
Symptom Management
Simple strategies to address the oral complications of the seven most common chronic medical conditions faced by older adults.
This course was published in the July 2013 issue and expires July 2016. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Identify seven chronic medical conditions that affect older adults.
- Recognize the potential oral manifestations of these medical conditions.
- Discuss strategies for addressing the dental symptoms of these chronic health problems.
The United States Census Bureau projects that between 2012 and 2060, the number of individuals age 65 and older will increase from 43.1 million to 92 million.1 Life expectancy is not the only statistic that is increasing. Older adults are also keeping their teeth longer than ever before.2 With more patients maintaining their natural teeth, there are increased risks of dental problems. In 1972, the American Dental Association estimated that older adults had 140 million teeth at risk of oral disease. This number is expected to grow to more than 900 million by 2030.2 Dental professionals must be prepared to deal with the oral health challenges present among older patients. Failure to meet the oral health needs of this population can have significant effects on their systemic health, as well as quality of life.3
As adults age, their risk for developing a chronic medical condition increases.4–6 More than half of individuals age 60 and older have an average of three chronic health problems, and seven out of 10 deaths in the US are caused by these conditions.1,7 Of the 10 most commonly prescribed medications, six are used to treat chronic conditions. This article discusses seven of these conditions, along with possible oral effects.3-14 Table 1 provides a helpful summary of these conditions’ oral symptoms, as well as applicable dental considerations, which can be kept on hand in the operatory.3–14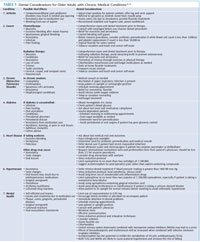
ARTHRITIS
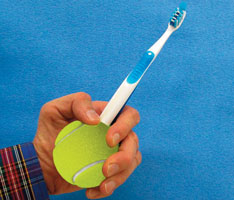
Arthritis is the most common cause of disability, affecting one in every five adults.15 Osteoarthritis, a noninflammatory degenerative disease characterized by cartilage loss and marginal bony overgrowth, is the most common form.10 Because its prevalence increases with age, almost all individuals older than 70 are affected.6 Unlike osteoarthritis, rheumatoid arthritis is an inflammatory disease, resulting in inflammation of the joints. Regardless, both osteoarthritis and rheumatoid arthritis can interfere with the ability to adequately remove bacterial plaque due to decreased dexterity.4,9 To reduce patients’ risk of developing dental disease, oral health professionals can recommend power toothbrushes or modified oral hygiene aids (Figure 1) to improve older adults’ ability to maintain sufficient oral hygiene.4,6,9
Individuals with arthritis may suffer from temporomandibular joint (TMJ) problems, such as pain, tenderness, and decreased mobility due to inflammation of the joint or structural changes in the TMJ.10 Patients can try at-home moist heat applications to decrease pain. During the dental visit, utilizing a mouth prop, keeping appointments short, and allowing frequent breaks to relax the jaw may help increase the patient’s comfort and tolerance of treatment.4,6,10
Due to a decrease in stiffness as the day progresses, scheduling afternoon appointments is preferred.4 While osteoarthritic pain affecting the TMJ often resolves within 8 months, TMJ-related symptoms may be treated with acetaminophen, aspirin, nonsteroidal anti-inflammatory drugs (NSAIDs—eg, Celebrex and Vioxx), muscle relaxants, by limiting jaw movements, physical therapy (hot and cold compresses, ultrasound, rest, controlled exercise), occlusal splints, and, ultimately, artificial joint replacement.6,10 But it should be noted that medications—such as corticosteroids, aspirin, or NSAIDs—used to treat arthritis may lead to gingival bleeding and xerostomia.10 Dental professionals should assess the patient’s risk for caries and recommend in-office and prescription fluoride applications if the risk is elevated.
CANCER
The US Centers for Disease Control and Prevention identifies cancer as the second leading cause of death, affecting more than half a million people each year.8 In 2007, 34,360 new cases of oral and pharyngeal cancer were diagnosed, causing 7,550 deaths.4 Adults older than 65 are seven times more likely to be diagnosed with oral cancer than those younger than 65.11 Patients who engage in high-risk behaviors, such as smoking and drinking, should be advised about their elevated risk, and provided with instructions for performing routine oral cancer self-examinations (Figure 2).6
Prior to undergoing any type of cancer therapy, patients should receive comprehensive exams along with any necessary preventive or restorative treatments, as well as education on optimal self-care.4,10 Extractions should be performed on teeth with poor prognosis at least 2 weeks before radiotherapy begins to reduce the risk of osteoradio necrosis.4,6 When treating patients undergoing cancer treatment, their oncologists should be consulted before any invasive dental procedure is attempted. For patients receiving chemotherapy, treating oncologists may need to be consulted to determine if any changes to the treatment plan are necessary, such as the addition of a prophylactic antibiotic before dental appointments.10
Oral effects, such as bleeding, poor healing, infections, and pain, are common among those undergoing cancer therapy.4 Mucositis (inflammation of the mucous membrane) is likely to begin 7 days to 10 days after chemotherapy is administered and is characterized by red, raw, and tender mucosa.10 Patients can minimize the risk of mucositis by drinking ice-cold water during the infusion of the chemotherapy agent, and rinsing with warm saline after the therapy is complete.4 The use of viscous lidocaine 2%, and an alcohol-free 0.12% chlorhexidine mouthrinse may also be beneficial.4
Patients undergoing radiation therapy may experience a 60% to 90% decrease in salivary output after 1 week of treatment. Chemotherapy can also interfere with salivary flow. Salivary substitutes, salivary stimulants, and fluoride therapy can support the oral health of patients experiencing xerostomia or hyposalivation.4,6,10,11 Muscle trismus, the limited ability to open the mouth due to muscle spasm, is another possible side effect of cancer therapy. It may be alleviated with the application of warm, moist heat and jaw exercises. For example, patients can place several tongue blades in their mouths three times a day for 10 minutes, while increasing the number of tongue blades used each day.4,10
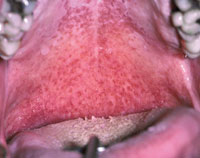
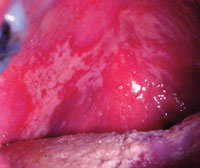
Patients undergoing cancer treatment may develop candidiasis, a fungal infection caused by yeast (Figure 3), which may require an antifungal drug.4 For those wearing dentures, the appliances can be soaked for up to 30 minutes in 1% hypochlorite to reduce the risk of fungal infection.4
CHRONIC OBSTRUCTIVE PULMONARY DISEASE
Chronic obstructive pulmonary disease (COPD), which is often caused by smoking, is a leading cause of mortality and morbidity in the United States.8,15 In 2000, more than 2 million individuals over the age of 65 were diagnosed with COPD.4 This condition results in difficulty breathing and has two common forms: chronic bronchitis and emphysema.8
Patients with a moderate to high risk of incapacity should receive a medical consultation prior to any dental treatment.4 Patients with upper respiratory infections should be rescheduled.10 It is best to treat patients with COPD in an upright or semi-upright position (due to difficulty breathing while in the supine position), and to schedule midmorning or early afternoon appointments.4,10 A low flow of oxygen (2 L/min to 3 L/min) may increase patient comfort. The use of nitrous oxide/oxygen is contraindicated in patients with severe COPD and emphysema.8,10
Because patients with COPD rely on inhalers and other medications, xerostomia and oropharyngeal candidiasis tend to be the most common oral symptoms.8 Xerostomia also raises the risk of dental caries, gingivitis, and periodontitis, and may lead to a secondary lung infection if the individual aspirates oral microorganisms. 8,12 Frequent sips of water throughout the day and the use of salivary substitutes or salivary stimulants may minimize xerostomia, while fluoride treatments and frequent recare intervals may reduce the risk of caries.4,8,10,12 Candidiasis may be treated with a prescribed antifungal medication.8 Chronic smokers with COPD may exhibit lesions such as leukoplakia (white patch), erythroplakia (red patch), and squamous cell carcinoma (varies in appearance from red patches, swelling, or ulceration), that require biopsy.10 It is the oral health professional’s responsibility to provide tobacco cessation counseling and teach patients how to perform an oral cancer self-examination.8
DIABETES
The annual incidence of type 2 diabetes among individuals older than 65 is 680 per 100,000.4 The most common dental emergency experienced by those with type 2 diabetes is hypoglycemia or low blood sugar.4,8,15 Signs of hypoglycemia include: tremors, tachycardia, altered consciousness, and a blood glucose level below 60 mg/dL.15 Hypoglycemia can be avoided by eating a meal prior to the dental appointment and complying with the prescription medication regimen.4,15 Oral health care professionals should inquire about HbA1c levels (average levels of blood glucose over the past 3 months) and measure the patient’s blood glucose before treatment.4,10 HbA1c levels less than 7% indicate that the patient’s diabetes is controlled.10,15 Ideally, blood glucose levels should be less than 120 mg/dL if fasting and less than 150 mg/dL 2 hours after eating.15 Elective dental treatment should be deferred if a patient’s fasting blood glucose is greater than 200 mg/dL.10 If a patient has taken his or her medication, but has not had an appropriate meal, the oral health care professional may dispense oral glucose prior to the dental procedure.4
Individuals with uncontrolled diabetes may be immunocompromised and present with various oral conditions, including infection; poor healing; oral ulcerations; candidiasis; periodontal abscesses; periodontal diseases; medication-induced xerostomia; numbness, burning, or pain in oral tissues; aphthous stomatitis; and lichen planus.4,6,8,10
Periodontal and oral surgery should be avoided in patients with poor glycemic control.10 Patients taking high doses of insulin that present with oral infections may require antibiotic prophylaxis, if indicated by their physicians.8 The best time to schedule a patient with diabetes is in the morning or mid-morning. 10 Research has demonstrated that uncontrolled diabetes affects periodontal health and the presence of periodontal diseases affects diabetic control. As such, dental hygienists should use these findings to motivate patients with uncontrolled diabetes to establish and maintain optimal oral health.8
HEART DISEASE
Ischemic heart disease (hardening of the arteries) is a leading cause of death among 70% of individuals 75 and older.4,5,14 Oral health care professionals can prevent and manage medical emergencies related to heart disease by maintaining their cardiopulmonary resuscitation training, developing and rehearsing a dental office medical emergency protocol, keeping emergency kits readily available, carefully reviewing each patient’s medical history, and providing profound anesthesia and conscious sedation.4,5,7,10 During the medical history update, clinicians should ensure medication compliance and inquire about the patient’s last medical visit and outcomes.4 Recent international normalized level should be obtained for patients on warfarin, in addition to careful consideration of drug interactions.4,5,10 If a patient’s medical history indicates a heart attack experienced within the past 6 months, routine dental care should be postponed due to the instability of the myocardium.5
Patients with histories of angina should place their nitroglycerine in an accessible location during the dental appointment. Those with frequent episodes of angina require medical consultation and are usually managed with a prophylactic dose of 0.3 mg to 0.6 mg of nitroglycerin.4,5,7 Patients with unstable angina or recent hospitalization related to myocardial infarction, angioplasty, or stent placement should receive medical consultations prior to treatment.4
Because dental visits can increase stress levels and, consequently, blood pressure, clinicians should monitor vitals, use a stress-reduction protocol, and limit the use of epinephrine to 0.036 mg or two carpules of local anesthesia with 1:100,000 epinephrine, while ensuring a negative aspiration.4,10 Magnetostrictive ultrasonic scaling and electrosurgery should be avoided if the patient has a unipolar pacemaker or defibrillator.10 Patients with heart disease do best with short morning appointments.5 Before dismissal, patients should be allowed to sit upright for several minutes prior to standing to avoid orthostatic hypotension (a sudden decrease in blood pressure upon standing).4,5 For post-operative pain relief, acetaminophen should be recommended instead of aspirin to minimize gingival bleeding.5,10
HYPERTENSION
Elevated blood pressure or prehypertension occurs when the systolic reading is 120 mm Hg to 139 mm Hg and the diastolic reading is between 80 mm Hg and 89 mm Hg. Hypertension exists when blood pressure exceeds 140/90 mm Hg.7 Studies indicate that approximately 30% (67 million) of adults have hypertension, with 36 million experiencing uncontrolled hypertension and 15 million unaware of their condition.7 Many of the same recommendations made for patients with heart disease also apply to patients diagnosed with hypertension. Patients with repeatedly high blood pressure readings should consult with their physicians before receiving dental treatment.4 Patients presenting with blood pressure exceeding 180/100 mm Hg should not receive elective dental care.10 Numerous medications used to control hypertension may cause xerostomia and other side effects, which should be addressed by the patient’s oral health care professional.4,10,12 Additionally, drug interactions should be carefully considered. To decrease stress and anxiety, some patients may benefit from the use of local anesthesia and nitrous oxide during treatment.7
MENTAL HEALTH CONDITIONS
Approximately 7% of people older than 65 and 40% of those 85 and older experience dementia or loss of cognitive ability.4,10 The most common form of dementia is Alzheimer’s disease, a progressive neurodegenerative disorder characterized by impaired memory, comprehension, judgment, and orientation to time, people, and places; reduced attention span; and the inability to think abstractly.4,13,16 To effectively treat patients with dementia, oral health professionals must demonstrate patience and compassion.
While there is no cure for Alzheimer’s disease or dementia, treatment almost always includes the use of prescription medications. 4,13,16 Dental professionals should be familiar with the possible drug interactions to avoid any complications. Clinicians must obtain informed consent from the patient’s legal guardian before treatment is provided, and explicit self-care instructions should be given to the caregiver. Additionally, the guardian should be present during the dental procedure to alleviate stress and anxiety.4,13 Dental problems should be addressed quickly, as patients diagnosed with dementia may become less cooperative as the disease progresses.4,16 While profound anesthesia will ensure patient comfort, the use of vasoconstrictors should be limited to 0.05 mg (equivalent to three cartridges of 1:100,00 epinephrine).13It is best to schedule short (45 minutes) morning appointments to ensure patient cooperation.4,13 Patients with dementia should be treated in the semi-upright position to avoid complications such as aspiration and postural hypotension.4
Some cognitively impaired older adults have difficulty communicating the fact that they are in pain during dental treatment, and may resort to negative behaviors, such as chewing the lip, tongue, or hands; acting aggressively; or screaming.16 Dental considerations include: consulting with the patients’ physicians regarding the disease stage and prognosis, minimizing noise, breaking down tasks into simple elements, explaining all procedures, repeating information, reassuring patient safety, avoiding excessive stimulation, using short sentences, providing direct eye contact, and gently touching the patient.13 In some cases, the patient’s disorder may be uncontrolled, and the dental appointment should be postponed.4,10 Given the patient’s tendency to forget, all instructions should be expressed both verbally and in writing.4 Patients presenting with oral side effects may benefit from the addition of chlorhexidine and home-based fluoride application.10
CONCLUSION
The incidence of chronic medical conditions that can exert significant oral side effects is high among older adults, and will continue to grow as the US experiences an increase in this demographic. Many older adults struggle to maintain their oral health, so dental professionals need to support this patient population with strategies—ranging from self-care education to shortened appointment times—in order to support both systemic and oral health.
ACKNOWLEDGMENT
FIGURE 2 AND FIGURE 3 ARE COURTESY OF LAWRENCE W. BLANK, DDS, ROCKVILLE, MD.
REFERENCES
- United States Census Bureau. 2012 NationalPopulation Projections. Available at:www.census.gov/population/projections/data/national/2012.html. Accessed June 10, 2013.
- American Dental Association. NationalCoalition Consensus Conference on Oral Health of Vulnerable Older Adults and Persons with Disabilities. Available at:www.ada.org/sections/newsAndEvents/pdfs/2010_nccc_proceedings.pdf. Accessed June 10, 2013
- Chalmers J, Johnson V, Tang JH, Titler MG.Evidence-based protocol: oral hygiene care for functionally dependent and cognitively impairedolder adults. J Gerontol Nurs. 2004;30:5–12.
- Scully C, Ettinger RL. The influence of systemic diseases on oral health in older adults. J Am DentAssoc. 2007;138(Suppl):7S–14S.
- Rose LF, Mealey B, Minsk L, Cohen W. Oral care for patients with cardiovascular diseases and stroke. J Am Dent Assoc.2002;133(Suppl):37S–44S.
- DeBiase CB, Austin SL. Oral health and older adults. J Dent Hyg. 2003;77:125–145.
- Grover S, Rhodus NL. Common medical conditions in elderly dental patients. Part one:cardiovascular implications and management. Northwest Dent. 2012;91(5):29–35.
- Grover S, Rhodus NL. Common medical conditions in elderly dental patients. Part two:diabetes, stroke, and breathing problems.Northwest Dent. 2012;91(6):29–35.
- Kelsey JL, Lamster IB. Influence of musculoskeletal conditions on oral health among older adults. Am J Public Health. 2008;98:1177–1183.
- Little JW, Falace DA, Miller CS, Rhodus NL.Dental Management of the Medically Compromised Patient. 8th ed. St. Louis: Elsevier; 2012.
- Vargas CM. Kramarow EA, Yellowitz JA. The oral health of older Americans. Aging Trends.2001;3:1–8.
- Turner MD, Ship JA. Dry mouth and its effects on the oral health of elderly people. J Am DentAssoc. 2007;138:15S–20S.
- Friedlander AH, Norman DC, Mahler ME,Norma KM, Yagiela JA. Alzheimer’s disease psychopathology, medical management, and dental implications. J Am Dent Assoc. 2006;137:1240-1251.
- United States Center for Disease Control andPrevention. Chronic disease prevention and health promotion. Available at: www.cdc.gov/ chronicdisease/ resources/publications/aag.htm. Accessed on June 10, 2013.
- Kidambi S, Patel SB. Diabetes mellitus:considerations for dentistry. J Am Dent Assoc.2008;139(Suppl):8S–18S.
- Chalmers J, Pearson A. Oral hygiene care for residents with dementia: a literature review. J Adv Nurs. 2005;52:410–419.
From Dimensions of Dental Hygiene. July 2013; 11(7): 59–63.



