
The Obesity-Inflammation Cycle
With obesity linked to the inflammatory process and the significant growth of obesity and overweight across the globe, dental hygienists need to understand the implications.
This course was published in the March 2009 issue and expires 3/31/12. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Discuss the role of obesity as a risk factor for systemic disease.
- Compare and contrast different methods of classification for overweight and obesity.
- Describe the advantages and limitations of using body mass index as a measure for overweight and obesity.
- Discuss how abdominal fat contributes to local and systemic inflammation.
- Describe how chronic inflammation leads to insulin resistance and metabolic syndrome.
Studies of population trends in obesity and overweight identify those who are at greater risk for associated health problems, including individuals and groups at increased risk for morbidity and mortality. Classification of overweight and obesity is a valuable tool in identifying priorities for health interventions and for evaluating the efficacy of programs aimed at controlling weight and improving health outcomes.1 The growing epidemic of childhood obesity is one of the most serious public health concerns of this century.3 The negative health outcomes associated with obesity in children become apparent later in their lives, including increased risk for diabetes and cardiovascular disease in adulthood.
The etiology of obesity is multifactorial, and includes endocrine and metabolic disorders; lifestyle behaviors, such as poor eating habits and lack of exercise; and genetic predisposition. Obesity is a risk factor for many diseases, including cardiovascular disease, type 2 diabetes mellitus, cancer, osteoarthritis, and sleep apnea.4 Obesity is also associated with reduced life expectancy and is a significant cause of preventable death.5
Body Mass Index (BMI)
|
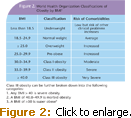
Methods to classify obesity vary in their strengths and weaknesses, but generally, obesity is defined by body mass index (BMI).6 BMI requires height and weight measures in its calculation (Figure 1).7 BMI is used to measure prevalence of obesity within a population and associated disease risks. BMI correlates strongly with fat mass and morbidity and mortality risk, and is considered the most diagnostically useful measure (Figure 2).6,8
 BMI is not a direct measure of body fat, as it is calculated using an individual’s total weight, which includes the weight of muscle mass. It does not account for body fat distribution. BMI is therefore limited as a measure for certain individuals and population groups. For example, athletes may have a high BMI due to their higher muscle mass and low percentage of body fat. At the same BMI, women will have more body fat than men, and older individuals will have more body fat than younger adults. BMI also varies by race; for Asians, BMI may be too high.1,6-10,9-12
BMI is not a direct measure of body fat, as it is calculated using an individual’s total weight, which includes the weight of muscle mass. It does not account for body fat distribution. BMI is therefore limited as a measure for certain individuals and population groups. For example, athletes may have a high BMI due to their higher muscle mass and low percentage of body fat. At the same BMI, women will have more body fat than men, and older individuals will have more body fat than younger adults. BMI also varies by race; for Asians, BMI may be too high.1,6-10,9-12
WAIST CIRCUMFERENCE AND WAIST TO HIP RATIO
Abdominal obesity is associated with significant disease risks; the degree of abdominal fat mass can vary significantly within a narrow range of BMI.1 Therefore, waist circumference (WC) also serves as a simple and accurate measure of identifying at-risk overweight and obese individuals.1,6 WC is measured using a tape measure placed around the smallest point, which is usually just above the navel. A measurement of greater than 40 inches for men or 35 inches for women is indicative of increased health risk.6,13
Waist to hip ratio (WHR) is also used to assess abdominal fat accumulation and fat distribution. A high ratio is associated with negative health consequences.13 WHR is calculated by using a tape measure to measure the waist at its smallest point and the hips at their widest point. Then, the waist measurement is divided by the hip measurement. A WHR greater than 0.9 for men and 0.85 for women indicates increased health risk (Figure 3).13
BMI, WC, and WHR are all closely correlated as assessment tools for disease risk, however, WC is unrelated to height and is a simple and more practical diagnostic screening tool to measure the quantity of abdominal fat mass.1,6,9,13,15 Other measures of body fat are available but are limited in their utility as disease predictors.6,8,15
|
|||||||||||||||
CYTOKINE PRODUCTION IN ABDOMINAL FAT
Obesity is the result of enlarged white adipose tissue, and is associated with increased local and systemic inflammation.16 Adipose tissue secretes a variety of cytokines that mediate immune and inflammatory responses throughout the body. The discovery of these chemicals and their complicated roles in mediating inflammation and disease continues to be the focus of ongoing research.
Cytokines are typically secreted by immune cells that are triggered by pathogens and endotoxins. These cells activate and recruit other immune cells in response to the antigen. Macrophages and other cells produce the immunomodulatory cytokines known as the interferons, interleukins (IL-1, IL-6), and tumor necrosis factor alpha (TNF–?). These cytokines, as well as prostaglandin E2 (PGE2), are known as pro-inflammatory mediators; even local production in a tissue may cause systemic effects or effects distant to the site of infection, as they can travel throughout the body via the circulation.17
Cytokines may exert their actions by traveling to distant parts of the body (endocrinelike effects) or by acting locally near the site of their secretion (paracrine-like effects), similar to hormones. Many of the cytokines secreted by adipose tissue act in this manner and are known as adipose-derived hormones. Adipocytes secrete cytokines known as adipokines, which are being researched for their utility as biomarkers to assess obesity related disease risks.16
Cytokines activate hepatocytes in the liver to produce acute phase proteins. Acute phase proteins possess many properties, including pro-inflammatory properties that activate, complement, and neutralize invading pathogens and stimulate tissue repair.18 IL-6 is an important inflammatory mediator that activates hepatocytes to produce acute phase proteins, such as serum amyloid P component, serum amyloid A protein, and Creactive protein (CRP).17,18 Acute phase proteins are present in both acute and chronic disease, and a large body of research is devoted to studying these proteins as biomarkers for disease risk associated with many chronic conditions, such as obesity, diabetes, and cardiovascular disease. For example, chronically elevated CRP levels and other inflammatory markers are predictive of adverse cardiovascular events and type 2 diabetes.19,20
TNF–? and IL-6 induce liver production of acute phase proteins, including CRP.21 Increased levels of TNF–?, IL-6, and CRP are associated with insulin resistance and obesity in humans.22 In animal studies, diet-induced weight gain is associated with significant increases in macrophage infiltration in adipose tissue, with increased inflammatory cytokine expression. This is the proposed mechanism by which obesity-related inflammation is thought to lead to metabolic disorders, such as insulin resistance and metabolic syndrome.16
Adipose tissue is thought to produce about 25% of systemic IL-6, and research suggests that IL-6 levels correlate more strongly to the development of insulin resistance than levels of TNF–?; TNF–? appears to act more locally than IL-6. Weight loss and low calorie diets reduce circulating levels of IL-6, but there is conflicting data about whether IL-6 actually leads to or prevents the development of insulin resistance. Confounding variables in studies examining the relationship of IL-6 to insulin resistance include age, gender, glucose tolerance, and degree of obesity. More research is needed to further define these relationships. At this time, it appears that neither TNF–? nor IL-6 used alone are appropriate biomarkers for assessing insulin resistance or metabolic syndrome.16
IL-8 is a pro-inflammatory cytokine that induces chemotaxis of white blood cells. IL-8 is produced and secreted by adipocytes, and circulating plasma levels of IL-8 are increased in obese subjects.23 Monocyte chemoattractant protein-1 (MCP-1) is an adipokine that recruits monocytes to infiltrate adipose tissue, and thus helps maintain the pro-inflammatory state that leads to insulin resistance and metabolic syndrome.24 Some studies have found increased circulating levels of MCP-1 in plasma of obese subjects. However, others suggest that this chemokine primarily acts locally causing inflammation in adipose tissue. Circulating levels of IL-8 and MCP-1 are positively correlated with BMI, WC, and level of CRP.25 The role of these cytokines as biomarkers is still under investigation.
CONCLUSION
Obesity is a significant public health concern and is a known risk factor for numerous medical conditions. The underlying pathophysiology of obesity is related to the complex interaction of immune and inflammatory processes. Chronic inflammatory processes associated with obesity are similar to those found in periodontitis. Part two of this article will explore the relationship of obesity and periodontal diseases.
Colgate is generously providing the two CE units for this course at no charge to the first 300 ONLINE TEST TAKERS ONLY (with a passing exam). To take advantage of this offer, visit the CE page and enter in the following:
|
REFERENCES
- World Health Organization. Technical report series 894. Obesity: preventing and managing the global epidemic. Available at: http://whqlibdoc.who.int/trs/WHO_TRS_894_(part1).pdf. Accessed February 12, 2009.
- James PT, Leach R, Kalamara E, et al. The worldwide obesity epidemic. Obes Res. 2001;9(Suppl 4):228S- 233S.
- Barness LA, Opitz JM, Gilbert-Barness E. Obesity: genetic, molecular, and environmental aspects. Am J Med Genet A. 2007;143A:3016-3034.
- National Heart, Lung, and Blood Institute. Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults. Available at: www.nhlbi.nih.gov/guidelines/obesity/. Accessed February 12, 2009.
- Haslam DW, James WP. Obesity. Lancet. 2005;366:1197-1209.
- Executive summary of the clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults. Arch Intern Med. 1998;158:1855-1867.
- Body Mass Index Calculator. Available at: www.cdc.gov/healthyweight/assessing/bmi/adult_bmi/index.html. Accessed February 11, 2009.
- Pischon N, Heng N, Bernimoulin JP, et al. Obesity, inflammation and periodontal disease. J Dent Res. 2007;86:400-409.
- Uwaifo GI, Arioglu E. Obesity. Available at: http://emedicine.medscape.com/article/123702-overview. Accessed February 12, 2009.
- Gallagher D, Visser M, Sepúlveda D, et al. How useful is BMI for comparison of body fatness across age, sex and ethnic groups? Am J Epidemiol. 1996;143:228–239.
- Prentice AM, Jebb SA. Beyond body mass index. Obes Rev. 2001;2:141–147.
- Mei Z, Grummer-Strawn LM, Pietrobelli A, et al. Validity of body mass index compared with other body composition screening indexes for the assessment of body fatness in children and adolescents. Am J Clin Nutr. 2002;75:978-985.
- Mayo Clinic. Waist circumference and waist to hip ratio. Available at: www.mayoclinic.com/health/waistto-hip-ratio/AN01794. Accessed February 11, 2009.
- Waist to Hip Ratio Calculator. Available at: www.bmi-calculator.net/waist-to-hip-ratio-calculator/waist-tohip-ratio-chart.php. Accessed February 11, 2009.
- Han TS, Seidell JC, Currall JE, et al. The influences of height and age on waist circumference as an index of adiposity in adults. Int J Obes Relat Metab Disord. 1997;21:83-89.
- Inadera H. The usefulness of circulating adipokine levels for the assessment of obesity-related health problems. Int J Med Sci. 2008;5:248-262.
- Loos BG. Systemic markers of inflammation in periodontitis. J Periodontol. 2005;76:2106-2115.
- Steel D, Whitehead AS. The major acute phase reactants: C-reactive protein, serum amyloid P component and serum amyloid A protein. Immunol Today. 1994;15:81-88.
- Rosenson RS, Koenig W. Utility of inflammatory markers in the management of coronary artery disease. Am J Cardiol. 2003;92:10i-18i.
- Pradhan AD, Ridker PM. Do atherosclerosis and type 2 diabetes share a common inflammatory basis? Eur Heart J. 2002;23:831-834.
- Yudkin JS, Kumari M, Humphries SE, Mohamed-Ali V. Inflammation, obesity, stress and coronary heart disease: is interleukin-6 the link? Atherosclerosis. 2000;148:209-214.
- Kern PA, Ranganathan S, Li C, et al. Adipose tissue tumor necrosis factor and interleukin-6 expression in human obesity and insulin resistance. Am J Physiol Endocrinol Metab. 2001;280:E745-E751.
- Straczkowski M, Dzienis-Straczkowska S, Stêpieñ A, et al. Plasma interleukin-8 concentrations are increased in obese subjects and related to fat mass and tumor necrosis factor-alpha system. J Clin Endocrinol Metab. 2002;87:4602-4606.
- Dahlman I, Kaaman M, Olsson T, et al. A unique role of monocyte chemoattractant protein 1 among chemokines in adipose tissue of obese subjects. J Clin Endocrinol Metab. 2005;90:5834-5840. Epub 2005 Aug 9.
- Kim CS, Park HS, Kawada T, et al. Circulating levels of MCP-1 and IL-8 are elevated in human obese subjects and associated with obesity-related parameters. Int J Obes (Lond). 2006;30:1347-1355. Epub 2006 Mar 14.
From Dimensions of Dental Hygiene. March 2009; 7(3): 24-27.



