
Improving Access to Care
The dental prevention coordinator can make a big difference in the oral health of vulnerable populations.
Access to quality oral healthcare is a concern for many in the United States. In the past, initiatives, such as the American Dental Association’s community dental health coordinator (CDHC), were designed to facilitate dental treatment by connecting underserved groups with accessible dental care.1 However, this initiative left out one of the most underserved groups: adolescents and adults with special needs. As adults with mentally and physically compromising conditions are living longer, their dental needs have grown proportionately. Skilled, knowledgeable dental team members who can listen, assess, and provide treatment are critical to ensuring patients with special needs receive comprehensive care. To address this need, a pilot program was established at the Henderson Dental Center at St. Joseph Mercy Oakland in Pontiac, Michigan, that introduced a new member to the oral healthcare team—the dental prevention coordinator (DPC).1 A dental hygienist was the logical choice for this position, as this team member would meet the patient before treatment, participate in care, and follow-up after treatment—in whatever setting was required.

Community and Clinical Settings
Much like the CDHC and visiting nurse model, the DPC would first meet the patient in the community setting. Patients residing in a group home were initially chosen, as these facilities are licensed by the state. After the DPC received training in state group home procedures, protocols, and requirements, the local mental health agency began referring group home residents in need of dental care.
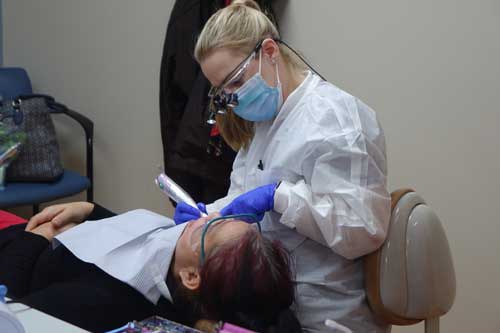
After obtaining necessary consents, the DPC would visit the patient at the group home. This visit occurred at dinnertime so the DPC could view the patient’s social interactions, examine dietary preferences or restrictions, and observe eating and chewing. As all medical records were available at the home, there was ample opportunity to review complex medical records, and plan questions or medical consultations. Finally, after dinner, the DPC would observe dental hygiene practices in order to better understand the patient’s capabilities, toothbrushes and dental aids used, and degree of staff involvement (Figure 1). Meeting the staff responsible for nighttime hygiene practices would be important to the success of dental treatment.
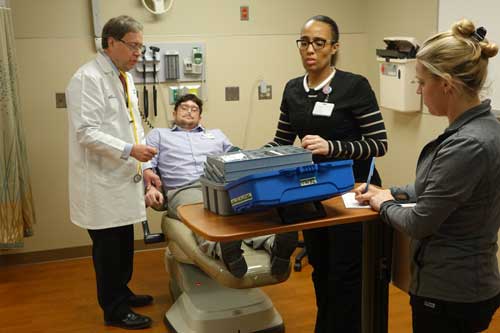
The information gathered by the DPC is invaluable in scheduling the patient’s first dental visit in the clinic or a hospital setting. Due to personal familiarity, the DPC initially greets the patient at the facility. This is key because seeing someone who has actually been to the group home makes it much easier for patients with special needs to adjust. At this appointment, an examination is attempted and the clinical findings documented (as behavior will allow). Based on the home assessment by the DPC, as well as the patient’s observed needs and behavior, a decision is made by the dentist on where care will be delivered. For the cooperative patient, this may begin with periodontal treatment in the dental clinic, with no alteration in how care is delivered. For the patient with extensive needs and/or little cooperation, care may take place in the hospital operating room under general anesthesia.

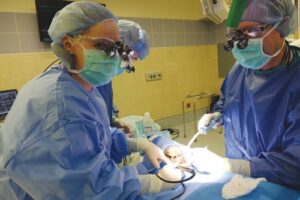
When care will be delivered in the operating room, the DPC initiates the necessary consent forms and medical coordination to schedule the case. On the day of the procedure, the DPC serves on the clinical team treating the patient (Figure 2). Almost all of the patients treated need periodontal therapy, thus, the clinical hygiene skills of the DPC heighten the importance of this dental team member. This is also an opportunity for the DPC to view all areas of the oral cavity in order to gain a thorough understanding of the patient’s oral condition. Once periodontal treatment is completed, the dentist and dental residents perform the restorative and surgical procedures deemed necessary.
Educator Role
Following completion of periodontal treatment, the DPC leaves the operating room to meet the patient’s caregivers. After reassuring them of the safety and progress of the case, the DPC can begin the educational process. In addition, the DPC can review precautions and restrictions following general anesthesia and dental treatment. Once all of the calculus and plaque are removed, hopeless teeth extracted, and teeth restored, the patient is ready to start on a new path toward oral health. Most importantly, the DPC and other team members can advocate to improve patients’ at-home oral hygiene in order to maintain the new level of oral health following initial care. Having visited the group home and observing the patient’s oral hygiene practices, the DPC can realistically suggest techniques and routines to support improved oral health.

This level of support continues with a home visit 2 days to 3 days after the procedure. At this time, the DPC can answer questions about recovery from general anesthesia and begin to support at-home hygiene efforts with the group home staff. All too often, the staff is hesitant to provide oral hygiene support because they do not want to “hurt” or “disturb” anything; this is usually not the right approach. Again, this presents an opportunity for the DPC to provide caregiver education. These steps are key, because the immediate period following definitive treatment is the time to clean healing tissues and implement post-operative instructions given at the hospital or clinic. The DPC is present to review these instructions and coach the staff on necessary at-home care. When the patient is seen back in the hospital or clinic 2 weeks to 3 weeks after the procedure, the continuity of the DPC once again plays a significant role in coordinating the group effort to help the patient attain optimal oral health.
There are many benefits to employing a skilled dental hygienist in the role of DPC. As with any type of community outreach, it first requires someone who is comfortable meeting new people. As many of the patients have complex medical histories, the DPC must determine the relevant facts on history, medical status, and medication usage. Frequently, the primary care physician does not have a thorough understanding of the patient’s oral health needs, nor the dental implications of prescribed therapies.
Due to the in-depth, coordinated approach led by the DPC, medical management is sometimes adjusted and improved by the dental team’s involvement. This can help prevent complications in cases involving oral care under general anesthesia. Additionally, this approach can yield improved systemic health. Just as dental care is often an unmet need, these patients may have unmet medical needs, as well. For example, while reviewing the medical history, the DPC might find that a pelvic exam is warranted for female patients. Coordinating testing and other treatment at the same time dental care is delivered leads to more comprehensive care in a safe and cost-effective manner.

Quite often, patients who are nonverbal cannot communicate the oral pain they may be experiencing. The pain may result in behaviors that are atypical, yet medical providers and caregivers do not consider a dental etiology for the behavior. In the past, delayed diagnosis of dental problems has led to emergency extraction of teeth and further oral health issues. Here again, the DPC’s relationship with caregivers in the group home helps provide support and education for the home staff—and, ultimately, true preventive and maintenance care for the patient.
Based on our experience with the DPC model at St. Joseph Mercy Oakland, once a patient’s acute dental problems are resolved, it often becomes easier to perform periodontal maintenance procedures in the clinic, with no special accommodations. This can result in a more comfortable, maintainable level of oral health that can be supported in the future. Thus, having a dental team member who is focused on treatment and prevention helps support the oral and systemic health of this patient population.
As this pilot program demonstrates, utilizing the training of a dental hygienist allows for expansive opportunities to help educate and make the community aware of the oral healthcare needs of these patients. Whether it involved answering questions regarding adults with special needs, or serving as a resource to the county mental health agency, the dental knowledge of the DPC proved essential.
Summary
Educating dental and dental hygiene organizations helps everyone in the profession reassess how we can improve treatment for those with special needs. Assessment of the DPC pilot program demonstrates this new team member can facilitate respectful, comprehensive care in the least restrictive setting. Where a patient with special needs may have been uncooperative to begin with, an ongoing relationship with a skilled provider can allow for a better dental experience. Ultimately, the continuity and coordination of care provided by a DPC seeing patients in a group home supports greater cooperation, more frequent visits, and improved oral and systemic health for this population.
Acknowledgment: The authors wish to thank Stephanie Demoss, RDH, BS, the first dental prevention coordinator, and the Jewish Fund of Metropolitan Detroit for its financial support.

Reference
- American Dental Education Association. Temple University to Serve as Site for New ADA Pilot Program to Help Serve Area Communities. Available at: adea.org/ADEA/Blogs/Bulletin_of_Dental_Education/Temple_ University_to_Serve_as_Site_for_New_ADA_Pilot_Program_to_Help_Serve_Area_Communities.html#:~:text=Kornberg%20School%20of%20Dentistry%2C%20Temple,limited%20access%20to%20dental%20care. Accessed March 17, 2022.
From Dimensions of Dental Hygiene. April 2022;20(4):14-15.

