What Do You Do At The Reevaluation Appointment?
How long does your office wait after completion of four quadrants of scaling and root planing for reevaluation, and what do you do at that appointment?
QUESTION: How long does your office wait after completion of four quadrants of scaling and root planing for reevaluation, and what do you do at that appointment?
ANSWER: Reevaluation subsequent to completion of scaling and root planing should occur at a minimum of 3 weeks to 4 weeks. This period allows for resolution of periodontal inflammation and a gain in clinical attachment (Figure 1 and Figure 2). Both of these outcomes will result in a reduction of probing depths.
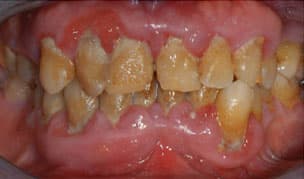
appointment prior to providing scaling and root planing.
In 1980, Morrison et al1 showed that the clinical severity of periodontitis was reduced in 1 month following scaling and root planing with a concomitant improvement in self-care. The 1-month interval was reinforced by Proye et al2 in 1982. In their investigation, improved parameters associated with periodontal health—particularly an increase in clinical attachment gain—occurred at 1 month, and these measurements were similar at 2-month and 3-month intervals. As a result of these investigations, a 1-month interval between providing scaling and root planing and the reevaluation was deemed the appropriate time interval for healing. Moreover, waiting too long for reevaluation may result in disease progression.
At the reevaluation, the oral health professional should reexamine the patient to determine if gingival indices have improved (ie, reduction in gingival inflammation and plaque scores). In addition, documentation of probing depths with a second periodontal charting should be completed to determine if a reduction of probing depths has occurred.
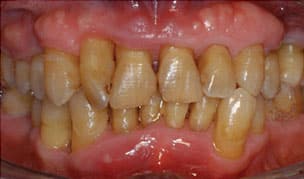
Another important element of the reevaluation appointment is to make a treatment plan regarding future management of the patient’s periodontal condition. If probing depths are 3 mm or less, maintenance may be all that is needed. Four mm to 5 mm probing depths could benefit from additional nonsurgical periodontal therapy, which may include systemic antibiotics or local antibiotic/antimicrobial therapy.
Deep probing depths associated with radiographic indication of angular bone loss may trigger decision-making regarding surgical access to diseased root surfaces. Recommended surgical procedures could provide pocket reduction via regeneration or resective therapy. Moreover, the presence of gingival recession and an associated mucogingival deformity may warrant therapy with a gingival augmentation procedure.
Determining the need for maintenance and possible surgical therapy should be discussed with the patient at the reevaluation appointment. In addition, the reevaluation visit could include a review of self-care; smoking/vaping cessation; diet, especially relating to type II diabetes; and any other risk factors associated with the potential for future periodontal attachment loss and caries.
REFERENCES
- Morrison EC, Ramfjord SP, Hill RW. Short term effects of initial, nonsurgical periodontal treatment. J Clin Perio Periodontol. 1980;7:199–211.
- Proye M, Caton J, Polson A. Initial healing periodontal pockets after a single episode and root planing monitored by control probing forces. J Periodontol. 1982;53:296–301.
From Dimensions of Dental Hygiene. July/August 2019;17(7):56.

