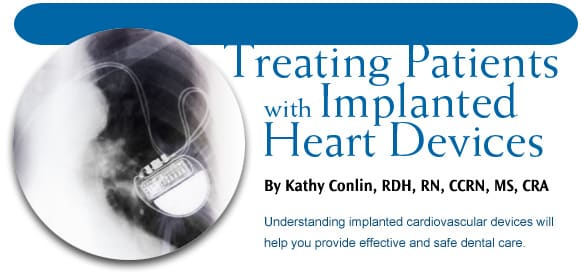
Treating Patients with Implanted Heart Devices
Understanding implanted cardiovascular devices will help you provide effective and safe dental care.
This course was published in the January 2008 issue and expires January 2011. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Discuss the challenges of correlating the medical history and providing safe, effective dental care for a patient with a surgical implantable device that treats abnormal heart rhythms.
- Explain how the different types of implantable devices manage and treat abnormal heart rhythms.
- Implement treatment plan modifications that may affect a patient with an implantable device.
- Identify methods to obtain correct information on the implantable device that treats and manages abnormal heart rhythms.
- Define electromagnetic interference and the effects on a patient with an implantable device receiving dental care.
Dental professionals are required to accurately and systematically collect, permanently record, and update the medical histories of their patients. This process is imperative to the provision of safe dental care. Every patient’s health history is unique. Health histories are becoming more involved due to the medical and technological advances in health care. If patients indicate that they have a surgically implanted device to correct heart rhythms or a device to improve the function of their heart, are you able to assess and implement accurately the dental care needed for these patients?
DEVICES AND DENTAL CARE
Understanding how the different types of implantable devices treat abnormal heart rhythms helps dental professionals implement the necessary precautions or modifications to ensure that the care delivered will not harm the patient and that emergency situations are prevented.
Pacemakers, implantable cardioverter defibrillators (ICDs), and cardiac resynchronization devices (CRTs) are complex and highly technical. They have drastically improved the quality of life for patients who are at high risk for sudden cardiac death.
In the United States alone the number of pacemakers and ICDs implanted has grown dramatically. From 1990 to 2002, 2.25 million pacemakers and 415,780 ICDs were implanted.1 The annual number of pacemakers implanted has increased almost three-fold from 94,755 in 1990 to 267,278 in 2002.1 During this same period, the annual number of ICD implants increased from 10,000 ICDs implanted in 1990 to close to 100,000 implanted in 2002.1 With the increased number of devices implanted, dental professionals must know what kind of a device their patient has and how it can directly impact the management of the patient in the dental care setting.
The type of device provides insight on how to better manage the dental care for that patient. Having one of these devices alone does not require prophylactic antibiotic premedication but the heart condition of the patient requiring the implant could dictate a need for prophylactic antibiotic coverage during certain dental procedures.
From 1997 to April 2007, the American Heart Association has recommended that patients diagnosed with hypertrophic cardiomyopathy (HCM) be premedicated prior to dental procedures.2 Cardiomyopathy is any disease that affects the heart muscle or myocardium and hypertrophic refers to the enlarged or thickened wall of the myocardium. HCM is a genetic disease that occurs in 1 out of 500 people.3 HCM most commonly causes death in those under 30 years of age by creating a fast abnormal rhythm of the ventricle, called sustained ventricular tachycardia. This heart condition requires a cardioverter defibrillator or ICD to treat the fast abnormal heart rhythm. The American Heart Association recently modified its guidelines for the prevention of infective endocarditis in May 2007. Hypertrophic cardiomyopathy no longer requires premedication for certain dental procedures.4
CARDIAC CONDITIONS
The heart conditions still associated with a high risk from infective endocarditis are the complex cyanotic congenital heart defects that can include a single ventricle, transposition of the great arteries, and/or tetralogy of fallot.5 They may require either a pacemaker to treat a slow heart rhythm or an ICD for a fast heart rhythm. These complex cyanotic congenital heart conditions still require antibiotic coverage prior to specific dental procedures per the 2007 American Heart Association Guidelines.4
Contacting the attending physician, cardiologist, or electrophysiologist (a cardiologist specializing in the electrical system of the heart) is necessary to confirm if premedication with an antibiotic is recommended for certain dental procedures. In addition, confirming if vasoconstrictors in local anesthetics (lidocaine 1:100,000 with epinephrine) need to be avoided or limited to a cardiac dose of 0.036 mg of epinephrine or two cartridges of lidocaine at 1:100,000 may also be prudent.6
For patients with prolonged QT interval disorder, all vasoconstrictors should be avoided.7 Prolonged QT interval is an inherited disorder caused by abnormalities in the ion channels of the electrical conduction system of the heart. An estimated 2,000-3,000 children and adults die each year because of this disorder. Frequently, it can be treated with medications like a beta blocker but other times devices like a pacemaker or an ICD may be required. Other medications are contraindicated because they can also prolong the QT interval in these individuals. They include over-the-counter medications, antibiotics, and fungicides. A complete list of drugs that can prolong the QT interval and cause a fast ventricular abnormal rhythm (torsade de pointes [twisting on point]) can be found at www.sads.org and www.torsade.org.
PACEMAKERS
Pacemakers have been used since the 1950s. The first pacemakers were not implanted inside the body. Only a small lead was implanted on the external surface of the heart or the epicardium. The other end was connected to an AC power unit. A definite drawback was that the patient was limited to the length of the extension cord! Power failure was also a concern, especially with a patient totally dependent on the pacemaker for his or her heart rhythm.8
Major advances have been made in the development of pacemakers. The first totally implantable pacemaker was introduced in 1960. Then came advances in pacing leads that allowed the lead to be inserted through a vein that connected to the heart instead of the earlier leads that were attached to the epicardium or the outer surface of the heart. Further advances in pacemaker technology allowed the pacemaker to pace only when necessary and to sense an intrinsic heart beat. The biggest breakthrough was the development of the lithium iodine battery in 1975. This greatly extended the pacemaker life from the AC power unit to 12 – 18 months with a mercury-zinc battery to 10 + years with the lithium battery.8
In the late 1970s, the first dual-chamber pacemaker became available. A lead was placed in the upper chamber (atrium) of the right side of the heart with another lead placed into the lower right side of the heart or right ventricle. Using two leads in the heart allowed the heart to synchronize the timing between the chambers and allowed time for the blood to flow from the upper chamber of the heart to the lower chamber of the heart, mimicking the sinoatrial node, the heart’s normal pacemaker.8
The current pacemaker is now about the size of a silver dollar. It is placed in the upper shoulder area on the nondominant side. It operates like a computer by collecting and storing data information. The computer-driven device can also adjust the heart rate to a person’s activity and, through sensing, the pacemaker can deliver the most appropriate pacing therapy for the patient.8
TABLE 1. ELECTROMAGNETIC INTERFERENCE CAN BE CAUSED BY:
- Electrical appliances in poor condition or not grounded correctly
- Electrical equipment that produces a great deal of energy, like industrial generators
- Certain devices, notably arc-welders
- Medical equipment including MRI devices, therapeutic radiation, and TENS units (pain control devices)
- Diathermy
- Electrosurgery
- Electrocautery
- External defibrillation: If the CRT/ICD device does not provide the therapy to slow the fast heart rate, the use of an automated external defibrillator is needed. The pads of the external defibrillator should not be placed on top of the device but rather 1-2 inches away from the device.
- Lithotripsy
- Radiation therapy
- Large magnets in stereo speakers
IMPLANTABLE CARDIOVERTER DEFIBRILLATOR
The implantable cardioverter defibrillator (ICD) was developed in the late 1960s. The first ICD was implanted in a patient in 1980. This device treated fast heart rates in the lower chamber of the heart, called ventricular tachycardia. It also treated ventricular fibrillation or sudden cardiac arrest. Early ICDs were quite primitive because they could only shock the heart to slow the heart rate down, had a limited battery, required open heart surgery to implant the device, and had no ability to record the data about the sudden cardiac event if a shock was needed.9
The first ICD was quite large and needed to be implanted in the abdominal area. Current ICDs are the size of a pager and can be implanted like a pacemaker. The ICD, like the pacemaker, is a computer-driven device that can store data and provide and record therapies. In addition, the ICD has pacemaker-like qualities and can provide therapy for slow and fast heart rates. The ICD treats a slow heart rate by recognizing that the heart rate is below the parameters the physician has set in the ICD. Once the ICD recognizes that the heart rate is below the acceptable range, it provides an electrical stimulus to increase the heart rate to the ranges in the ICD. In addition, the ICD can treat a fast heart rate. A pacemaker can only treat a slow heart rate. The ICD treats the fast heart rate with antitachycardia pacing. This is a painless therapy and sometimes aborts the need to shock the heart if the heart rate is too fast.9
The latest generation of implants offers CRT or cardiac resynchronization therapy. These implant devices are used for poor pump or congestive heart failure patients. They are highly advanced devices that provide 100% cardiac pacing to improve pump function along with ICD protection for fast arrhythmias related to the low ejection fraction of the heart.10
AVOIDING DANGER IN THE DENTAL OFFICE
Certain types of electrical (at certain frequencies) and magnetic energy or electromagnetic interference (EMI) can interfere with the device operation. The implantable devices are protected from interference because the circuitry is shielded inside a stainless steel or titanium case. The software provides a filtering process in the computer-driven device and has the ability to filter out some but not all electrical interference. This interference protection can be done by noise reversion function and programmable parameters.9
EMI is a concern in the dental office because newer dental equipment can operate at higher electrical frequencies and/or may have magnetic properties that can cause an interference within the pacemaker or ICD device.
Pacemakers are also tested by a magnet during routine phone checks. Patients call their pacemaker clinic and are instructed to place a magnet over the pacemaker. This magnet testing, done through a modem, indicates if the pacemaker’s battery needs to be replaced. If a replacement battery is needed, a new generator or pacemaker is implanted and the old generator or pacemaker is removed. The leads in the heart are tested and attached to the new generator.
The concern with EMI is in the ICD and CRT devices. Large magnets can deactivate them. In the hospital setting, magnets are used to deactivate the devices during surgery if certain equipment, like an electrocautery machinery, will be used during the procedure.9
These devices have improved filtering processes but can still be confused with noise. This is a greater concern because if the ICD or CRT device misinterprets the noise as a fast heart rate and the EMI continues, the device will try fast pacing to slow the heart rate down (antitachycardia pacing) and if the EMI is not terminated, the device will set up the shock therapy.9 The delivered shock is not a pleasant feeling and most patients who are conscious when they receive this therapy describe the shock as a “mule kick to the chest.” See Table 1 for the causes of EMI.
The best source of information on EMI and what can be used safely in the dental office is the manufacturer that produces the device. Each company has skilled engineers and quality assurance guidelines. Companies go through rigorous testing on their devices to provide quality preventive education for patients receiving their particular device.
When patients receive an implant, a pacemaker, ICD, or cardiac resynchronization device, they get an identification card from the manufacturer that should be placed in their wallet. This card is very helpful for the dental professional. It specifies what kind of device is implanted, what facility implanted the device, the physician who implanted the device, and how to contact the manufacturer if there are any questions regarding the device. See Table 2 for typical manufacturer recommendations for dental equipment.
Table 2. BOSTON SCIENTIFIC OFFERS THE FOLLOWING RECOMMENDATIONS FOR DENTAL DRILLS AND ULTRASONIC DENTAL EQUIPMENT:
- Vibrations produced by dental drills or ultrasonic dental equipment should not interfere with pacemaker/ICD operation. However, the EMI generated by the power source and equipment cables could potentially be detected by an implanted system. Boston Scientific has not tested for possible interactions between this type of dental equipment and Boston Scientific pacemaker/ICD systems. However, Boston Scientific has had no reported cases of interference of pacemaker/ICD systems with the use of dental drills or ultrasonic dental equipment.
Recommendation: No restrictions on use of handpiece or ultrasonic insert, but the equipment cables and power source should be kept as far away as possible from the pacemaker/ICD system.
- Dental X-rays, Apex Locators:
The use of x-ray will not affect pacemaker/ICD systems. Apex locators or root canal measuring devices also should not affect pacemaker/ICD systems.
Boston Scientific. Cardiac Myths and Facts. Available at: www.bostonscientific.com/templatedata/imports/HTML/lifebeatonline/spring2003/living.shtml. Accessed December 13, 2007.
 Another manufacturer, Medtronic, Minneapolis, Minn, has also addressed the dental environment and states: “Dental equipment and procedures such as dental drills, ultrasonic probes to clean teeth, and dental X-rays are safe from interfering with your defibrillator.”11 Medtronic also recommends that an electric toothbrush and the base charger of an ultrasonic toothbrush be kept at least 6 inches away from the device.11
Another manufacturer, Medtronic, Minneapolis, Minn, has also addressed the dental environment and states: “Dental equipment and procedures such as dental drills, ultrasonic probes to clean teeth, and dental X-rays are safe from interfering with your defibrillator.”11 Medtronic also recommends that an electric toothbrush and the base charger of an ultrasonic toothbrush be kept at least 6 inches away from the device.11
Ultrasonic units were introduced in the 1950s, long before pacemakers, ICD, and cardiac resynchronization devices were implanted. There have been no reported cases of interference. However, there may be concerns with the newer multifaceted devices that are now used in the dental environment. These devices can be used in endodontics, crown and bridge removal, and nonsurgical periodontal therapy for the removal of calculus and biofilm. They need to be validated and tested by the engineers from the device companies to assure that they do not interfere or produce EMI with the implant.
The dental professional should ask to see the patient’s pacemaker/ICD identification card, which details the type of device the patient has, the physician who implanted the device, and a toll-free number for any questions regarding the possibility of dental equipment interfering with the device. The physician who implanted the device is an excellent resource if the dental professional has any questions about the need for premedication prior to the dental appointment and/or restrictions of local anesthetics or prescribed medications.
Pacemakers, ICDs, and cardiac resynchronization therapy devices have improved the quality of life for patients at high risk for sudden cardiac death. Understanding what kind of a device a patient has can give insight on how to better provide safe dental care.
REFERENCES
- Maisel W, Moynahan M, Zuckerman B, et al. Pacemaker and ICD generator malfunctions: analysis of Food and Drug Administration annual reports. JAMA. 2006;295:1901-1906.
- Dajani A, Taubert K, Wilson W, et al. Prevention of bacterial endocarditis. Recommendations by the American Heart Association. JAMA. 1997;277:1794-1801.
- Maron B. Hypertrophic cardiomyopathy. Circ. 2006;19:2419-2421.
- Prevention of Infective Endocarditis. Available at: http://circ.ahajournals.org/cgi/reprint/CIRCULATIONAHA.106.183095. Accessed December 13, 2007.
- Deal B, Wolf G, Gelband H. Current Concepts in Diagnosis and Management of Arrhythmias in Infant and Children. 1st ed. Armonk, NY: Futura Publishing Co Inc; 1998:93-94.
- Malamed S. Handbook of Local Anesthesia. 5th ed. St Louis: Elsevier Mosby; 2004:46.
- Ahmed M, Elseed A. The medical management and dental implications of long QT syndrome. Dental Update. 2005;32(8):472-474.
- History of Pacemakers: Technology Development Through the Decades. Available at www.medtronic.com/servlet/ContentServer?pagename=Medtronic/Website/StageArticle&ConditionName=Sinus+Node+Dysfunction&Stage=Diagnosis&Article=brady_art_pacemaker_history. Accessed December 13, 2007.
- Lloyd M, Hayes D, Friedman P. Cardiac Pacing and Defibrillation: A Clinical Approach. 1st ed. Armonk, NY: Futura Publishing Co Inc; 2000:106-107.
- Cohen, T, Klein, J. Cardiac resynchronization therapy for treatment of chronic heart failure. J Invasive Cardiol. 2002;1:48-53.
- Guidelines: Medical and Dental Procedures. Available at: www.medtronic.com/servlet/ContentServer?pagename=Medtronic/Website/StageArticle&ConditionName=Sinus+Node+Dysfunction&Stage=Management&Article=brady_art_medical_and_dental. Accessed December 13, 2007.
From Dimensions of Dental Hygiene. January 2008;6(1): 14-17.



