
Keeping Your Hands Healthy
Dimensions of Dental Hygiene talks with John Molinari, PhD, about hand dermatitis reactions.
Q. What is the most common cause of contact dermatitis?
A. The most influential factor in contact dermatitis is dental professionals not caring for their hands properly. After repeated exposure to soaps and chemicals, clinicians often don’t follow the steps needed to protect their hands. For example, when soap is not rinsed off the hands and then the gloves go on, the hands perspire, reactivating the soap left on the hands, causing irritation. A reddened area can develop with itching. This irritation eventually breaks down epithelium, thereby initiating dermatitis. This is a nonspecific dermatitis caused by contact with substances that physically or chemically break down or damage the skin. This nonimmunological adverse reaction is the most common form of observed hand dermatitis (Figure 1).

Figure 1. Nonspecific irritation dermatitis on the hand of a dental hygienist who washed hands frequently and did not use a water-based lotion to keep her hands from becoming dry and chapped.
Q. What are the symptoms of this type of dermatitis?
A. The hands become reddened, dried, cracked, and they may even bleed in severe incidences. After washing hands 25 to 30 times a day, they can become dry. This occurs when moisture is not replaced with a water-based type of emollient, when the hands are not dried properly, and/or when soap residue is left. When the hand wash agent is not properly rinsed from an existing site of irritation, the wounded area holds the soap more tenaciously. Thus, an important component of hand washing requires that any area of dermatitis be rinsed even better than the rest of the hand.
Q. Are hives or small raised bumps a symptom of contact dermatitis?
A. No, hives are due to a type I hypersensitivity, which is a true adverse immunological reaction. This form of immediate allergic reaction is an IgE (reaginic)-based response, which means visible manifestations occur in response to specific antibodies and released pharmacological mediators, ie, histamine, serotonin, prostaglandins, slow reacting substance–anaphylaxis. A variety of substances can induce this type of reaction, ranging from house dust to foods to chemicals. The IgE-mediated allergic reaction can produce a wheal and flare skin lesion (hives), which usually develops within a few minutes after challenge exposure to the allergen. This is also one of the harmful allergic reactions that can develop against certain natural rubber latex (NRL) proteins. For example, you may wear latex gloves for 20 years and one day your body tolerance to the allergens disappears. You subsequently become sensitized to the allergenic proteins in the latex liquid. Clinical symptoms can then develop with the next and subsequent challenge exposures. A more severe manifestation of type I hypersensitivity can develop in certain people who are allergic to airborne allergens. Allergic challenges via respiratory or conjunctival tissues to NRL or other allergens can lead to more systemic anaphylactic symptoms, such as coughing, wheezing, shortness of breath, and/or respiratory distress.
Q. What is contact dermatitis and can this type of reaction affect dental hygienists?
A. Along with the aforementioned nonspecific and type I allergic reactions,contact dermatitis in the form of a type IV or delayed hypersensitivity reaction can occur. >This is different from the type I immune reaction in that it does not involve antibodies, but rather sensitized lymphocytes. The type IV hypersensitivity involves CD 4+ T-lymphocytes and, as a result, clinical symptoms take longer to manifest. This abnormal cellular immune response is typically localized and observed as a delayed contact dermatitis. The visible reaction is delayed since lymphocytes and other inflammatory cells must migrate to the area where the inciting chemical or other allergen is located. Thus, the reaction can take 12 to 24 hours or longer to become observable. The slow forming, well-demarcated lesion is the result of chronic inflammation into the affected area. A common example of contact dermatitis is seen with people who suffer from a poison ivy allergy. The allergenic poison ivy oil, called urishiol, is found primarily on the leaves. A person may be initially sensitized when he or she touches the plant’s leaves. Following a subsequent challenge of the now allergic person, sensitized lymphocytes and other chronic inflammatory lymphoid cells migrate to where the allergenic chemical is found on surface epithelial cells, walling off the whole area. This reaction causes necrosis and scabbing, which lasts for about 4 days.
Q. What is the duration of the type I lesion?
A. In contrast to the delayed type IV contact dermatitis, type I allergic reactions have a much shorter duration, approximately 20-30 minutes. In some instances, the response can take up to an hour if it is a slow reacting type I hypersensitivity. This is a primary reason why type 1 reactions are called immediate hypersensitivities (Figure 2) and the others (type IV) are called delayed.
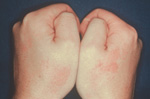
Figure 2. Example of type I cutaneous anaphylactic hypersensitivity. Immediate, type I allergic reaction to latex gloves worn by a dental assistant. Itching and reddening of the hands began with a few minutes after the sensitized person was challenged with latex allergens. After she immediately removed the gloves, the symptoms subsided over the next 30-45 minutes.
Q. Where Does Latex Come From?
A. Latex comes the secretions of plants, mostly rubber trees. The sap from tropical trees are collected periodically during the year and water soluble proteins come out in the sap. The sap is collected, treated, and more than 200 chemicals are added. The substance is then heated in order to increased its strength and elasticity. Latex gloves are rinsed extensively after the heating process to remove the water-soluble proteins and as much of the water-soluble chemicals but not all are removed.
Q. What are the most common irritants that cause contact dermatitis?
A. Metal and jewelry are common allergens. Many people become allergic to their watches or other metal jewelry as the bands often contain nickel (Figure 3). Regarding the latex allergy example, as a result of better qualitative and quantitative information, manufacturers are now required by law to better purify their latex products. This includes using additional water-rinse procedures in order to remove water-soluble latex proteins and water-soluble chemicals. All manufacturers are required to adhere to the applicable Food and Drug Administration regulations that went into effect in the fall of 1997.

Figure 3. Example of type IV hypersensitivity illustrating an allergic reaction to nickel in a metal watchband worn by a dental hygienist. Note the well-demarcated induration and localization of the chronic inflammatory reaction. This harmful response healed with scabbing and epithelial sloughing within 96 hours.
Q. How do we protect ourselves from latex exposure?
A. Gloves and rubber dams are not the only products that contain latex. Items like balloons, the soles of shoes, the rubber backing of carpeting, and underwear with elastic all contain latex. Thus, the potential for latex exposure has increased dramatically. Becoming better consumers is key so you know what products contain latex in the operatory. Latex-free alternatives also exist, including vinyl, nitrile, and other semisynthetic gloves. The new generation of latex-free gloves fit better, are sturdier, have more flexibility, and are less irritating than nonlatex gloves in the past. Also, there are now latex-free rubber dams, prophylaxis cups, and a variety of other disposable items. Even in an office without latex allergic staff, multiple products are available that further reduce the potential for these harmful reactions. The keys to protection are first preventing development of hypersensitivity reactions where possible and then correctly diagnosing the type I or type IV allergies when they occur. Most people immediately assume they have a latex allergy when, in fact, it could be irritation dermatitis that can be corrected just by taking care of the hands. In cases where a hypersensitivity is possible, an allergist or dermatologist should be consulted to make the final diagnosis.
Q. What is the most effective treatment for an allergic reaction?
A. Basically, antihistamines are used to treat most common cutaneous type 1 reactions (hives), since it is the histamine release from mast cells and basophils that causes many of the symptoms of edema, runny nose, and the itchy eyes. In life threatening situations (after calling 911), epinephrine is used to assist a person who is having a systemic anaphylaxis episode. For type IV reactions, the standard treatment is topical corticosteroids because they are anti-inflammatory. A topical antihistamine can also be used to reduce itching.
Q. Are the waterless disinfecting soaps effective?
A. They work if the hands are not dirty, meaning contaminated with body fluids such as saliva, blood, or exudate. The 2003 Centers for Disease Control and Prevention Guidelines for infection control in dentistry note that when hands are not visibly soiled, the waterless hand hygiene agents are useful and effective as alternatives to traditional hand washing with liquid soaps or antiseptics. If hands are visibly soiled, then only soap and water or antiseptic hand washes with soap and water should be used. The use of waterless hand hygiene agents has been shown to be effective in a number of health professional settings in part because they have fostered an increase in hand washing compliance. However, a note of caution is necessary. If a person has dry skin, these agents may exacerbate the problem. Many of the newer products contain emollients like glycerin and aloe vera, which help moisturize the epithelium and reduce dryness and cracking.
Q. Does the addition of aloe in gloves help?
A. I believe that aloe is effective for lubrication. It also may help in the irritation dermatitis both in comfort and in healing.
Q. Are there any preventive therapies on the horizon?
A. Allergy shots are not given for latex sensitivity or contact dermatitis so basically creating new products and, in the case of latex, more nonlatex products as a substitute are the current options.
From Dimensions of Dental Hygiene. April 2005;3(4):16, 18, 20.

