
Avoid Low Back Pain
Musculoskeletal disorders, particularly low back pain, are common among oral health professionals. Here are strategies to keep your back healthy.
Low back pain (LBP) is a common musculoskeletal disorder among oral health professionals and is often associated with overuse and strain of muscles. Appropriate back support, such as a lumbar roll that maintains the low back curve, helps reduces the occurrence of spine-related musculoskeletal injuries. However, other factors such as prolonged sitting, sitting with poor posture, sitting with uneven pressure, and twisting the spine while sitting or standing, may also contribute to this disorder.
LOW BACK PAIN IN ORAL HEALTH CARE PROFESSIONALS
The prevalence of LBP in oral health practitioners is between 53% and 64%1 whereas in the general United States adult population, it is 27%.2 Generally, oral health professionals report higher rates of LBP compared to other occupational groups such as physicians and pharmacists.3
 Leggat et al1 reported that dentists, dental hygienists, and dental assistants had lower incidences of LBP relative to years from graduation. This may be because practitioners further from graduation have learned to adapt their working postures and techniques, or developed coping strategies to deal with LBP pain, thus not reporting problems. However, the authors1 also suggest that the practitioners further from graduation with severe back problems might have stopped working, thus making them unavailable for the investigation.1 Among the general American population, back and spine problems are the second leading cause of disabilities in all age groups.3 Moreover, reported LBP also increases with age and often includes decreased participation in dayto- day occupational activities.4
Leggat et al1 reported that dentists, dental hygienists, and dental assistants had lower incidences of LBP relative to years from graduation. This may be because practitioners further from graduation have learned to adapt their working postures and techniques, or developed coping strategies to deal with LBP pain, thus not reporting problems. However, the authors1 also suggest that the practitioners further from graduation with severe back problems might have stopped working, thus making them unavailable for the investigation.1 Among the general American population, back and spine problems are the second leading cause of disabilities in all age groups.3 Moreover, reported LBP also increases with age and often includes decreased participation in dayto- day occupational activities.4
The health-related impact of disabilities from LBP in dental practitioners results in increased medical care costs and decreased or lost income from diminished productivity.5 From a 5-year follow-up study, Leggat et al1 report that dentists with a higher prevalence of musculoskeletal disorders, particularly LBP, were more likely to leave the profession. In the general population, LBP accounts for approximately 40% of all lost work time due to musculoskeletal problems.2 In 2003, an estimated loss of $65 million was attributed to cancelled patient appointments when oral health professionals could not work due to musculoskeletal pain.6
As dental practitioners transitioned from standing to sitting working positions, the number of professionals reporting low back pain did not change, but there was a shift in affected areas.7 With prolonged standing, pain was experienced in the low back, legs, and feet. The standing affected lower limb circulation and caused postural defects such as flat feet. With prolonged sitting, pain is experienced in the low back, necks, shoulders, and arms.7 For all individuals, whether sitting or standing, the lower back carries most of their weight.7 The problem is not the position per se, but static position throughout the workday. Within a work environment, both prolonged sitting and standing can have detrimental health effects. James Levine, MD, PhD, a Mayo Clinic endocrinologist, suggests that people were not built to sit for long periods, but rather made to stand and move.8 Prolonged sitting, especially in an imbalanced position, unaided by lumbar support, contributes to LBP. Thus oral health care professionals need to limit prolonged sitting using improper postures and poor ergonomics.
For individuals with LBP, simple movements, such as bending, switching from sitting to standing, and walking, become difficult. While recovery from LBP in its acute phase is often favorable for 80% to 90% of sufferers,9 an estimated 60% to 86% of those individuals suffer recurrences within the first year. If LBP reoccurs, appropriate interventions need to be identified. Repeated occurrences can lead to more serious limitations, such as loss of flexibility, strength, and endurance.
STRATEGIES FOR PREVENTION
 Low back pain does not have to be an occupational health hazard for oral health professionals. Identifying common causes and risk factors helps practitioners implement preventive measures. Risk factors and causes for LBP include: operator posture, patient positioning, and elements unique to dental environments such as lighting and stools.10,11 Table 1 provides a list of problems, causes, and recommendations for low back pain.7,11-20 Careful consideration of these factors helps to identify the influencing aspects and aids in recommendations for prevention.
Low back pain does not have to be an occupational health hazard for oral health professionals. Identifying common causes and risk factors helps practitioners implement preventive measures. Risk factors and causes for LBP include: operator posture, patient positioning, and elements unique to dental environments such as lighting and stools.10,11 Table 1 provides a list of problems, causes, and recommendations for low back pain.7,11-20 Careful consideration of these factors helps to identify the influencing aspects and aids in recommendations for prevention.
Maintaining a neutral body position is vital for a healthy working posture. The focal distance between the operator’s eye and the treatment object is key to determining and maintaining correct posture; consequently, more practitioners are electing to wear magnification loupes. However, to avoid the challenge of eye fatigue related to wearing loupes, clinicians should relax their eyes by not wearing the loupes during procedures such as greeting a patient, setting up or breaking down an operatory, and providing oral care instructions.
Droeze and Jonsson21 demonstrated that oral health professionals were more likely to change work habits related to LBP when they received individualized treatment recommendations provided by physicians and physical therapists. For example, muscle imbalances may be part of a person’s current posture and muscle use patterns or they can develop over time. Oral health practitioners who remain seated and do not correct or change their posture periodically may develop a muscle imbalance between the abdominals and the low back extensors. Static sitting and leaning forward to work over a patient can stretch and overwork the low back extensors (multifidus and erector spinae), while the abdominals muscles (transverse abdominis, rectus abdominis, external and internal obliques) become weaker from decreased use and a shortened position.7
 An additional problem from prolonged sitting is the pressure put on the spine. In unsupported sitting, the pressure on the spine is 40% more than standing, but in sitting in forward flexion and rotating, the pressure increases to 400%.7 Over time, the muscle imbalances and influences on the ligaments and disks from increased pressure accumulate and may affect the spinal structure, which may lead to more serious complications such as a herniated disk.22 If pain is persistent (more than 3 months) or there are other signs of serious problems, such as pain down the leg, the practitioner should seek medical care.22-24
An additional problem from prolonged sitting is the pressure put on the spine. In unsupported sitting, the pressure on the spine is 40% more than standing, but in sitting in forward flexion and rotating, the pressure increases to 400%.7 Over time, the muscle imbalances and influences on the ligaments and disks from increased pressure accumulate and may affect the spinal structure, which may lead to more serious complications such as a herniated disk.22 If pain is persistent (more than 3 months) or there are other signs of serious problems, such as pain down the leg, the practitioner should seek medical care.22-24
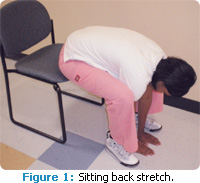
Acute back problems may become chronic because of additional factors such as decreased physical conditioning, muscle imbalances, muscle patterns of use, or more serious medical conditions such as a herniated disk.22 While physical conditioning does change with age, the lack of activity can hasten the process. Changes in physical condition can mean decreased health-related fitness components of endurance, strength, and flexibility. Incorporating aerobics, strength training, and stretching into the daily routine can help maintain body health, as well as provide pain relief during episodes of acute LBP if performed gently.23 Table 2 provides a list of exercises to prevent and manage LBP. A quick stretch that can easily be done between patients is sitting at the front edge of a sturdy chair and leaning forward from the waist reaching hands to the floor—remember not to twist. This exercise widens the spaces between the vertebrae and stretches the back muscles (See Figure 1).
A physician can determine if the back problem is limited to one site (eg, spinal stenosis, sciatica, herniated disc) or if it is a systemic problem (eg, arthritis) and recommend appropriate treatment.9,22 A physical therapist can evaluate the problem and provide an individualized assessment including movement analysis and environmental appraisal, and then develop a program tailored to specific problems. Physical therapists have several treatment options that can help patients with LBP whether due to degenerative disk disease or other causes.24,25 For example, intervention may include strengthening of core muscle groups, specifically abdominal wall and lumbar musculature, and hands-on therapy to mobilize the spine, all of which can have a positive effect in patients with LBP.24,25
CONCLUSION
LBP may appear to be an occupational hazard that cannot be avoided, but several actions can be taken to modify risk factors or address negative cumulative effects. Attention to work-related ergonomics and health-related components of fitness can provide ways to prevent and manage low back problems. Sitting does not have to be detrimental to health. Standing and moving around, making sure the stool’s lumbar support is properly adjusted, using loupes, and incorporating mild low back stretching exercises into the day can help dental professionals maintain a healthy back and overall good health.
REFERENCES
- Leggat PA, Redjarune U, Smith DR. Occupational health problems in modern dentistry: a review. Indust Health. 2007;45:611-621.
- Vital and Health Statistics Summary Health Statistics for U.S. Adults: National Health Interview Survey, 2009. Available at: www.cdc.gov/nchs/nhis.htm. Accessed: January 25, 2011.
- Alexopoulos EC, Stathi I-C, Charizani F. Prevalence of musculoskeletal disorders in dentists. BMC Musculoskelet Disord. 2004;9;5:16.
- Centers for Disease Control and Prevention (CDC). Prevalence and most common causes of disability among adults–United States, 2005. MMWR Morb Mortal Wkly Rep. 2009;58:421-426.5. Epidemiology of Musculoskeletal Pain-Fact sheet. Available at: http://www.iasp-pain.org/Content/NavigationMenu/GlobalYearAgainstCancerPain/20092010MusculoskeletalPain/FactSheets/default.htm. Accessed January 13, 2011.
- Hedge A. Back care for dentists and surgeons. Available at: http://www.spineuniverse.com/wellness/ergonomics/back-care-dentist-surgeons.Accessed January 13, 2011.
- Valachi B, Valachi K. Mechanisms leading to musculoskeletal disorders of dentistry. J Am Dent Assoc. 2003;134:1344-1350.
- Levine JA. Can too much sitting hurt your health? Available at: www.mayoclinic.com/health/sitting/AN02082. Accessed January 13, 2011.
- Kinkade S. Evaluation and treatment of acute low back pain. Am Fam Phys. 2001; 75:1181-1188, 1190-1192.
- White S. Ergonomics. How does dentistry fit you? Available at: www.dentistryiq.com/index/display/article-display/201885/articles/woman-dentist-journal/volume-1/issue-1/features/ergonomics-how-does-dentistry-fit-you.html. Accessed: January 13, 2011.
- Valachi B, Valachi K. Preventing musculoskeletal disorders in clinical dentistry: strategies to address mechanisms leading to musculoskeletal disorders. J Am Dent Assoc. 2003;134:1604-1612.
- Valachi B. Neck, back & beyond: preventing pain for peak productivity. Available at: www.vsds.org/_ah/editor/documents/Program8_Valachi_Handout.pdf. Accessed: January 13, 2010.
- Maillet JP, Millar AM, Burke JM, Maillet MA, Maillet WA, Feish NR. Effects of magnification loupes on dental hygiene student posture. J Dent Educ. 2008;72:33-44.
- Congdon LM, Tolle SL, Darby ML. Magnifying loupes in U.S. entry-level dental hygiene. J Dent Hyg. 2010,84:203.
- Rucker LM, Sunell S. Ergonomics risk factors associated with clinical dentistry. Available at: www.cda.org/library/cda_member/pubs/journal/jour0202/ergonomic.html. Accessed: January 13, 2011.
- Ratzon NV, Yaros T, Mizlik A, Kanner T. Musculoskeletal symptoms among dentists in relation to work posture. Work. 2000;15:153-158.
- Yoser AJ, Mito R. Injury prevention for the practice of dentistry. Available at: www.cda.org/library/cda_member/pubs/journal/jour0202/injuryprevention.html. Accessed: January 13, 2011.
- Cherniack MG, Dussetschleger J, Bjor B. Musculosketetal disease and disability in dentists. Work.2010,35:411-418.
- Valachi B. Move it: Physical movement is key to preventing musculoskeletal problems. Dental Practice Report. 2006;14,52-54.
- Prather H, Foye PM, Stiens SA, Wilder RP, Cianca JC. Industrial medicine and acute musculoskeletal rehabilitation 6 occupational health in special populations. Arch Phys Med Rehabil. 2002;83:S25-32.
- Droeze EH, Jonsson H. Evaluation of ergonomic interventions to reduce musculoskeletal disorders of dentists in the Netherlands. Work. 2005;25:211–220.
- Andersson G. Epidemiological features of chronic Low-back pain. Lancet. 1999; 354:581–85.
- Back pain health center. Available at: www.webmd.com/back-pain/exercises-to-reduce-low-back-pain. Accessed January 13, 2011.
- Lewis A, Morris M, Walsh C. Are physiotherapy exercises effective in reducing chronic low back pain? Phys Ther Rev. 2008;13: 37-43.
- Physical therapy is effective for management of low-back pain: a “cornerstone” of non-surgical treatment, a new report concludes. Available at: www.apta.org_AM_Template.cfm_Section=Home&Template=_CM_ContentDisplay.pdf. Accessed: January 13, 2011.
From Dimensions of Dental Hygiene. January 2011; 9(1): 36, 38, 40-41.

