Boost Your Optic Acumen
The right surgical magnification system can support your musculoskeletal health and improve treatment outcomes.
Medicine has used surgical magnification since the 1920s,1 but dentistry has only recently adopted this technology. Most American dental schools have integrated surgical telescopes to some extent and dental hygiene faculties are expressing increased interest in their integration. Surgical telescopes (Figure 1) are often called surgical loupes, although this term is ambiguous because “surgical loupes” also refers to single-lens magnification (Figure 2).
Surgical magnification helps dental hygienists see better and can reduce the risks for musculoskeletal discomfort and pain that often accompanies dental hygiene clinical practice.2 Tremendous advancements have been made in the materials and designs of surgical telescopes for dental practice and a variety of systems are now available to meet individual needs. Knowing what features are critical for your day-to-day practice is integral to selecting the best surgical magnification system for you.
Evidence
The benefits of surgical magnification include better visual acuity, greater motor control, improved diagnostic abilities, and better treatment outcomes.3-8 Some argue that surgical telescopes support improved clinical decision-making.9,10 Other studies have evaluated the outcomes of restorative procedures1,11,12 but not all found statistically significant differences for the use of surgical magnification.
Extrapolation of this evidence supports the benefit of greater visual acuity during assessments (eg, probe readings and tissue characteristics). However, acknowledging the use of tactile sensitivity and proprioception in the provision of dental care is also important.9,11,23
The most convincing argument for integrating surgical telescopes is based on studies related to the musculoskeletal health of dental hygienists. The results of a qualitative study at Vancouver Community College in British Columbia14 involving 25 dental hygiene students and clinical educators suggested physical health benefits of surgical magnification. The study participants reported decreased neck, back, and shoulder problems; decreased time leaning forward; decreased eye fatigue; and enhanced vision.
This was followed by a larger study conducted in 1999 to assess the musculoskeletal health and practice patterns of British Columbia dental hygienists.2 Of the 170 dental hygiene respondents in the study 15% used surgical magnification telescope systems of some sort and they reported less incidence of musculoskeletal problems in the lower back area (p [significance of statistical results] <.001). However, several other equipment and positioning variables were also correlated with problems in this and other areas.
|
|
Figure 2. Single-lens surgical loupes. |
While there is evidence that surgical magnification systems have the potential to support the musculoskeletal health of dental hygienists, their integration is not a sole solution for imbalanced position. The magnification system must not force clinicians to compromise their chosen working position. As with all equipment in the operatory, surgical telescopes must be adapted to the needs of clinicians, not vice versa.15 Clinicians must first determine their optimal balanced musculoskeletal position for providing care before making decisions about surgical magnification systems.
Balanced Positioning
Before purchasing surgical telescopes, first determine your most comfortable and natural working posture.16 This is not necessarily the posture in which you work but the posture that allows your muscles to be balanced and relaxed.
A balanced position is best determined by first closing your eyes and relaxing your muscles. Sit in free space (not leaning against the backrest) on your operator stool and adjust the height of the stool until it feels comfortable. Take time to explore the full range of options and focus on how your body feels. In most cases, individuals select a chair position where the seat of the chair is adjacent to the mid-point of the head of the fibula, located at the lower half of the kneecap. With arms resting at your sides, explore the options for your upper body by moving back and forth and side-to-side to find the most comfortable position.
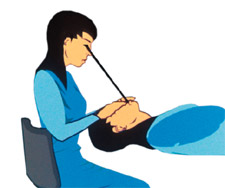
Now explore the same range to find a comfortable position for your head. With your arms still hanging loosely at your sides and your eyes closed, bring your thumbs and index fingers together, as if you were holding a needle. Raise your arms to the position you prefer if vision were not an issue. Now open your eyes to investigate the location of your fingers. If you cannot see your fingers, you need to decide whether to move your hands or tilt your head forward slightly. If you work through these steps and carefully rely on your internal feedback, the position you select represents your optimal working position (see Figure 3).

Optical Declination Angle
You need to select a system that meets your optical declination angle, working distance, and depth of field. The optical declination angle is the angle to which you lower your eyes when positioned in your optimal working position (see Figure 4). After establishing an optimal balanced musculoskeletal position, your declination angle can be measured with a protractor device. However, many clinicians assess this by first positioning themselves in their optimal working position with eyes closed and then opening their eyes to determine if the telescopes they are wearing match their optical declination angle. If you perform this assessment and need to adjust your head position to see the working field, then the scopes need to be adjusted or avoided.
If the declination angle is not matched to your musculoskeletal needs, you may experience eye strain and/or muscle strain of the head, neck, and back. While surgical telescopes can help promote your optimum positioning, they can also lock you into uncomfortable positions that can lead to pain or exacerbate the pain and discomfort you may already feel.
Working Distance and Depth of Field
The working distance is the distance between the clinician’s eyes and the working site. This measurement refers to the depth of field over which the clinician is able to see clearly. Depth of field is recorded in terms of the nearest and furthest extremes of distance from the surface of the eye to the object observed (eg, from 13 inches to 17 inches). It may also be recorded by the difference between these extremes (eg, in the above example, a 4-inch depth of field). Manufacturers may identify the characteristics of their magnification systems using these terms, but these factors need to be individually assessed because the depth of field provided by a particular system varies greatly between clinicians based on their vision. Younger clinicians tend to have greater depth of field so this particular factor is more important for older clinicians. However, analyzing working distance and depth of field carefully to determine that they meet your needs is crucial because they affect your ability to work comfortably and efficiently. These critical characteristics are best assessed in a clinical situation or one that closely approximates such an environment.
|
Figure 3. Self-derived balanced position. |
Figure 4. Optical declination angle. |
Choosing the Right System
With advancements in technology, consumers are presented with an ever-increasing number of surgical telescopes to choose from. A variety of surgical magnification systems are available including surgical microscopes; fixed spectacles-mounted (through-the-lens) telescopes; flip-up systems with and without vertical adjustability (Figure 1); and headband-mounted systems. The through-the-lens (TTL) telescopes originally provided the widest range of declination angles and they are lightweight. However, the weight of the flip-up telescopes is now often comparable to the TTL systems. Both allow for changes in declination angles, but the flip-up systems can be adjusted in a few moments by the clinician whereas TTL telescopes need to be shipped to the manufacturer for adjustment. Both types come in a wide range of frames and frame colors. The flip up systems can also be mounted on a head-band. When assessing frames, make sure the frame is large enough to provide protection and also does not obscure your vision at your optimal working posture.
Level of magnification
There are a variety of magnifications that can support operators’ balanced positions while providing dental hygiene care. However, less magnification is generally preferable—the higher the magnification, the smaller the actual field of view. Given that dental hygienists commonly work with sextants, quadrants, or the entire arch, a larger field of view is helpful. Higher magnification also reduces the depth of field, ie, the distance through which the particular area remains in focus without the operator having to move closer or further from the object viewed. The use of magnification also reduces the light available for vision. From our experience, most dental hygiene students select 2.0x or 2.5x magnification for their work.
Conclusion
Deriving a balanced position is the first step in selecting and adjusting surgical telescopes. Surgical telescopes need to be carefully assessed to ensure that their declination range, working distance, and depth of field support the individualized needs of the dental hygienist. If these are addressed, then integrating surgical telescopes has the potential to support the musculoskeletal health of dental hygienists and may also increase the quality of dental hygiene care. However, improperly selected or adjusted surgical telescopes can promote positions that place clinicians at increased risk for musculoskeletal problems. By themselves, surgical telescopes are not a cure for musculoskeletal problems experienced by dental hygienists. Like all equipment, they need to be carefully selected and adjusted.
References
- Leknius C, Geissberger M. The effect of magnification on the performance of fixed prosthodontic procedures. J CalifDent Assoc. 1995; 23:66-70.
- Sunell S, Rucker LM. Ergonomic risk factors associated with clinical dental hygiene practice. Probe. 2003; 37(4):159-166.
- Syme SE, Fried JL, Strassler HE. Enhanced visualization using magnification systems. J Dent Hyg. 1997;71(5):202-206.
- Chang BJ. Ergonomic benefits of surgical telescope systems: selection guidelines. JCalifDent Assoc. 2002;30:161-169.
- Simonsen FJ. The use of field magnification. Quintessence Int. 1985; 16:445.
- Coburn DG. Vision, posture and productivity. Practice Management. 1985;74(8):13-15.
- Strassler HE, Syme SE, Serio F, Kaim JM. Enhanced visualization during dental practice using magnification systems. Compend Contin Educ Dent. 1998;19(6):595-611.
- Andrews N, Vigoren G. Ergonomics: muscle fatigue, posture, magnification and illumination. Compend Contin Educ Dent. 2002;23(3):261-266, 268, 270.
- Mines P, Loushine RJ, West LA, Liewehr FR, Zadinsky JR. Use of the microscope in endodontics: a report based on a questionnaire. J Endod. 1999;25(11):755-758.
- Whitehead SA, Wilson NHF. Restorative decision-making behavior with magnification. Quintessence Int. 1992:23:667-671.
- Donaldson ME, Knight GW, Guenzel PJ. The effect of magnification on student performance in pediatric operative dentistry. J Dent Educ. 1998;62(11):905-910.
- Forgie AH, Pine CM, Pitts NB. Restoration removal with and without the aid of magnification. J Oral Rehabil. 2001;28:309-313.
- Rucker LM, Gibson G, McGregor C. Getting the “feel” of it: the non-visual component of dimensional accuracy during operative tooth preparation. J Can Dent Assoc. 1990;56(10):937-941.
- Sunell S, Maschak L. Positioning for clinical dental hygiene care: preventing back, neck and shoulder pain. Probe. 1996;30(6):216-219.
- Dainoff M, Dainoff MH. People and Productivity. Toronto, Canada: Holt, Rinehart, and Winston; 1986.
- Rucker LM. Surgical telescopes: posture maker or posture breaker? In: Murphy D, ed. Ergonomics and the Dental Care Worker. Washington, DC: American Public Health Association; 1998:191-216.
From Dimensions of Dental Hygiene. January 2004;2(1):14-16, 18, 20.