Addressing Chronic Periodontitis
Chronic periodontitis is an inflammatory destruction of the supporting apparatus of the teeth.
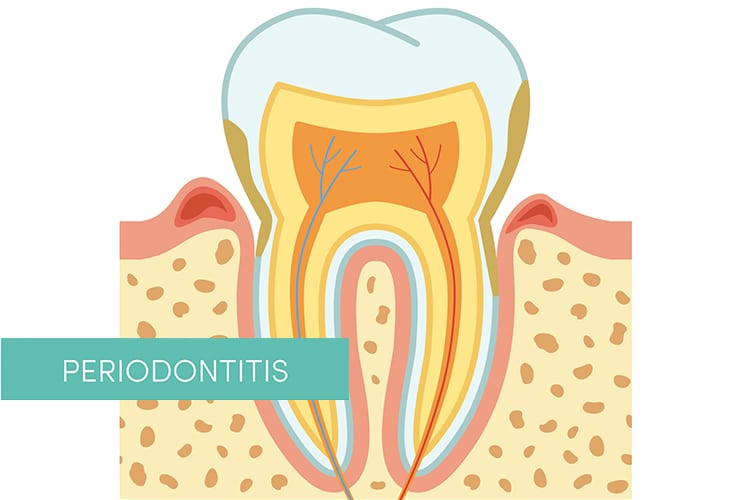
Chronic periodontitis is an inflammatory destruction of the supporting apparatus of the teeth. It results in inflammation and destruction of alveolar bone and the periodontal fibers that insert into cementum, thereby exposing cementum to dental plaque within a periodontal pocket. If left unchecked, the mechanical stability of a tooth may become compromised, or the localized chronic infection may become acute—both resulting in tooth loss. Early detection of the signs of chronic periodontitis is essential to halting disease progression and improving outcomes. As such, clinicians should be familiar with the subclassifications of chronic periodontitis, the tools used to assess and interpret its location and severity, and how to document anatomic changes over time.
Photo Credit: marina_ua / iStock / Getty Images Plus
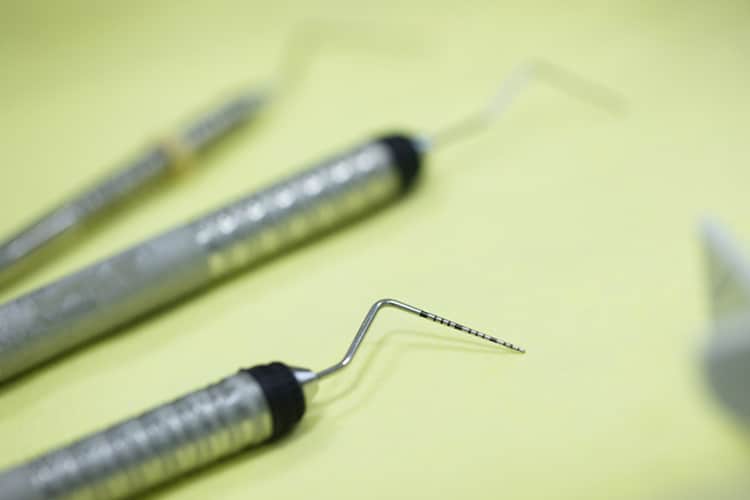
Probing Process
Probing and charting of periodontal tissues to assess clinical attachment losses and the use of radiography to evaluate the underlying osseous support and possible presence of furcation involvement are essential components of accurate periodontal assessment. Pocket probing depths (or sulcus depths) are measured using gentle pressure from the gingival margin to the most coronal aspects of the junctional epithelium while paralleling the long axis of the tooth. Because inflamed epithelium is easily penetrated by periodontal probing, true periodontal pocket depths can only be determined histologically. Therefore, the term “probing depth” is preferred over “pocket depth” for clinical assessments.
Photo Credit: zlikovec / iStock / Getty Images Plus
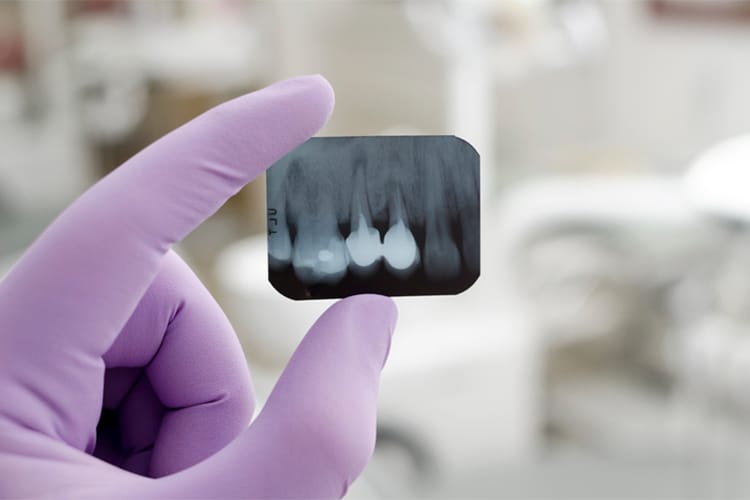
Radiographs
Intra- and extraoral radiographs are used to assess the apical-coronal extent of alveolar bone present, and they may serve as a baseline record for future comparisons aimed at detecting longitudinal changes in bone dimensions and densities. Bitewing and periapical radiographs are most commonly used. They are generally easy to acquire, inexpensive, and provide reasonable resolutions. Optimal bitewing radiographs are achieved with horizontal angulation perpendicular to the tooth surfaces and vertical angulation above or below perpendicular. Vertical bitewings using #2-size films are recommended in cases where bone loss > 4 mm in order to properly capture bone heights. A full-mouth series of radiographs is appropriate for a patient who may have chronic periodontitis to help detect any periapical pathoses that could produce localized drainage tracts, which can mimic chronic periodontitis. However, a full-mouth series is time consuming and periapical radiographs tend to be more geometrically distorted than bitewings.
Photo Credit: milosljubicic / iStock / Getty Images Plus
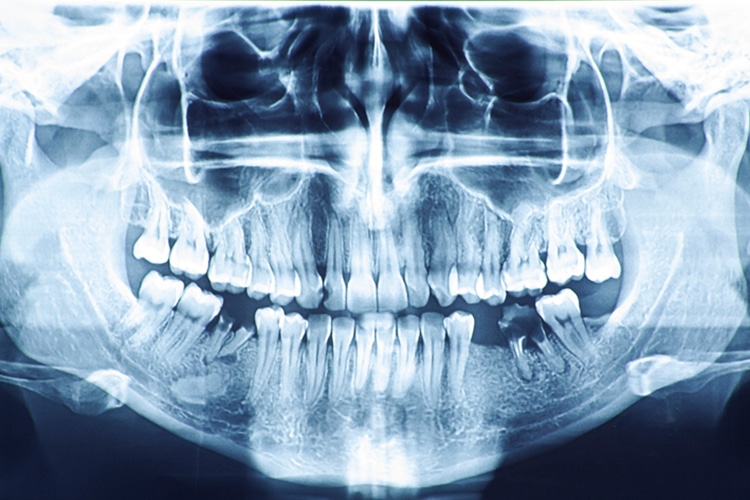
Digital Approach
Digital intraoral radiography may enhance the imaging of intraoral structures, while also reducing radiation exposure. Two-dimensional (2D) intraoral radiography, however, is difficult to standardize geometrically. An extraoral panoramic radiograph is another 2D image that can be used for viewing large areas. Unfortunately, this technique’s inherent distortions limit its diagnostic value for assessing subtle characteristics, such as alveolar bone levels.
Photo Credit: cioncabogdana / iStock / Getty Images Plus
Three-Dimensions
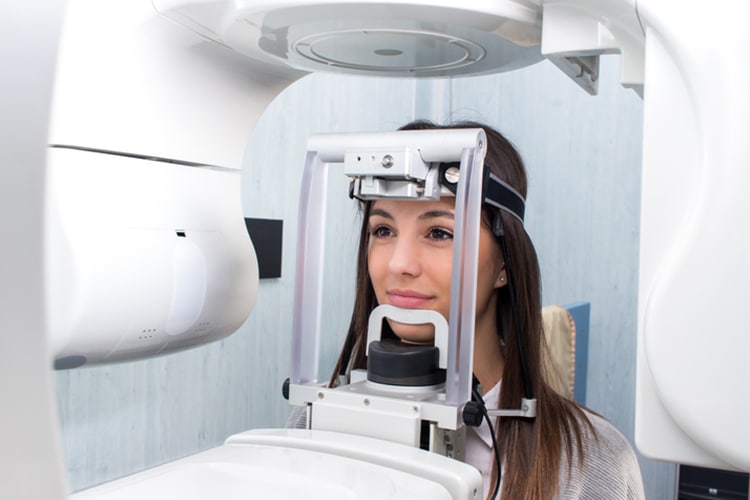
Cone-beam computed tomography (CBCT) provides a three-dimensional (3D) assessment of bony changes. The quality of images obtained by CBCT depends on acquisition parameters. To measure alveolar bone height, CBCT requires identification of the alveolar bone margin and the CEJ. The accuracy of identifying these intersections is limited by the size of each voxel in the image. Therefore, locating the CEJ on the CBCT image within the margin of error of a single voxel size should be possible. In contrast to the CEJ, the alveolar bone margin is the junction between cementum and bone. Here, the accuracy is limited by the physical spatial resolution of the image. To establish the bony changes characteristic of chronic periodontitis, images with better definition obtained by smaller voxel size are desirable, but this increases radiation exposure.
Photo Credit: karelnoppe / iStock / Getty Images Plus
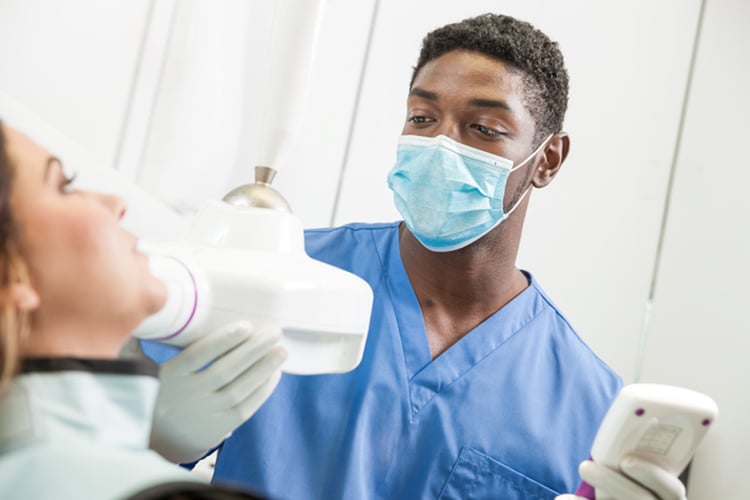
Healthy Bone
In radiographs, healthy alveolar bone presents as a thin line of what appears to be densely radiopaque bone that is continuous with the lamina dura of adjacent teeth. The lamina dura can be seen starting approximately 0.5 mm to 2.0 mm apical to tooth roots. Clinically, bone loss can be classified into horizontal and angular (vertical) defects. It runs parallel to an imaginary line joining cementoenamel junctions of adjacent teeth, and can be further classified as mild, moderate, or severe.

