Caring for Patients With Down Syndrome
Individuals with Down syndrome, or trisomy 21, have specific oral health considerations that clinicians should be prepared to address.
This course was published in the June 2021 issue and expires June 2024. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Identify the incidence and common clinical characteristics of Down syndrome (DS) or trisomy 21.
- Describe oral health considerations and treatment approaches applicable to this patient population.
- Discuss considerations for comorbidities in patients with DS, and the importance of a collaborative, multidisciplinary approach to care.
Down syndrome (DS), or trisomy 21, is a condition in which a person has a full or partial extra copy of chromosome 21. It is considered the most common chromosomal disorder.1,2 The United States Centers for Disease Control and Prevention reports that nearly one in 700 babies in the US is born with DS.1–3 This population is characterized by individuals with different abilities and intellectual capacities. In addition, these patients often have increased risk for medical and oral health conditions. Dental professionals have an opportunity to improve oral health outcomes and quality of life for patients with DS. With that goal, this paper will provide an overview of DS, including etiology, risk factors, comorbidities, and oral health considerations.
Among this patient population, DS is caused by full trisomy 21 in the majority of cases (94%), translocations (3.3%) and mosaicism (2.4%). Most of the translocations are de novo, while approximately 25% result from familial translocation.4 Full trisomy 21 occurs from nondisjunction during meiosis in one of the parents, with the most common occurrence associated with an error in maternal meiotic division (meiosis I error). This error occurs three times as frequently as maternal meiosis II errors. The remaining cases are associated with paternal origin.4,5
Risk factors include advanced maternal age and altered recombination patterns during meiosis.4–7 More recently, a significant association between low maternal socioeconomic status and meiosis II chromosome 21 nondisjunction was found in an epidemiological study of DS cases compared to control families. Further study is needed to determine if other risk factors, such as environmental exposures and poor nutrition, may affect this genetic outcome.8
CLINICAL CHARACTERISTICS AND COMORBIDITIES
Individuals with DS have common physical features and craniofacial characteristics. General physical features may include shortened extremities; short, broad hands; small fifth fingers that sometimes curve toward the thumb; single transverse palmar creases; joint hyperflexibility; neuromuscular hypotonia; diastasis recti; dry skin; premature aging; and congenital heart defects. Craniofacial features may include flat occiput; flattened facial appearance; small brachycephalic head; epicanthal folds; flat nasal bridge; Brushfield spots; small nose and mouth; protruding tongue; low-set, dysplastic ears; and a short neck with nuchal skin.4,9
These patients often have comorbidities or complications that involve multiple organ systems.10 Most notable are cardiovascular complications and risk factors that impact cardiovascular event incidence. In addition, a population level matched cohort study revealed a higher risk of stroke, both ischemic and hemorrhagic, among people with DS compared to the general population.11 Respiratory problems are common in children and adults with DS, and may be associated with developmental delays, craniofacial abnormalities, immune deficiencies, gastroesophageal reflux, and cardiovascular disease.12,13
Gastrointestinal tract abnormalities appear in 12% of patients with DS and most commonly consist of celiac disease, chronic duodenal atresia, trachea-esophageal fistula, pyloric stenosis, anal-rectal atresia, and Hirschsprung disease.14 These conditions may lead to choking, gagging, feeding difficulties, and inadequate nutrition. Hearing loss can affect 40% to 75% of individuals with DS. Other common concerns include sinusitis, nasopharyngitis, enlarged tonsils, and obstructive sleep apnea.4,15,16
Orthopedic issues are experienced by approximately 20% of individuals with DS.17 Upper spine instability, most notably atlantoaxial instability causing increased mobility of the cervical spine at the first and second vertebrae, can lead to subluxation, neck pain, torticollis, changes in gait, paralysis, or weakness.
The presence of mental health disorders is understudied in children and young adults with DS.18 The National Down Syndrome Society reports the most common mental health concerns among individuals with DS include general anxiety; repetitive and obsessive-compulsive behaviors; oppositional, impulsive, and inattentive behaviors; depression; autism spectrum conditions; and neuropsychological problems associated with progressive loss of cognitive skills.19
TREATMENT AND PROGNOSIS
While there is no cure for DS, life expectancy has increased from 25 years in 1983 to 60 years presently.2 Multiple consultations and treatment options are indicated. Pediatric specialists, including cardiologists, pulmonologists, neurologists, orthopedists, and ophthalmologists, will be important team members to evaluate and treat for congenital heart defects, respiratory tract infections, eye disease, epilepsy, and atlantoaxial instability. A pediatric psychiatrist will be instrumental in coordinating interventions, family therapies, psychometric evaluations, behavioral management techniques, and supportive care. Physical and occupational therapists, speech-language pathologists, and audiologists may assist with rehabilitation requirements. As the child transitions to adolescence and adulthood, services will be important to support alternative living arrangements, social and recreational programs, sexuality and socialization, and adult healthcare.
While drug therapy is not a traditional treatment standard for those with DS, medications may be indicated for comorbid health problems. For example, rivastigmine, galantamine, memantine, and donepezil have been used to treat DS-associated dementia. Carbamazepine, phenytoin, and valproic acid may be indicated for seizure control. Inhaled bronchodilators are recommended to treat respiratory disorders and supplementation with levothyroxine is used for cases of hypothyroidism.20 Medications for managing congestive heart failure include digoxin, furosemide, hydrochlorothiazide, and metolazone.4 Individuals with DS are often socioeconomically disadvantaged, placing them at higher risk for nonadherence to medication management.20
ORAL HEALTH ISSUES
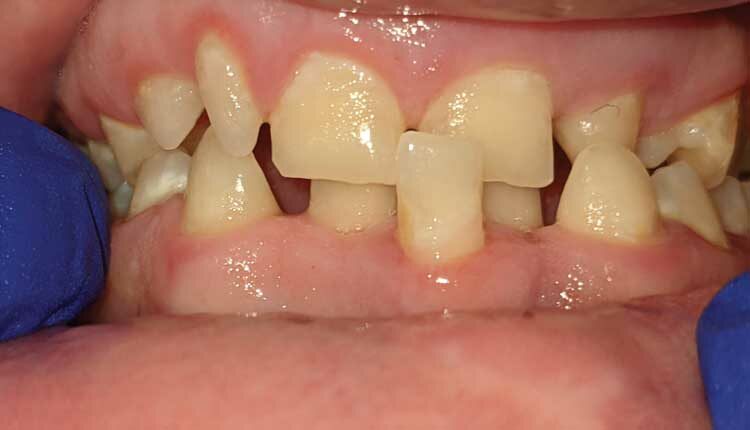
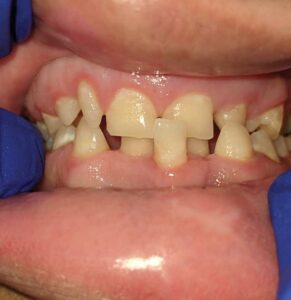
Several orofacial features are characteristic of individuals with DS. The maxilla, bridge of the nose, and bones of the midface are small, while the mandible is protruded, resulting in a prognathic profile. Class III malocclusion is common and the patient may also present with an anterior open bite and posterior crossbite (Figure 1). The palate may be short and narrow, with a high vault.21,22
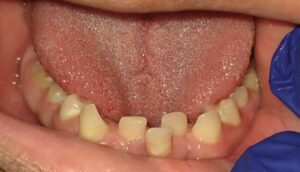
The lips are typically large, thick, dry, and fissured. A poor anterior oral seal may be noted, reflected as mouth drooping and lower lip protrusion. Mouth breathing is common, as is drooling that contributes to angular cheilitis. The tongue may be large and scalloped, representing macroglossia, and is often fissured (Figure 2). The deep fissures can trap food, causing oral malodor.21,22 A cross-sectional study of 50 children with DS and 50 age- and gender-matched healthy controls were compared to evaluate the prevalence of orolabial lesions and conditions. The findings revealed a high prevalence of fissured tongue (78%), lip fissures (64%), and angular cheilitis (38%) among subjects with DS.23 Hypotonic orofacial musculature can impact the ability to speak, chew, and swallow.21,22
Other oral complications may result from systemic conditions, such as leukemia and celiac disease. Signs of leukemia—a disorder for which these patients are at increased risk—include mucosal pallor, increased bleeding tendency, gingival hyperplasia, and anemia. Oral manifestations of celiac disease include glossitis and recurrent aphthous stomatitis.21
Tooth anomalies may be apparent in individuals with DS. Congenitally missing teeth occur, affecting third molars, lateral incisors, and mandibular second premolars most frequently.22 Delayed tooth formation and eruption may occur in which primary teeth can be 2 years or 3 years behind a normal eruption pattern. Exfoliation and sequence of eruption are subsequently affected. Other examples include hypodontia, impacted canines and premolars, peg lateral incisors, taurodontism, hypoplasia, hypocalcification, and unfavorable crown-to-root ratios that may increase tooth mobility and lead to early tooth loss.21,22
Periodontal diseases tend to be more severe and generalized in individuals with DS.24 Local risk factors may be associated with poor oral hygiene and malocclusion. General risk factors may include impairment of the immunological system and high levels of inflammatory cytokines.24 A study of the oral hygiene and gingival health status of 101 children with DS at a special-needs school revealed that all subjects had gingivitis and poor oral hygiene. The best predictors for plaque index were IQ level, age, and father’s education, while the most important predictors for poor gingival health status were severe mental retardation, older age, and having less educated parents. The authors concluded that tailoring appropriate oral health education was needed, along with ongoing support from teachers and parents.25 A systematic review of prevention and periodontal treatment in patients with DS demonstrated the importance of introducing preventive programs and periodontal therapy early. Including parents, caregivers, or institutional attendants in supervising and performing daily oral hygiene care is essential for the prevention and control of periodontal diseases. The use of chlorhexidine mouthrinses and disclosing agents appeared to improve periodontal outcomes and motivation to brush more thoroughly.24
Caries risk has been studied in individuals with DS and subsequently compared to the general population. A systematic literature review and meta-analysis examined the association between caries in individuals with DS compared to controls. Twenty-six studies were selected for full-text analysis; 13 studies were included in the systematic review and eight in the meta-analysis. Findings revealed that individuals with DS have significantly fewer dental caries than subjects without DS. Factors contributing to this result were orofacial characteristics of individuals with DS, such as microdontia, diastema, agenesis, delayed tooth eruption, and dental morphology. These factors contribute to the significant reduction in proximal caries lesions, chance of food collecting between teeth, and opportunity for smooth surface areas to be colonized by cariogenic bacteria.26
TREATMENT CONSIDERATIONS
Prior to performing any dental or dental hygiene treatment, a thorough risk assessment should be performed, including a comprehensive health history, dental history, pharmacologic history, and assessment of mental capabilities, communication skills, behavioral management, mobility issues, and parent/caregiver needs. Consultation with the patient’s chief medical provider is recommended given the significant comorbidities that could exist. It is also important to identify who can legally provide informed consent for treatment.21,22
When treating this patient population, communication is an important part of any successful dental appointment. Providers should prepare for each visit by speaking with parents or caregivers in advance about the patient’s needs. Involve the entire dental team in creating an environment that is friendly, caring, and supportive. Communicate respectfully with the patient and comfort those who express anxiety or are resistant to dental care. Allow for desensitizing appointments to help patients with DS become familiar with the office, staff, equipment, and procedures. Keep appointments short when possible and offer praise for cooperative behaviors. Try to end each appointment on a positive note.22
Some individuals with DS will experience rigid or loose masticatory muscles; others will present with drooling, gagging, or swallowing issues. Patient positioning can be adjusted to address these challenges. For example, if the patient has a frequent gag reflex, place his or her chin in a neutral or downward position. If a patient has a swallowing problem, tilt the head slightly to one side and place the body in a more upright position. Some patients may benefit from pillows to support the head.22
Regular preventive care is important for individuals with DS, and might include dental and dental hygiene therapy, nutrition counseling, professional and at-home fluoride therapy, mouthrinse use, and oral hygiene instruction for the patient and parent/caregiver. Ongoing reevaluation appointments to monitor motivation and outcomes are essential.
A study of individuals with DS found that if clinicians could successfully teach the patient and caregiver effective self-care strategies as part of the patient’s daily routine, gingival and periodontal issues could be controlled or eliminated. It was recommended that parents and caregivers be educated about the need to supervise toothbrushing for those with DS, regardless of the patient’s age. The author noted that oral hygiene was effective only if individuals with special needs are regularly helped by another person, emphasizing the significance of family members and caregivers in assisting those with DS.27
Dental treatment emphasis includes assessment of periodontal status and priority care for periodontal treatment, orthodontic consultation, and orofacial therapy for infants with DS.21,28 In addition, a qualitative study of mothers of children with DS explored how oral health affects the quality of life for these children and their families.29 The study involved interviews of mothers of children and adolescents attending DS centers, schools, and rehabilitation institutes. Three main themes emerged: oral health problems and functional limitations; impact of oral health on the child’s/adolescent’s quality of life; and impacts of the child’s/adolescent’s oral health on the family’s quality of life. These mothers reported that caries lesions and pain were common among their children, as were difficulty speaking or unclear speech.
These issues appear to have a wide range of impacts on the children’s lives, including physiological pain and negative impacts on daily activities, emotional state, and social interactions. For example, speech problems caused children to become depressed and angry if they thought they were not understood; this also affected their ability to make friends. Children exhibited pain-related behaviors, such as crying and anger, which improved if dental treatment was provided. The child’s oral health impacted the family’s quality of life, as well. Mothers described feeling neglectful if their child experienced oral-related pain, and they avoided going out if their child had pain. The authors concluded that oral health does have an impact on the life of individuals with DS and their families; therefore, attention to oral healthcare by dental providers is an important aspect of these patients’ overall health and well-being.29
CONCLUSION
As evidenced by this overview of DS, including its etiology, risk factors, comorbidities, and oral health considerations, individuals with DS may have multiple clinical and oral manifestations that require an interprofessional approach to care. Dental providers should carefully evaluate the patient, and assess all pertinent treatment considerations to ensure this population receives comprehensive oral care that will contribute to better oral and systemic outcomes, as well as improved quality of life.
REFERENCES
- United States Centers for Disease Control and Prevention. Data and statistics on Down syndrome. Available at: cdc.gov/ncbddd/birthdefects/downsyndrome/data.html. Accessed May 19, 2021.
- National Down Syndrome Society. Down Syndrome Fact Sheet. Available at: ndss.org/about-down-syndrome/down-syndrome-facts/. Accessed May 19, 2021.
- National Down Syndrome Society. What Is Down Syndrome? Available at: ndss.org/about-down-syndrome/down-syndrome/. Accessed May 19, 2021.
- Mundakel GT. Down syndrome. Available at: https://emedicine.medscape. com/article/943216-print. Accessed May 19, 2021.
- Vraneković J, Božović IB, Grubić Z, et al. Down syndrome: Parental origin, recombination, and maternal age. Genet Test Mol Boimark. 2012;16:70–73.
- Sherman SL, Lamb NE, Feingold E. Relationship of recombination patterns and maternal age among non-disjoined chromosomes 21. Biochem Soc Trans. 2006;34:578–580.
- Ghosh S, Feingold E, Dey SK. Etiology of Down syndrome: Evidence for consistent association among altered meiotic recombination, nondisjunction and maternal age across populations. Am J Med Genet A. 2009;149A:1415–1420.
- Hunter JE, Allen EG, Shin M, et al. The association of low socioeconomic status and the risk of having a child with Down syndrome: A report from the National Down Syndrome Project. Genet Med. 2013;15:698–705.
- US Centers for Disease Control and Prevention. Facts About Down Syndrome. Available at: cdc.gov/ncbddd/birthdefects/downsyndrome.html. Accessed May 19, 2021.
- Baum RA, Nash PL, Foster JE, et al. Primary care of children and adolescents with down syndrome: An update. Curr Probl Pediatr Adolesc Health Care. 2008;38:241–261.
- Sobey CG, Judkins CP, Sundararajan V, et al. Risk of major cardiovascular events in people with Down syndrome. PLOS One. 2015;10:e0137093.
- Jensen KM, Bulova PD. Managing the care of adults with Down’s syndrome. BMJ. 2014;349:g5596.
- McDowell KM, Craven DI. Pulmonary complications of Down syndrome during childhood. J Pediatr. 2011;158:319–325.
- Mazurek D, Wyka J. Down syndrome—genetic and nutritional aspects of accompanying disorders. Rocz Panstw Zakl Hig. 2015:66:189–194.
- Liyanage S, Barnes J. The eye and Down’s syndrome. Br J Hosp Med. 2008;69:632–634.
- Miyazaki EA. The orthoptics of Down syndrome. Am Orthopt J. 2014;64:12–16.
- Mik G, Gholve PA, Scher DM, et al. Down syndrome: orthopedic issues. Curr Opin Pediatr. 2008;20:30–36.
- Dykens EM, Shah B, Davis B, et al. Psychiatric disorders in adolescents and young adults with Down syndrome and other intellectual disabilities. J Neurodev Disord. 2015;7:9.
- National Down Syndrome Society. Mental Health Issues and Down Syndrome. Available at: ndss.org/resources/mental-health-issues-syndrome/#:~:text=The% 20most%20common%20mental%20health,progressive%20loss%20of%20cognitive%20skills. Accessed May 19, 2021.
- Hefti EJ, Blanco JG. Pharacotherapeutic considerations for individuals with Down syndrome. Pharmacotherapy. 2017;37:214–220.
- Aldosssary MS. Down syndrome: A review for the dental professional. IOSR J Dent Med Sciences. 2017;16:61–66.
- National Institute of Dental and Craniofacial Research. Practical Oral Care for People With Down Syndrome. Available at: nidcr.nih.gov/sites/default/files/2017-09/practical-oral-care-down-syndrome.pdf. Accessed May 19, 2021.
- Al-Maweri, SA, Tarakji B, Al-Sufyani GA, et al. Lip and oral lesions in children with Down syndrome. A controlled study. J Clin Exp Dent. 2015;7:e284–e288.
- Ferreira R, Michel RC, Greghi SL, et al. Prevention and periodontal treatment in Down syndrome patients: A systematic review. PLOS One. 2016;11:e0158339.
- Al-Sufyani GA, Al-Maweri SA, Al-Ghashm AA, et al. Oral hygiene and gingival health status of children with Down syndrome in Yemen: A cross-sectional study. J Int Soc Prev Community Dent. 2014;4:82–86.
- Deps TD, Angelo GL, Martins CC, et al. Association between dental caries and Down syndrome: A systematic review and meta-analysis. PLOS One. 2015;10:e0127484.
- Oredugba F. Oral health condition and treatment needs of a group of Nigerian individuals with Down syndrome. Down Syndr Res Pract. 2007;12:72–76.
- Sixou JL, Vernusset N, Daigneau A, et al. Orofacial therapy in infants with Down syndrome. J Dentofacial Anom Orthod. 2017;20:108.
- AlJameel AH, Watt RG, Tsakos G, et al. Down syndrome and oral health: mothers’ perception on their children’s oral health and its impact. Journal Patient-Reported Outcomes. 2020;4:45.
From Dimensions of Dental Hygiene. June 2021;19(6):32-35.



