
With the current COVID-19 pandemic, there is a great deal of commentary about the airborne spread of disease. All of us who practice clinical dentistry know that dental procedures tend to produce copious airborne materials. The potential for these airborne particles to carry the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) from an infected patient to dental personnel—including dentists, dental hygienists, dental assistants, and office staff—is a major concern. Transmission from dental team members to patients is also a possibility.
Photo Credit: MichaelSapryhin / iStock / Getty Images Plus
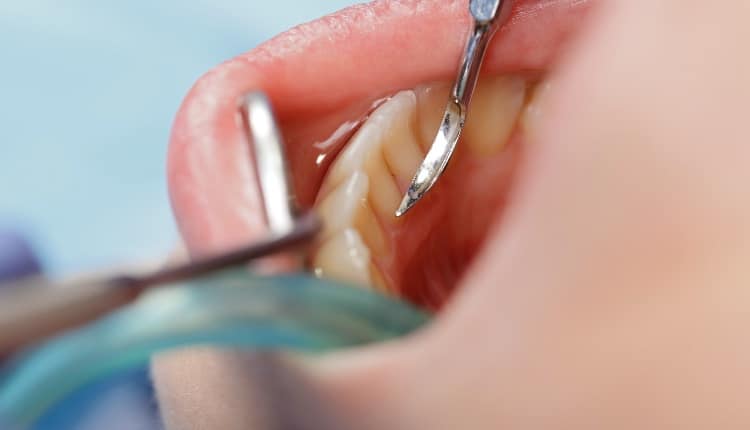
The Cloud Created by Ultrasonic Use
The cloud created by ultrasonic use contains splatter, aerosols, and droplet nuclei. All the material we see comes under the heading of spatter. By definition, if the airborne particle is large enough that it can be seen, it is spatter. By definition, aerosols are too small to be seen with the naked eye. Most industrial hygiene professionals define aerosols as particles less than 50 microns (about the diameter of a human hair). Beginning as spatter but, as the water component of the spatter starts to evaporate and particle size and weight diminish, droplet nuclei become light enough to become aerosols. This may be the greatest concern with dental infection control, as droplet nuclei exit the mouth as relatively large particles and therefore are able to contain more biological material from the patient.
Photo Credit: Ocskaymark / iStock / Getty Images Plus
Risks Posed by COVID-19-Containing Aerosols
The most likely danger will come from the asymptomatic individual with COVID-19 who is shedding the virus. The news media has reported on studies that indicate approximately 30% to 50% of many populations are asymptomatic carriers of the virus. The best approach would be to test all patients for the virus when they arrive at the office. While point-of-care testing is not possible at this time, there is a high probability this will become possible and perhaps mandatory in the near future.
Photo Credit: fpm / iStock / Getty Images Plus

Draping the Operatory
Most dental settings have many flat surfaces and cabinets. In addition, various pieces of equipment are often stored in treatment rooms. Dental teams should drape this equipment, as is routinely done in a medical operating room. Only the items that will be used on the current patient should be exposed to aerosols and spatter. The fronts of cabinets, flat surfaces (such as tray tables and Mayo stands), and equipment (such as radiography units and scanning devices) should be draped. It would be best if these drapes were replaced after each patient, but plastic drapes could be wiped down with disinfectants.
Photo Credit: Maridav / iStock / Getty Images Plus

Preprocedural Mouthrinses
In many offices, it is routine to have the patient rinse with chlorhexidine (CHX) prior to treatment. Early studies have indicated that while CHX will reduce the viral load of SARS-CoV-2, a diluted hydrogen peroxide or diluted bleach mouthrinse is more effective in killing the virus. The currently recommended dilution for hydrogen peroxide is 1% to 1.5%. Commercially available hydrogen peroxide is 3%, so a 1:1 dilution with water will yield the recommended rinse. The dilution of bleach varies considerably, with a capful of bleach to 1 liter of water as one of the recommendations.
Photo Credit: Ivan Pantic / iStock / Getty Images Plus

Use of High-Volume Evacuation
Almost all dental offices have an evacuator system that is capable of removing a high volume of air/droplets/aerosols from the operating field. High-volume evacuation is usually performed by an assistant using a large-bore, disposable evacuation tip. The inside diameter of a large-bore evacuator tip is 13 mm or greater. This large internal size allows for a high volume of material to be removed from the treatment area, and has been shown to reduce the number of bacteria produced during various procedures by 90% to 95%. Various high-volume vacuum devices that fit in the patient’s mouth and fit around an ultrasonic tip are available that allow for high-volume evacuation without the need for a dental assistant.
Photo Credit: skynesher / E+

Reduction of Material From the Nasopharynx
An important risk of aerosols and spatter that is not directly associated with the dental procedure comes from the patient’s normal respiration. During care, the patient is breathing directly in the practitioners’ faces. While high-filtration (eg, N95) masks will filter out a large amount of viral particles, as the name implies, they will only filter 95% of the potentially infectious material. I recommend the use of a facial surgical drape for the patient. These are commonly used in oral surgeries, but are rarely used in other dental procedures. These drapes consist of a disposable sheet that covers the patient’s nose, eyes, and hair, while having an opening that allows access to the oral cavity. This drape will “put a mask” on the patient’s nose and help block any particles exhaled through the nose. This drape will also act to absorb much of the spatter that originates from the mouth and, as a disposable item, will be thrown away after the procedure.
Photo Credit: Liliboas / iStock / Getty Images Plus

Personal Protective Equipment
As of this writing, the recommendations for personal protective equipment (PPE) are rapidly changing. Some are recommending full environmental protection, such as gowns with masks and independent filtered breathing equipment. While ideal, this level of protection is impractical at this time. It is likely the universal use of existing protective gear, with the addition of high-filtration masks (eg, N95) will be the norm for the foreseeable future. As a minimum, these must include a high-filtration mask, goggles or safety glasses with side shields, face shield, hair covering, and a disposable gown. Many clinicians currently practice in short-sleeved scrubs with a standard surgical mask and their routinely used glasses. This is inadequate to protect against SARS-CoV-2 infection. All of the items previously listed are necessary during treatment of every patient; in addition, all disposable items should be changed between each patient and nondisposable items wiped down with disinfectant.

