Impact of Bisphosphonates on Oral Health
Osteoporosis can impact a patient’s quality of life due to the possibility of bone fractures.
Osteoporosis can impact a patient’s quality of life due to the possibility of bone fractures. Antiresorptive medications—such as bisphosphonates and receptor activator of nuclear factor kappa-Β ligand (RANKL) inhibitors, which help in the management of osteoporosis—are commonly prescribed. Antiresorptive therapies for individuals with osteoporosis include five principal classes of agents: bisphosphonates, estrogens, selective estrogen receptor modulators, calcitonin, and monoclonal antibodies, such as denosumab. While each has the potential to cause osteonecrosis, bisphosphonates are the main focus of this article because they are the most commonly prescribed antiresorptive agents. As such, clinicians should be mindful of strategies that can help these patients maintain optimum oral health.
Photo Credit: Goldfinch4ever / iStock / Getty Images Plus
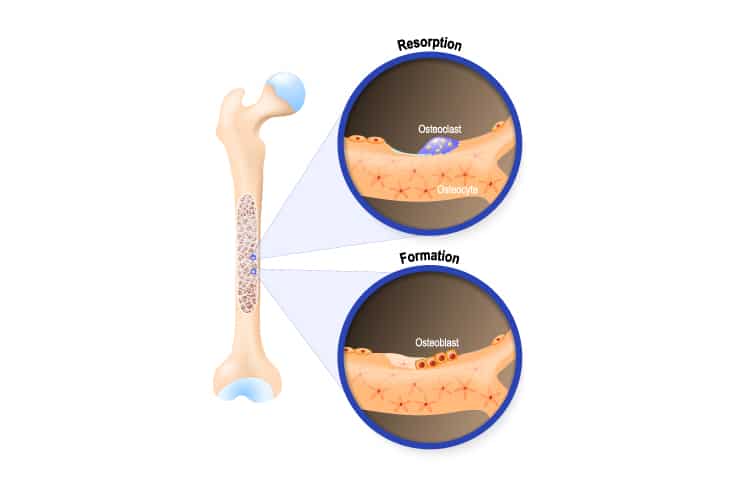
Mechanism of Action
Bisphosphonates inhibit osteoclastic bone resorption in a different fashion than other antiresorptive agents. They attach to hydroxyapatite binding sites on bony surfaces undergoing active resorption, where they impair the ability of the osteoclasts to form the ruffled border, adhere to the bony surface, and produce the protons necessary for continued bone resorption. They also reduce osteoclast activity by decreasing osteoclast progenitor development and recruitment, and by promoting osteoclast apoptosis.
Photo Credit: ttsz / iStock / Getty Images Plus
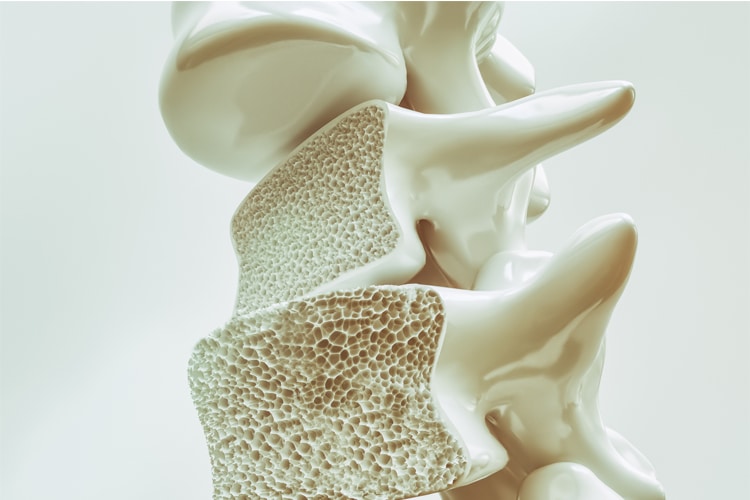
Treatment
In defining the staging and treatment of medication-related osteonecrosis of the jaw, the American Association of Oral and Maxillofacial Surgeons (AAOMS) task force classified patients into five categories, ranging from a patient presenting with no symptoms and needing no treatment to individuals in stages 0, 1, 2, and 3. Various stages require different treatment strategies. For example, pain management and infection control are necessary for each stage, while surgical treatment is indicated for stages 2 and 3. Stage 3 will likely require surgical debridement, with possible resection of sites. However, studies have indicated that surgical procedures in stages 1 and 2 may help achieve optimal results.
Photo Credit: CreVis2 / iStock / Getty Images Plus
Drug Holiday
The role of a “drug holiday” remains controversial. In 2009, the AAOMS recommended withholding oral bisphosphonates for up to 3 months before and after a surgical procedure. However, a recent study by Hasegawa et al did not support the effectiveness of a drug holiday on the outcome of medication-related osteonecrosis of the jaw in patients taking oral bisphosphonates. For patient on IV bisphosphonates, short-term discontinuation might not allow for better outcomes, while long-term discontinuation might be beneficial in stabilizing established sites of medication-related osteonecrosis of the jaw, reducing the risk of new site development and clinical symptoms. Based on the recommendation of McClung et al, the decision to discontinue antiresorptive medication relies on the patient’s fracture risk, T score, and history of hip or spine fracture. Discussion with the patient’s physician regarding cessation of bisphosphonates is mandatory in medication-related osteonecrosis of the jaw treatment.
Photo Credit: Rawf8 / iStock / Getty Images Plus

Dental Management
For patients taking these drugs, good oral hygiene and regular dental visits are essential. Prior to starting bisphosphonate therapy, addressing existing dental issues is a best-practice strategy. Generally speaking, if routine dental treatment—such as prophylaxis, fluoride carriers, dental restorations, or dentures—is indicated, no special precautions are required for these patients. However, if more invasive treatment is needed, such as extractions, periodontal surgery, or surgical root canal treatment, use of bisphosphonates should be delayed for a month to allow sufficient time for bone recovery and healing.

