The Role of Sealants in Caries Prevention
Many interventions can help prevent dental caries, such as topical fluoride application, community water fluoridation, reducing the accumulation of oral biofilm, and dietary counseling.
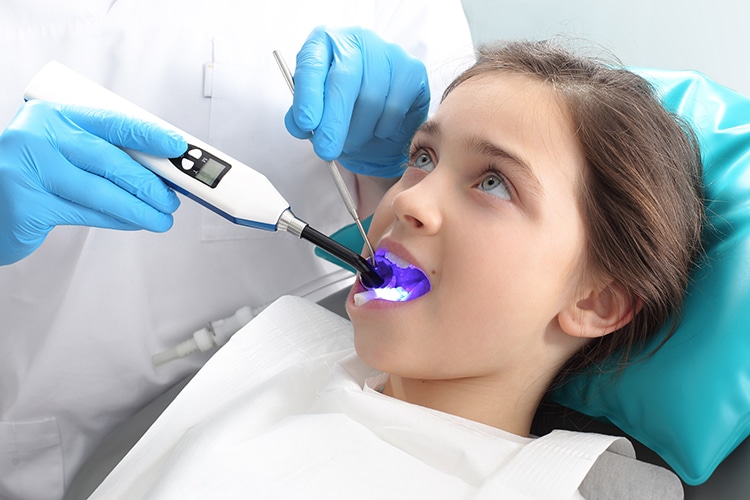
Many interventions can help prevent dental caries, such as topical fluoride application, community water fluoridation, reducing the accumulation of oral biofilm, and dietary counseling. However, due to the tooth’s anatomical morphology, sealant placement is an integral part of comprehensive caries management. This is especially true in the posterior teeth that present with more pits and fissures. Pits and fissures have a greater level of biofilm retention, thus, a higher risk of caries development. Furthermore, fluoride treatments, modification in diet, and biofilm control are most effective on smooth-surface caries vs decay in the pit and fissures. As an estimated 90% of carious lesions occur in pits and fissures, additional interventions, such as sealants, are vital to prevent tooth decay.
Photo Credit: robertprzybysz / iStock / Getty Images Plus

Providing a Barrier
Sealants are part of both primary and secondary caries-prevention measures. Sealants can prevent the initial onset of caries by providing a physical barrier between cariogenic bacteria and the tooth’s surface. This barrier inhibits cariogenic microorganisms and food debris from accumulating in deep pits and fissures, thus, decreasing the likelihood of carious lesion formation. Additionally, a panel study performed by the American Dental Association Council on Scientific Affairs concluded that sealants are not only effective in caries prevention but can also halt the progression of early noncavitated caries lesions and arrest the proliferation of cariogenic bacteria. In fact, when bacteria levels were assessed after sealant placement over a caries lesion, the number of viable bacteria decreased by 100 fold and the number of lesions with any remaining viable bacteria were reduced by 50%. This reduction in active cariogenic bacteria can decrease future caries development and the need for restorative intervention.
Photo Credit: ittipon2002 / iStock / Getty Images Plus
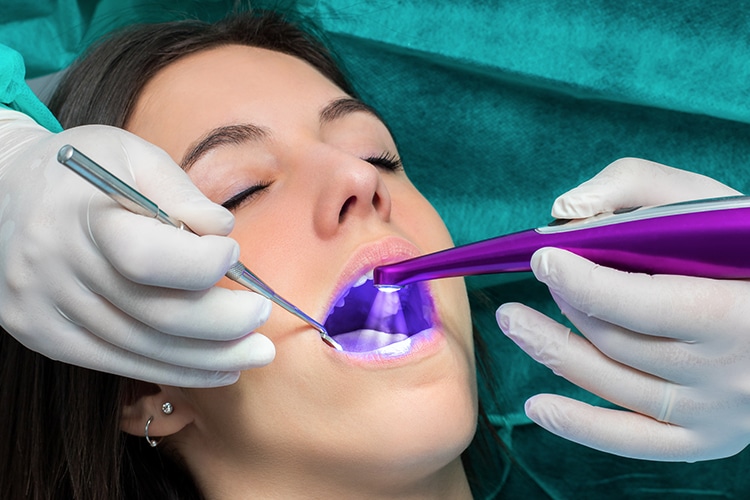
Retention Techniques
Sealant retention is an important factor to consider when evaluating a material’s efficacy. To provide the greatest level of protection, sealants should be applied as early as possible and be evaluated for retention at each dental hygiene visit, as retention rates decrease over time. Variables that affect the retention and longevity of sealants have been widely studied. With the exception of moisture contamination risk (although not all sealant products require a dry field), surface pretreatment techniques are one of the most significant factors affecting sealant retention. These pretreatment techniques include traditional acid etching, laser preparation, ultrasound preparation, and the use of classical burs to remove debris from pits and fissures.
Photo Credit: ayo888 / iStock / Getty Images Plus
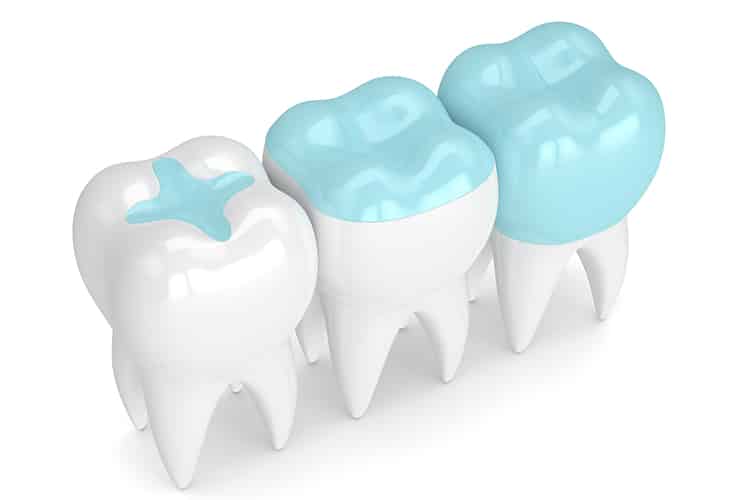
Sealant Types
There are two main types of sealant material based on the reaction that takes place as the material sets: resin-based and glass ionomer. Resin-based sealants are light-cured, causing a polymerization reaction to set the material, while glass ionomers have an acid-based reaction. Hybrids of the two materials also exist, contributing to a variety of differences in the material properties, tensile strength, shrinkage rate, ease of application, and fluoride release. A 2016 systematic review stated there was insufficient evidence to provide specific recommendations of one type of sealant material over another. Resin-based sealants offer superior retention capability. Some resin-based sealants require a dry field. Glass ionomer materials bond directly to enamel, increasing the ease of application and alleviating the need to acid etch. Glass ionomer materials also can act as a rechargeable fluoride reservoir after exogenous fluoride application and release fluoride into the tooth. However, glass-ionomer sealants do not offer the same longevity as resin-based sealants.

