the use of too much force or heavy handedness.
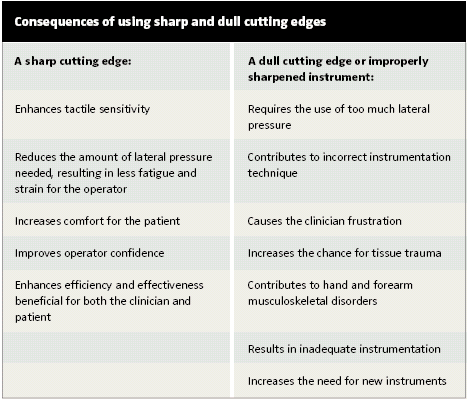
Efficiency and effectiveness of quality dental hygiene care are paramount for both the patient and clinician, especially when providing nonsurgical periodontal therapy (NSPT). Multiple appointments are required at the onset of NSPT and all efforts to streamline deposit removal are beneficial for the patient’s personal time, the operator’s appointed time, and the office’s scheduling. See the web version of this article at www.dimensionsofdentalhygiene.com for a table that reviews the advantages of using a sharp cutting edge.
Set goals for instrument sharpening work strategies to improve success and reduce burnout or stress. Plan how you will accomplish the following on a daily or periodic basis:
- Routine sharpening prior to and during use.
- Routine evaluation for instruments that are useless or hazardous to use.
- Daily self-assessment of your sharpening technique.
- Periodic peer discussions about design, sharpening, ordering, and incorporation of new instruments into practice.
- Periodic peer assessment of your technique.
EVALUATING SHARPNESS
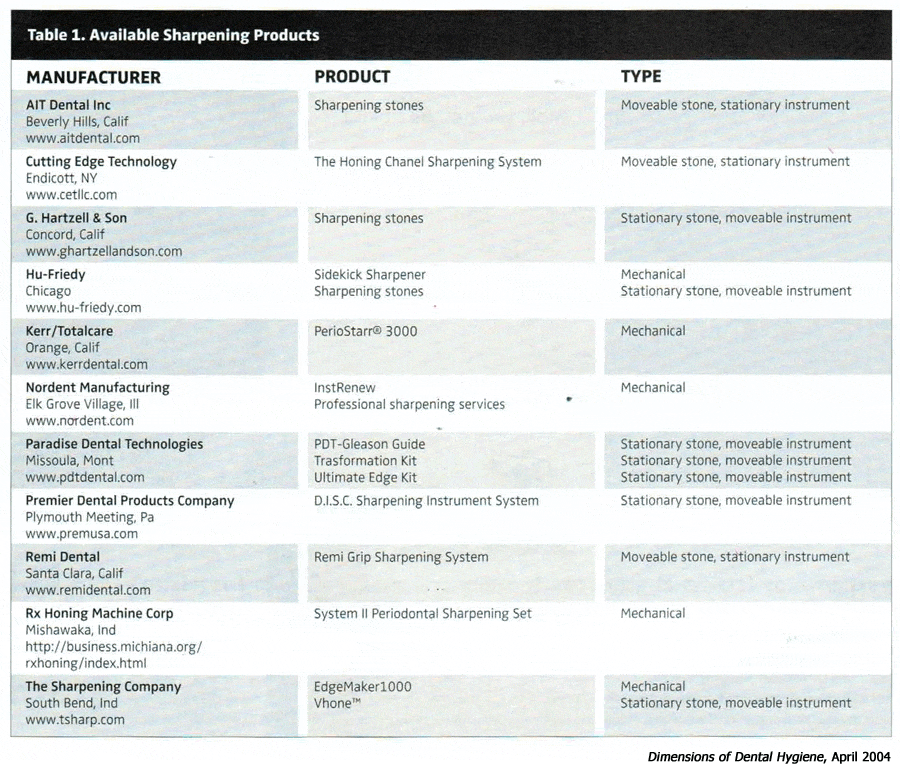
The purpose of sharpening is to produce an acute sharp cutting edge while maintaining original contour. Cutting edge quality is defined by four factors: the angle between the face and lateral surface, smoothness of the blade, relative sharpness or dullness, and presence or absence of metallic projections.2 Ideally, the internal angle—defined by the face and lateral surfaces of a curet—is 70°to 80° because it creates an optimal cutting edge for calculus removal. Smoothness, visualized by magnification, refers to the regularity of the cutting edge controlled by the fineness of the abrasive,3 such as the Arkansas stone. A finer grain stone abrades or reduces the blade slowly and produces a fine cutting edge.4 The smooth surface of blades created by a fine grit stone is, in turn, related to the smoothness of the root.5 Manufacturers’ catalogs identify particle size or grain of different stones. Table 1 lists some of the sharpening products available.
The relative sharpness in clinical practice is evaluated by visual and tactile tests. The difference between a dull cutting edge and a sharp one is determined by the visual appearance, performance during instrumentation, and the internal angle of the instrument. The presence of metal projections relates to wire edges on new or sharpened instruments. New instruments have numerous wire edges and need to be sharpened prior to use.2,6-9 Because wire edges are not clinically visible, proper sharpening technique must be used to prevent their occurrence by finishing each segment of the cutting blade with a downward stroke.
THE SHARPENING PROCESS
The sharpening sequence for the moveable stone, stationary instrument method is reviewed in Table 2. This process form is useful for self-assessment and peer evaluation. This step-by-step approach can be used by clinicians for a periodic assessment or checklist for technique and for peer evaluation in the office or during a continuing education course.
The steps in the sharpening process build upon one another and if the first step is incorrect, then all steps that follow are also incorrect. For example, if the face of the curet is not situated parallel to the floor, then placing the stone to the lateral surface at an apparent 90° angle and opening the stone 10° to 20° to achieve a 100° to 110° stone-to-face angle is inaccurate. The result is that the ideal internal angle of the curet is altered as previously described. Use of a protractor placed behind the face of the blade helps the clinician estimate the stone- to-face angle.
In the moveable stone, stationary instrument method, the stone is moved by the clinician with short up and down strokes on a counter or mobile cabinet. In the stationary stone, moveable instrument technique, the flat stone is stabilized on a surface with one of the clinician’s hands and the instrument is moved across the stone with push and pull strokes with the clinician’s opposite hand maintaining the proper instrument-to-stone angulation.
Manufacturers have developed guides to assess instrument and stone placement. Guides might benefit clinicians striving to perfect their sharpening technique, although an understanding of the original contour of the instrument and the goals and tests for sharpening are still necessary. Guides might also standardize the sharpening process when more than one person in the office is sharpening instruments that are shared with other professionals.10
Likewise, many mechanical sharpening devices are available from manufacturers. However, a thorough understanding of contour and assessment of properly sharpened instruments are still needed.
TESTING METHODS
Three tests are used to evaluate sharpness: 1) visual examination, 2) biting into an autoclavable test stick, and 3) sound created by a working stroke. Testing occurs prior to seating the patient, during therapy, or at maintenance intervals. Maintenance sharpening encourages maximum concentration, provides an unlimited time period, and is useful if certain team members are responsible for sharpening instruments for others. Maintenance sharpening is performed for all instruments at a routine time, not in the presence of a patient. For example, clinicians might schedule a time period each week to examine and sharpen instruments in preparation for the next week’s therapy.

Visual examination is based on the principle that the rounded edge or facet (dull blade), when placed under light, will appear white and shiny. This white line is observable with the naked eye or under magnification at the junction of the face and lateral surface where an acute cutting edge should be. The key to accurate observation is to rotate the instrument from face to lateral surface until the cutting edge is facing the central beam of the light. Visual examination also includes evaluation of the quality of the edge.
Placing a cutting edge against a test stick is effective when performed correctly. Clinicians must test the blade against the stick by employing the same angle (approximately 70° to 80°) and the lateral pressure used when instrumenting. A fulcrum is placed on the test stick and the blade is engaged at the heel, middle, and terminal end. If the instrument “bites” into the stick on the first attempt, it is sharp. If, however, the instrument can be dragged or pulled along the stick then additional sharpening is indicated. Any instrument can appear sharp using this technique if improper angles and excessive pressure are applied.
The sound test is extremely practical to use during therapy. The practitioner listens for the sound of the instrument during calculus removal and, if absent, the instrument is dull. The strokes made by a sharp instrument during channeling (powerful, short, overlapping working strokes) instrumentation produce an audible metallic sound. When this sound is no longer present, the clinician should stop and sharpen. Evaluation of instrumentation technique is frequent to ensure the proper blade to tooth angle is being used to create the sound.
MAINTENANCE
Continual sharpening throughout the debridement process is the key to maintaining sharp curets that do not need recontouring. When a clinician makes the choice to not sharpen during instrumentation, the detrimental effects previously mentioned occur. In addition, when sharpening is finally initiated the process is difficult because the blade is extremely dull. Also, excess metal is removed decreasing the longevity and increasing the financial burden of ordering new instruments.
How many strokes or how long can one instrument be used before sharpening is needed? The answer to this question depends on the initial sharpness of the blade, size of the deposit, tenacity of the deposit, and force exerted by the clinician. After 45 root planing strokes a significant bevel is usually formed.2,9,11 Although root planing performed to create a hard, glassy, smooth surface is no longer advocated, estimation of stroke numbers is useful in clinical practice.
 The need for recontouring will diminish as practitioners gain experience and proficiency with sharpening technique. Recontouring is needed to remove a significant bevel on the cutting edge and to restore the original contour of the instrument. A bevel is eliminated by removing enough metal from the lateral surface to reform the sharp cutting edge. The stone is placed at an angulation of about 110° to the face of the curet and routine sharpening is employed until an acute cutting edge is again created. Removal of a significant bevel takes longer than routine sharpening.
The need for recontouring will diminish as practitioners gain experience and proficiency with sharpening technique. Recontouring is needed to remove a significant bevel on the cutting edge and to restore the original contour of the instrument. A bevel is eliminated by removing enough metal from the lateral surface to reform the sharp cutting edge. The stone is placed at an angulation of about 110° to the face of the curet and routine sharpening is employed until an acute cutting edge is again created. Removal of a significant bevel takes longer than routine sharpening.
If the original shape of the curet has been compromised it is probably because the cutting edges were not sharpened in segments or the toe was not rounded. These problems are corrected by using proper sharpening skills to remove metal from the needed areas to restore the original contour. For example, if the middle of the cutting edge of an area-specific curet is flattened then metal must be removed from the toe and heel one-thirds of the blade significantly reducing blade width. If the toe is narrow and pointed, then sharpening is needed to round the toe.
Examination of an improperly contoured instrument requires that the clinician decide if enough metal remains to warrant recontouring or if the instrument should be replaced. Indications for replacement include loss of one half the width of the blade or bending during testing or scaling.12-14 Comparing new and used instruments is helpful in making these decisions. Failure to recognize the need for new instruments endangers the patient, results in considerable risk for the professional, and negatively affects the quality and efficiency of instrumentation.
Ultimately, a sharp instrument improves the quality of periodontal debridement. Factors that are within the clinician’s control are routine sharpening of instruments with each use, use of proper technique, and accurate assessment of sharpness. Quality assessment of this technique is related to quality assurance in your practice.
References
- Michalak-Turcotte C, Atwood-Sanders M. Ergonomic strategies for the dental hygienist PartI.Journal of Practical Hygiene. 2000;9:39-42.
- Tal H, Panno JM, Vaidyanathan TK. SEM evaluation of wear of dental curettes during standardized root planing. J Periodontol. 1985;56:532-536.
- Paquette OE, Levin MP. The sharpening of scaling instruments:I.An examination of principles. J Periodontol.1977;48:163-168.
- Wilkins EM. Instruments and principles for instrumentation. In: Wilkins EM, ed. Clinical Practice of the Dental Hygienist. 8th ed.Philadelphia: Lippincott, Williams and Wilkins; 1999:532.
- Rossi R, Smukler H. A scanning electron microscope study comparing the effectiveness of different types of sharpening stones and curets. J Periodontol. 1995;66:956-961.
- ClarkSM, Ueno H. An examination of periodontal curettes: an SEM study. Gen Dent.1990;38:14-16.
- DeNucci DI, Mader CJ. Scanning electron microscopic evaluation of several resharpening techniques. J Periodontol. 1983;54:618-628.
- Hoffman LA, Gross KB, Cobb CM, Pippin DJ, Tira DE, Overman PR. Assessment of curet sharpness. J Dent Hyg. 1989;63:382-387.
- Huang C, Tseng C. Effect of different sharpening stones on periodontal curettes evaluated by scanning electron microscopy. J Form Med Assoc. 1991;90:782-787.
- Ellingson P. Instrument sharpening. How to solve your sharpening problems. Journal of Practical Hygiene. 1993;Nov/Dec:23-25.
- Oleary TJ, Kafrawy AH.Total cementum removal: a realistic objective. J Periodontol. 1983;54:221-226.
- Keselyak N, Maschak L. Quality assessment in continuing education: an example of an instrument sharpening workshop for dental hygienists. Probe. 1995;29:13-17.
- Wilkins EM. Instruments and principles for instrumentation. In Wilkins EM, ed. Clinical Practice of the Dental Hygienist. 8th ed.Philadelphia: Lippincott, Williams and Wilkins; 1999:542.
- Schwartz M. The prevention and management of the broken curet. CompendContin Educ Dent. 1998;19:418-425.
From Dimensions of Dental Hygiene. April 2004;2(4):16, 18, 20.

