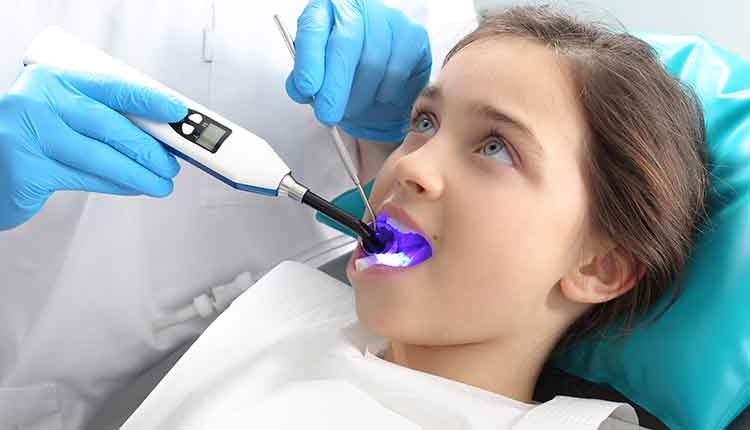
A strong research base demonstrates that dental sealants are highly effective in preventing tooth decay. Sealants can reduce the risk of decay in permanent molars by 80% in the first 2 years after application and continue to work after more than 4 years post-application. Given this evidence, the United States Centers for Disease Control and Prevention, Association of State and Territorial Dental Directors, and several other health organizations support sealant programs in schools to deliver preventive care to low-income children. Yet, 61% of low-income children ages 6 to 11 lack sealants. And the Pew Report released by the Pew Charitable Trusts found that school sealant programs are in fewer than half of high-need schools in 39 states.
Photo Credit: valentinrussanov / E+

Barriers Faced
There are numerous reasons for our nation’s underdeveloped school-based oral health prevention infrastructure. Featuring prominently are a range of state-based regulations or policies that either limit or prohibit dental hygienists from sealing children’s teeth at school or create financial burdens that impede the expansion of school-based sealant programs. These barriers can be found mainly in state practice acts—which define scope of practice for dental hygienists—and Medicaid policies.
Photo Credit: sorbetto / DigitalVision Vectors

Prior Exam Rules
Prior exam rules require that a student be examined by a dentist before receiving a sealant in school from a dental hygienist. These requirements exist because regulators are concerned that a dental hygienist cannot identify which molars are candidates for sealants, even though they are trained to do so. Research finds that labor accounts for about two-thirds of the cost per child of a school sealant program. Program costs are lower when dental hygienists, instead of dentists, are making sealant determinations. Currently, prior exam rules still remain in the District of Columbia, Alabama, Delaware, Hawaii, Louisiana, Mississippi, North Carolina, and Texas.
Photo Credit: Pavlo Stavnichuk / iStock / Getty Images Plus

Employment Requirements
In Kentucky and Virginia, only government employees can supervise public health dental hygienists. This requirement does not allow for an ample supply of school-based dental hygienists given the history of budget cuts for state and local public health departments. Without this restriction, private practices and nonprofits could participate. Other states place strict limits on the number of public health dental hygienists that any one dentist can supervise. For instance, in North Carolina, a dentist can supervise no more than two public health dental hygienists at a time. When dentist supervision is a requirement, as it is in nearly all states with public health hygienists, narrowing the pool of available supervisors limits the potential for program growth.
Photo Credit: sdecoret / iStock / Getty Images Plus

Reimbursement Based on Location
Medicaid is the dental insurer for nearly 80% of all low-income children and is a major funding source for school-based sealant programs. Dental directors in Alaska, Arkansas, Hawaii, and South Dakota said that Medicaid does not reimburse for care delivered outside of a traditional brick-and-mortar dental clinic or office.
Photo Credit: 3283197d_273 / iStock / Getty Images Plus

Restrictions on Direct Billing
Currently, 32 states and the District of Columbia do not allow dental hygienists to bill Medicaid directly for services. Instead, they must bill through their supervising dentists, requiring both clinical supervision and a financial arrangement to sustain the program. Eighteen of 44 dental directors identified this rule as a barrier. The inability to bill directly in many cases causes payment delays to programs. States also report that dentists are reluctant to supervise school-based hygienists because of lack of administrative capacity to handle billing.
Photo Credit: AndreyPopov / iStock / Getty Images Plus

Managed Care
In addition, some states that employ Medicaid managed care for dental services report that contracted insurers are not allowing dental hygienists to bill Medicaid directly, even though they can do so under the state’s Medicaid fee-for-service program.

