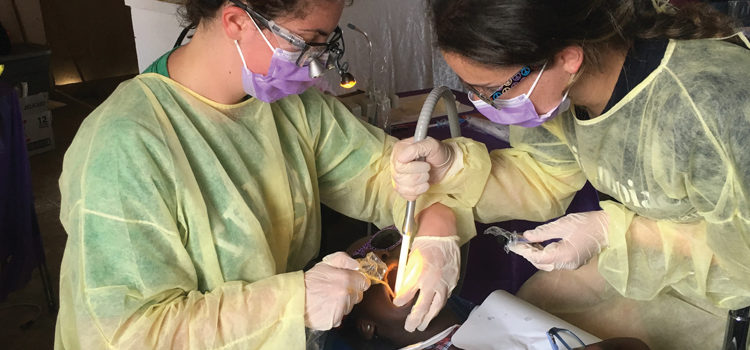
An Interprofessional Approach to Ergonomics
A collaboration between occupational therapy and dental hygiene departments increased awareness of the common pitfalls that lead to musculoskeletal disorders in the dental setting.
An interprofessional educational collaboration between occupational therapy and dental hygiene departments from different institutions was developed to promote children’s oral health. As assessment of dental hygiene work practices and positioning is the foundation for developing solutions to prevent, decrease, or eliminate pain and improve musculoskeletal health, this collaboration also included the occupational therapy students observing and assisting dental hygiene students during the delivery of oral health services (Figure 1). Both groups purposefully planned observations and interactions to create an awareness and appreciation of each other’s expertise. These observations and interactions created a secondary goal: to develop work environment alternatives that promote appropriate body mechanics.
Research has yielded evidence of negative health consequences associated with prolonged sitting.1,2 Research indicates that sitting for prolonged periods directly correlates to a higher risk for negative health outcomes despite physical activity outside work. However, a complete switch to prolonged standing promotes swelling in the legs and discomfort in the lower back.3 Thus, movement and change of positions throughout the day is advocated.
Studies suggest that the total duration of sitting time and the extent to which sitting time is accumulated in uninterrupted periods relate to mortality risk. In a recent study of 8,000 subjects followed for 4 years, those who sat for less than 30 minutes at a time had a 55% lower risk of death compared with those who sat for more than 30 minutes at a time.4 Moving (eg, walking, stretching, or changing positions) every 30 minutes is recommended. This will minimize a buildup of tense musculature, promote blood flow, and balance musculature.
STRETCHING AND BODY MECHANICS
Static stretching is the traditional approach to increasing the length of the musculo-tendinous unit (MTU) in order to lengthen shortened tissue and balance musculature. Static stretching involves moving a muscle into the position opposite the typical static position and holding it for 10 seconds to 30 seconds. The MTU elongates when subsequent stretches are held at a slightly increased range.5 Systematic reviews suggest that stretching can help decrease musculoskeletal discomfort, pain, and increase joint motion in a variety of occupations.6,7 However, stretching does not substantially prevent exercise-related injuries associated with sports.7
Options to counter prolonged sitting have been examined relative to productivity, comfort, general acceptance of alternatives, and satisfaction.8 One challenge is simply remembering to stretch. Marangoni9 compared the frequency of stretching and found that subjects using computer-generated and hard copy reminders of stretching completed significantly more stretches than the control group.9 For dental hygienists, hard copies with alarm reminders may be most practical. In essence, oral health professionals should move every 30 minutes.
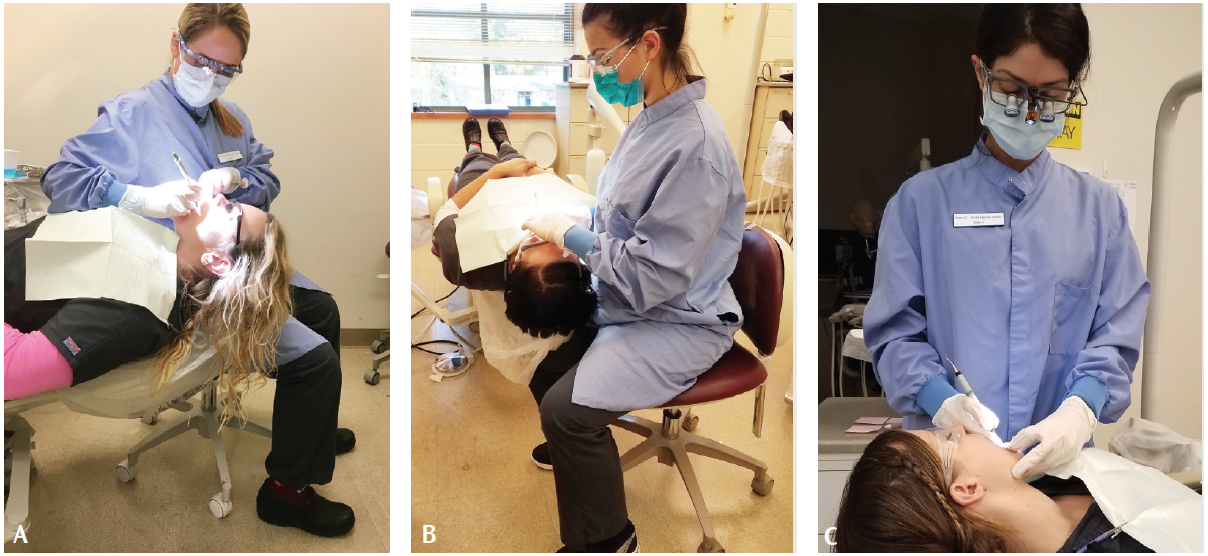
The dental hygiene/occupational therapy collaboration focused on promoting neutral posture for dental hygienists. Neutral posture is the position of the neck, shoulders, elbows, hips, and knees in which the flexor and extensor muscles of the body are balanced. This position is typically the mid-position of the joints: neck upright, shoulders relaxed, upper arms at sides, elbows flexed to 90°, wrists straight, and fingers relaxed. These positions promote an energy efficient use of muscles throughout the day.10 However, in dental hygiene work, excessive forward neck flexion, slouching, reaching, and twisting are not uncommon.
ADJUSTING CHAIRS/STOOLS AND HEADRESTS
An adjustable clinician chair/stool with a tilt mechanism offers dental hygienists the opportunity for closer seating to the patient and helps maintain the lower curvature back. Oral health professionals should adjust the seat height with the back and thighs at approximately 110° with the hips higher than the knees and forward seat tilt angled at 15°.11 Another option to the traditional clinician chair is the saddle stool, which offers a different option to maintain a natural curvature of the spine. The saddle stool positions the thighs downward at a 45° angle producing a stance between standing and sitting.12 There are occasions when the patient is reclined and the clinician cannot access the 12 o’clock position due to lack of space. Most patient chairs have a swivel mechanism to angle the chair or other equipment may need to be adjusted to improve access. The saddle stool also requires less space, improving access behind the patient between the 11 o’clock and 1 o’clock positions.
A double articulating headrest allows the patient’s head to be positioned for maxillary and mandibular access. The headrest should be adjusted to support the back of the patient’s head while seated upright. Once the patient’s chair is reclined to a supine or semi-supine position, the patient should reposition his/her head on the headrest. For maxillary teeth the patient should be in a supine position with the head tilted back with the chin up; for mandibular the teeth a semi-supine position should be assumed with the chin tilted down. Some headrests are not comfortable for tilting the head back. Various headrest cushions are available or a towel can be rolled and placed under the neck to cushion the occipital bone. As the patient is positioned, the clinician’s thighs should freely fit under the patient’s chair with the ability to easily move around patient’s head.
To enable his or her own chair to move efficiently, the oral health professional may raise the back of the patient’s chair. However, care must be taken to not raise the patient chair too high, which would cause the clinician’s arms to abduct from the body. Sustained shoulder abduction contributes to both neck and shoulder fatigue. If the patient is positioned too high or too low, shoulder strain/fatigue may occur.1 The headrest should be extended to improve access to the patient while enabling the clinician to move effortlessly around the patient’s head.
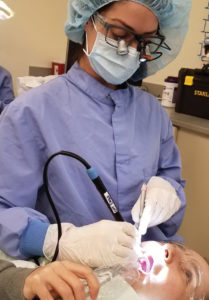
CLINICIAN MOVEMENT AROUND THE PATIENT
A study revealed that less awkward positions were noted in dental hygienists at 11:00 o’clock vs 7:00 o’clock seating position.13 Although proper body mechanics should be followed as much as possible; there are circumstances when clinicians need to be in an awkward position to access a specific area in the oral cavity.13
Traditionally, right-handed clinicians access the oral cavity from 8:00 o’clock to 12:00 o’clock and left-handed clinicians use 12:00 o’clock to 4:00 o’clock positions.14 More recent thinking has right-handed clinicians’ radius from 8:00 o’clock to 2:00 o’clock and 10:00 o’clock to 2:00 o’clock range for left-handed clinicians.15 Rucker et al16 found that all areas for the right-handed clinician can be accessed from 10:00 o’clock to 12:30 o’clock and left-handed clinician 11:30 o’clock to 2:00 o’clock. A 7:00 o’clock to 9:00 o’clock range causes the right-handed clinician (3:00 o’clock to 5:00 o’clock for left-handed clinicians) to access the oral cavity with awkward postures of torso twisting and abduction of arms.16The awkward position of torso twisting occurs from side sitting and can contribute to musculoskeletal disorders due to an imbalance of the clinicians’ musculature over time.
The dental hygienist’s awareness and reflection of awkward postures assist in recognizing alternatives to attain a more neutral posture while increasing visibility, access, and comfort (Figure 2 and Figure 3). However, following clock recommendations does not always lead to a balanced posture due to each clinician’s body stature, patients’ limitations in overall positioning, ability to maintain the oral cavity open, and crowding or missing teeth. Dental hygienists need to be mindful of their posture and minimize time spent in awkward positions.
Through this collaboration between occupational therapy and dental hygiene students, the ergonomics of dental hygiene practice were improved due to the assessment and feedback provided. Awareness and resourcefulness developed during the collaboration allowed the dental hygiene students to try alternatives in positioning in order to achieve a balanced working posture; hopefully, reducing their risk of musculoskeletal disorders once they begin clinical practice.
REFERENCES
- Ford ES, Kohl HW, Mokdad AH, Ajani UA. Sedentary behavior, physical activity, and the metabolic syndrome among US adults. Obesity Research, 2005; 13 (3): 608-14.
- Buckley, John P., et al. “Standing-based office work shows encouraging signs of attenuating post-prandial glycaemic excursion.” Occup Environ Med (2013): oemed-2013.
- Waters, Thomas R., and Robert B. Dick. “Evidence of health risks associated with prolonged standing at work and intervention effectiveness.” Rehabilitation Nursing. 2015; 40(3): 148-.
- Diaz KM, Howard VJ, Hutto B, Colabianchi N, Vena JE, Safford MM, et al. Patterns of Sedentary Behavior and Mortality in U.S. Middle-Aged and Older Adults: A National Cohort Study. Ann Intern Med. 2017;167:465–475.
- Bruno R, da Costa B, Vieira ER. Stretching to reduce work-related musculoskeletal disorders: a systematic review. J Rehabil Med. 2008;40:321–328.
- Sacco ICN, Rocha LE, Bragança CA, Casarotto RA. Stretching and joint mobilization exercises reduce call-center operators’ musculoskeletal discomfort and fatigue. Clinics. 2010;65(7):657-62.
- Small K , Naughton LM & Matthews M. A Systematic Review into the Efficacy of Static Stretching as Part of a Warm-Up for the Prevention of Exercise-Related Injury, Research in Sports Medicine. 2008;16(3):213-231.
- Karola S, Robertson MM. Implications of sit-stand and active workstations to counteract the adverse effects of sedentary work: A comprehensive review. Work. 2015; 52: 255–267.
- Marangoni AH. Effects of intermittent stretching exercises at work on musculoskeletal pain associated with the use of a personal computer and the influence of media on outcomes. Work. 2010; 36:27–37. DOI 10.3233/WOR-2010-1004
- Kroemer, K. H. E., & Grandjean, E. (2001). Fitting the task to the human (5th ed.). Philadelphia: Taylor & Francis.
- Yadav R, Rai R, Yadav A, Pahuja M, Solanki S. Ergonomics for pain free dental practice – a review. Int J of Information Research and Review. 2016; 3(6):2562-2565.
- Valachi B. The ergonomic benefits of saddle-style stools. DPR: Dental Products Reports. February 08, 2017. Available at http://www.dentalproductsreport.com/dental/article/ergonomic-benefits-saddle-style-stools. Accessed on October 14, 2017.
- Noh H, Roh H. Approach of Industrial Physical Therapy to Assessment of the Musculoskeletal System and Ergonomic Risk Factors of the Dental Hygienist. J Phys Ther Sci 2013; 25(7):821–826.
- Halaris JF, Wilkins E. Patient reception and ergonomic practice. In: Wilkins E, ed. Clinical Practice of the Dental Hygienist. 12th edition. Philadelpia, PA: Wolters Kluwer; 2017:104.
- Drummer LJ. Ergonomics. In: Darby ML, Walsh MM ed. Dental Hygiene Theory and Practice. Fourth edition. St. Louis, MO: Elsevier Saunders; 2015:148.
- Rucker LM, Sunell S, Wen M. Balanced Operator Position. Dental Clinical Ergonomics. The University of British Columbia. Available at https://secure.dentistry.ubc.ca/survey/app/fb_01/frameset.htm accessed on October 16, 2017.
From Dimensions of Dental Hygiene. January 2018;16(01):30-32.

