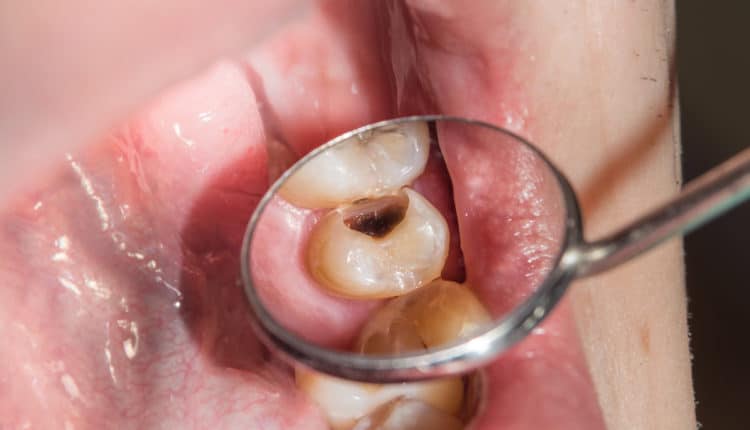
Using CTV to Reduce Root Caries Risk
The use of 1% chlorhexidine in 1% thymol varnish may help elderly patients with poor oral hygiene decrease their risk of decay.
I provide oral health services to older adults living in an assisted living facility. Most of my patients struggle with regular oral hygiene and they are at high risk for root caries. Would the addition of chlorhexidine/thymol varnish be a helpful adjunct to help prevent decay?
To date, most of the research on 1% chlorhexidine in 1% thymol varnish (CTV) has been conducted on children, examining levels of mutans streptococcus (MS) and lactobacillus in saliva, and levels of MS in fissures in both primary and permanent teeth following varnish placement.1–4 The premise for using CTV is that chlorhexidine produces antibacterial effects, including selective effects against MS. Theoretically, if MS levels can be reduced, caries risk should also decrease. Short-term reductions of MS and lactobacillus have been reported, with little differences shown after 3 months to 6 months as compared to placebo. Most studies have not been of sufficient duration to show long-term effects on caries incidence.
Investigators in a double-blind clinical trial randomly assigned 102 frail elderly patients to receive either CTV or a placebo varnish. All leathery and soft root lesions were first coated with a fluoride varnish, then the CTV or placebo varnish was applied to the lesions. Patients received their assigned varnish treatment five times over the course of 1 year. At the end of the study, the size and severity of root lesions did not change in patients who received CTV; however, lesions treated with the placebo varnish worsened (eg, increased length, width, and extended closer to the gingival margin). Following CTV application, there was an initial significant reduction in levels of salivary MS; however, at 12 months, there were no differences in salivary MS levels between the two varnish groups. These findings suggest that use of CTV may help to reduce lesion progression, but that antibacterial effects produced by CTV varnish are short-lived.5
Baca et al6 conducted a randomized controlled clinical trial to examine whether the use of CTV slows the progression of root caries, and whether its use reduces the overall incidence of new root caries formation. Dentate institutionalized elderly (n=68) were randomly assigned to receive application of CTV or placebo varnish twice in 1 week, then again at 1 month, and then every 3 months. Results revealed that the progression of root lesions was significantly less for those who received CTV as compared to application of a placebo varnish. At 1 year, the rate of new root caries was also significantly lower in those who received CTV. Investigators concluded that CTV may help to control progression of established root carious lesions and reduce incidence of root caries in an institutionalized population as a complement to usual oral hygiene practices.6
Chlorhexidine is the gold standard antibacterial agent against which other agents are compared for the reduction of supragingival plaque and gingivitis. Thus, investigators have hypothesized that application of CTV could also reduce plaque and gingivitis, especially among older adults with poor oral hygiene. However, a study of 56 institutionalized elderly, ages 64 and older, who were randomly assigned to receive CTV or placebo varnish, twice in the first week, then again at 1 month, 3 months, and 6 months, found no differences in either plaque or gingival index scores with either varnish.7 Use of CTV did not reduce plaque or gingivitis in this elderly population with poor oral hygiene.
Oral health professionals who choose to apply CTV and other varnishes likely do so at routine preventive care visits. In the previously discussed studies, patients received the varnishes at baseline, and then again repeatedly over the course of 3 months to 6 months, but without a change in patients’ usual oral hygiene habits. It is unknown what role oral hygiene status has on influencing efficacy of this treatment.
A recent systematic review found that there is no conclusive evidence that the application of CTV is effective when regular professional oral prophylaxis is performed. Higher concentrations of chlorhexidine varnish (40%) were found to provide a greater benefit over control or fluoride varnishes. Lower concentration chlorhexidine varnishes (1% and 10%) may be beneficial for high-risk patients, such as older adults, to help protect against root caries when oral hygiene is poor and in the absence of regular professional oral prophylaxis.8
In October 2018, the American Dental Association (ADA) issued revised evidence-based guidelines for the nonrestorative treatment of carious lesions.9 According to the latest ADA recommendation: “to arrest or reverse noncavitated and cavitated carious lesions on root surfaces of permanent teeth, the expert panel suggests clinicians prioritize the use of 5,000 ppm fluoride (1.1% NaF) toothpaste or gel (at least once per day) over 5% NaF varnish (application every 3 months to 6 months), 38% silver diamine fluoride (SDF) plus potassium iodide solution (annual application), 38% SDF solution (annual application), or 1% chlorhexidine plus 1% thymol varnish (application every 3 months to 6 months).”9 Clinicians are referred to the ADA Center for Evidence-Based Dentistry to read the full report with related recommendations at: ebd.ada.org.
REFERENCES
- Ben Khadra GM, Arrag EA, Alammori M, AlKadi MF. The effect of chlorhexidine-thymol and fluoride varnishes on the levels of Streptococcus mutans in saliva in children aged 6–8 years. Indian J Dent Res. 2019;30:67–72.
- Lipták L, Bársony N, Twetman S, Madléna M. The effect of a chlorhexidine-fluoride varnish on mutans streptococci counts and laser fluorescence readings in occlusal fissures of permanent teeth: a split-mouth study. Quintessence Int. 2016;47:767–73.
- Flamee S, Gizani S, Caroni C, Papagiannoulis L, Twetman S. Effect of a chlorhexidine/thymol and a fluoride varnish on caries development in erupting permanent molars: a comparative study. Eur Arch Paediatr Dent. 2015;16:449–454.
- Sajjan PG, Nagesh L, Sajjanar M, Reddy SK, Venktesh UG. Comparative evaluation of chlorhexidine varnish and fluoride varnish on plaque Streptococcus mutans count-—an in vivo study. Int J Dent Hyg. 2013;11:191–197.
- Brailsford SR, Fiske J, Gilbert S, Clark D, Beighton D. The effects of the combination of chlorhexidine/thymol- and fluoride-containing varnishes on the severity of root caries lesions in frail institutionalised elderly people. J Dent. 2002;30:319–324.
- Baca P, Clavero J, Baca AP, González-Rodríguez MP, Bravo M, Valderrama MJ. Effect of chlorhexidine-thymol varnish on root caries in a geriatric population: a randomized double-blind clinical trial. J Dent. 2009;37:679–685.
- Clavero J, Baca P, Paloma González M, Valderrama MJ. Efficacy of chlorhexidine-thymol varnish (Cervitec) against plaque accumulation and gingival inflammation in a geriatric population. Gerodontology. 2006;23:43–47.
- Slot DE, Vaandrager NC, Van Loveren C, Van Palenstein Helderman WH, Van der Weijden GA. The effect of chlorhexidine varnish on root caries: a systematic review. Caries Res. 2011;45:162–173.
- Slayton RL, Urquhart O, Araujo MWB, et al. Evidence-based clinical practice guideline on nonrestorative treatments for carious lesions: a report from the American Dental Association. J Am Dental Assoc. 2018;149:837–849.
From Dimensions of Dental Hygiene. July/August 2019;17(7):16,18.

