
Achieving Profound Local Anesthesia
The use of lesser known injections can offer myriad benefits—from improving patient comfort to providing longer lasting pain relief.
Profound anesthesia is essential to providing quality care during nonsurgical periodontal therapy (NSPT) and restorative and surgical procedures. The following lesser used injections offer significant benefits—such as profound anesthesia, improved patient comfort, fewer penetrations, and the administration of lower volumes of local anesthetic—compared to some more commonly employed techniques.
GOW-GATES NERVE BLOCK
The Gow-Gates nerve block is an excellent choice for initial anesthesia. It can also be used when an inferior alveolar nerve block (IANB) has been unsuccessful due to possible accessory nerve innervation or variations in anatomy. Traditionally, the IANB is used to provide anesthesia for mandibular teeth, with a success rate of 80% to 85% or less in some cases.1 According to Malamed,2 the Gow-Gates demonstrates a success rate of 97.5%. Additionally, the administration of the Gow-Gates may be more comfortable than the IANB because there is less resistance to needle advancement and the clinician is less likely to encounter dense anatomic structures in the upper part of the pterygomandibular space.3
In advanced cases of periodontitis or dentinal sensitivity, the Gow-Gates—with its extended anesthesia—can increase post-instrumentation comfort.4 This injection requires only one injection (the buccal is usually not needed), with a minimal positive aspiration rate of 2%.5 This reduces the number of penetrations, increasing patient comfort.5 The Gow-Gates anesthetizes the inferior alveolar and its terminal branches (incisive and mental), lingual, mylohyoid, auriculotemporal, and the buccal nerve 75% of the time.1,3–5

This line creates the positive angulation for
the barrel of the syringe.
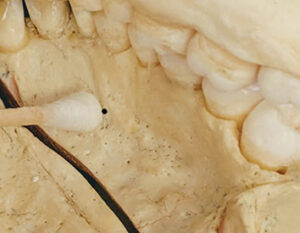
Considering that the depth of the Gow-Gates’ penetration is equal to or greater than that of the IANB, a long 25-gauge needle is recommended to minimize deflection during this injection.1,3,5 There are two landmarks to visualize when preparing for the Gow-Gates nerve block. Extraorally, observe the line from the intertragic notch (just below the tragus of the ear) to the labial commissure. This creates the slightly upward angulation of the barrel of the syringe (Figure 1). To establish the height of insertion, note the height of the mesiolingual cusp of the maxillary second molar.3–5 Good retraction is imperative to gain ideal illumination and visualization. Intraorally, find the landmark by first palpating the external oblique ridge with your thumb, then moving superiorly to palpate the coronoid process.1,3 With the thumb intraorally on the coronoid process, place the index finger extraorally over the intertragic notch (Figure 2).3,5 Insert the needle at the height of the mesiolingual cusp of the maxillary second molar (Figure 3) and distal to the maxillary second molar or third molar if present. The needle is directed toward the neck of the condyle with the syringe over the contralateral mandibular canines or premolars (Figure 4, page 18).3–5 This orientation is dependent on the flare of the ramus and condyle. Advance the needle slowly until the neck of the condyle is gently contacted (about 25 mm). If periosteum is not contacted, redirect the needle by positioning the barrel more posteriorly until you feel the neck of the condyle. Withdraw the needle 1 mm, aspirate, and administer a full cartridge if a negative aspiration is observed.1,3
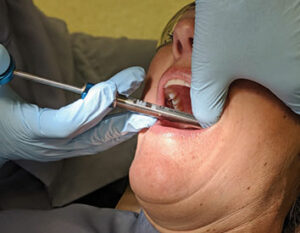
The position of the condyle neck is closer to the mandibular nerve trunk when the mouth is open wide.4,5 The patient should remain open during the entire procedure and for 1 minute to 2 minutes following deposition of the solution.5 This can be facilitated by placing a bite block in the mouth just after the needle is withdrawn and seating the patient in an upright position immediately following the injection.1,6 Note the onset of anesthesia is slower for the Gow-Gates nerve block than the IANB, with 5 minutes to 10 minutes frequently required.3,4
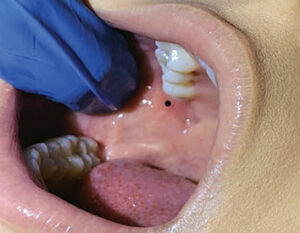
Common causes of injection failure may be due to lack of experience and familiarity with landmarks. A 2007 study at the Harvard School of Dental Medicine reported very few clinicians who were trained in the Gow-Gates nerve block chose to use it due to fear of straying from the conventional IANB, despite the reported advantages of the Gow-Gates injection.7 If inadequate anesthesia occurs, the following should be reevaluated: flare of the tragus, ability of the patient to keep his/her mouth open, volume of anesthetic deposited at the condyle, and promptly seating the patient upright following deposition of the solutions. The clinician may also want to consider using a higher concentrated anesthetic such as 4% articaine, 4% prilocaine, or 3% mepivacaine.3,6
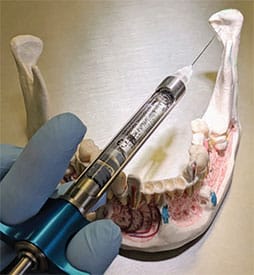
or premolars.
ANTERIOR MIDDLE SUPERIOR ALVEOLAR NERVE BLOCK
During the development of a computer-controlled local anesthetic device (CCLAD), the anterior middle superior alveolar (AMSA) nerve block was discovered.3–5 The porous nature of the palate and its multiple nutrient canals allow the local anesthetic solution to easily diffuse to the anterior superior alveolar and middle superior nerves (Figure 5).3,8
The AMSA nerve block injection is an additional option for NSPT. Benefits include: reduction in the number of tissue penetrations (saving time and increasing patient comfort), decrease in the total volume of local anesthetic and vasoconstrictor administered, and allows for an accurate assessment of the clinical “smile line.”8,9 Traditionally, a supraperiosteal injection into the mucobuccal fold is administered to anesthetize central incisors to the premolar area. Density of the bone, root length, type, dosage of anesthetic, and anatomy determine whether adequate pulpal anesthesia will occur from an infiltration. Multiple insertions may be necessary to achieve pain control. Only a portion of the solution administered reaches the target site, as some of the solution intended for the teeth at the injection site often dissipates into the soft tissues, resulting in numbness of the face and lip.9,10
Research demonstrates AMSA’s efficacy, and its use has grown in popularity.3,9 The AMSA nerve block provides 45 minutes to 90 minutes of profound anesthesia to the pulp, periodontium, and gingival tissues for areas traditionally covered by the anterior superior alveolar/infraorbital, middle superior alveolar, greater palatine, and nasopalatine nerve blocks. Hemostasis can also be achieved in the same region.3,10 Paired with the posterior superior alveolar nerve block, the clinician is able to anesthetize the entire maxillary quadrant with two injections vs four or five, and subsequently reduce the volume of anesthetic administered. The lack of anesthesia of the upper lip allows the patient to speak and eat, and decreases the risk of self-injury.9 Following careful procedures outlined for palatal injections, the AMSA nerve block can be administered with little or no pain.5
Malamed5 recommends a 27-gauge short needle. The optimum site for insertion is located between the maxillary premolars, halfway along an imaginary line between the median palatine raphe and gingival margin on the side to be anesthetized.3 Palatal injections can be made more comfortable using two steps. First, apply topical anesthetic for 1 minute followed by pressure anesthesia with a cotton tip applicator to increase patient comfort. Second, using a hard tissue fulcrum, place a cotton swab next to the insertion site and apply firm pressure during the entire process. The angle of needle insertion is approximately 45° to the palate with the bevel facing the bone and advancing slowly until periosteum is gently contacted.5 Depth of penetration is approximately 3 mm to 6 mm but often no more than the length of the needle bevel.4 Deposit 1.4 mL to 1.8 mL at a rate of 0.5 mL per minute.5 If administering a 4% solution, less drug should be administered and a slow deposition rate of less than 0.3 mL per minute should be used to decrease the risk of tissue injury and toxicity.3,4
Common causes of injection failure are inexperience, inadequate depth of penetration, and not enough volume of solution administered. Additionally, inadequate anesthesia of the incisors may occur if there is overlapping innervation by the contralateral anterior superior alveolar nerve. Excessive blanching and necrosis are more commonly seen when high concentrations of vasoconstrictors are used, therefore 1:50,000 concentrations should be avoided.5 Risks of complications with this injection are minimal.3
MENTAL/INCISIVE NERVE BLOCK
The mental nerve block, according to Malamed, is the least frequently used technique in all mandibular anesthesia.5 Areas anesthetized include the buccal soft tissue from the mental foramen to the midline and the lower lip and chin. The mental nerve is a terminal branch of the inferior alveolar nerve. Although no teeth or pulpal tissues are anesthetized, dental hygienists may find this block useful for NSPT when an IANB has not been successful for anesthetizing gingival tissues in the quadrant to the midline, or you only need anesthesia of anterior soft tissues.11 Advantages of this technically easy injection are a high success rate and sufficient hemostasis, in addition to it being largely atraumatic.
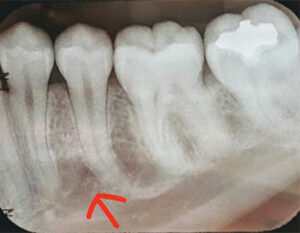
The landmark for the mental nerve block is the mental foramen, which is frequently located between the two mandibular premolars and commonly faces posteriosuperiorly. Radiographs are helpful when pinpointing the exact location of the foramen, as it may be located anteriorly or posteriorly (Figure 6).5 A 25-gauge or 27-gauge short needle is recommended and the insertion site is the mucobuccal fold between the premolars.12 The mental foramen can be palpated, and the periosteum will feel irregular and concave. Some patients state the area feels tender when palpated.5
For both the right and left blocks, the clinician has two options for operator positioning. The clinician may sit in front of the patient in order to keep the syringe out of the patient’s sight with an anterior approach, or the clinician may approach the insertion site from directly above the foramen from the 12:00 o’clock position. The bevel should be oriented toward the bone and tissues retracted. The approximate depth of penetration is 5 mm to 6 mm and 0.6 mL or 1⁄3 of the cartridge should be administered over a period of 20 seconds.5 The volume of anesthetic is lower when compared with the IA/lingual/buccal injections that require ¾ to 1 cartridge, especially if NSPT is only required for the soft tissues surrounding the mandibular anterior teeth.
The incisive nerve block anesthetizes both the mental and incisive nerves. It provides anesthesia to pulpal, periosteum, and buccal soft tissues, but not lingual soft tissues. It is useful when NSPT is required on the mandibular anterior sextant or when cross innervation exists and bilateral inferior alveolar blocks are contraindicated. The insertion site, landmarks, depth of penetration, needle size, and volume of anesthetic are identical to the mental nerve block. However, with the incisive nerve block, the clinician needs to apply light pressure over the foramen to force the anesthetic through the foramen for 1 minute. This will enhance the profoundness of the anesthesia following deposition of the solution. It is not necessary nor recommended to enter the foramen with the needle.5
Complications with both injections are few; the most common being a hematoma and swelling at the injection site. Rarely, short-term paresthesia of the lower lip or chin may occur if the needle contacts the mental nerve as it exits the foramen.
CONCLUSION
Providing profound anesthesia and becoming acquainted with alternative options is beneficial for both patients and clinicians. Minimizing the number of needle insertions may decrease patient anxiety and discomfort related to the administration of local anesthesia. Clinicians who are knowledgeable and skilled with a variety of injection techniques can increase the likelihood of obtaining profound anesthesia and enhancing patient care experiences.
REFERENCES
- Haas DA. Alternative mandibular nerve block techniques J Am Dent Assoc. 2011;142:8S–12S.
- Malamed SF. The Gow-Gates mandibular block. Evaluation after 4,275 cases. Oral Surg Oral Med Oral Pathol. 1981;51:463–467.
- Bassett KB, DiMarco AC, Naughton DK. Local Anesthesia for Dental Professionals. 2nd ed. Boston: Pearson; 2015:254–292.
- Logothetis DD. Local Anesthesia for the Dental Hygienist. St. Louis: Elsevier/Mosby; 2012:270–296.
- Malamed SF. Handbook of Local Anesthesia. 6th ed. St. Louis: Mosby; 2013:236–251.
- Kafalias MC, Gow-Gates GAE, Saliba GJ. A discussion and a mathematical analysis. Anesth Prog. 1987:8:142–149.
- Johnson TM, Badovinac R, Shaefer J. Teaching alternatives to the standard inferior alveolar nerve block in dental education: outcomes in clinical practice. J Dent Educ. 2007;71:1145–1152.
- de Souza Tolentino L, Barbisan Souza A, Girardi AA, Romito GA, Araújo MG. The anesthetic effect of anterior middle superior alveolar technique (AMSA). Anesth Prog. 2015;62:153–158.
- Corbett IP, Jaber AA, Whitworth JM, Meechan JG. A comparison of the anterior middle superior alveolar nerve block and infraorbital nerve block for anesthesia of maxillary anterior teeth. J Am Dent Assoc. 2010;141:1442–1448.
- Friedman MJ, Hochman MN. The AMSA injection: a new concept for local anesthesia of maxillary teeth using a computer-controlled injection system. Quintessence Int. 1998;29:297–303.
- Meechan JG. Infiltration anesthesia in the mandible. Dent Clin North Am. 2010;54:621–629.
- Royer R, Paarmann C, Bassett KB, DiMarco AC, Naughton DK. Techniques for Successful Local Anesthesia for Dental Professionals. Upper Saddle River, New Jersey: Prentice Hall; 2012.
From Dimensions of Dental Hygiene. March 2020;18(3):16–18,21.

