Analysis of the Two-Stage Injection Technique
One of the most important aspects of treating oral diseases is to ensure patients are free from pain during therapy. Because of this, many methods, techniques, agents, and equipment are dedicated to improving the patient and clinician experience with local anesthetic administration.

Ensuring Patients Are Pain Free
One of the most important aspects of treating oral diseases is to ensure patients are free from pain during therapy. Because of this, many methods, techniques, agents, and equipment are dedicated to improving the patient and clinician experience with local anesthetic administration. Individual dental practices often use a unique blend of methodology, anesthetics, and devices during local anesthesia administration. These individual approaches are typically based on differences in patient populations, clinician gender, practice location, provider and staff training, and business operations.
Photo Credit: Group4 Studio / E+

Body Processes
When pain is experienced, the central nervous system detects and processes tissue damage and/or bodily danger (with the goal of removing the body from harm). Generally, type A and type C nerve fibers are involved during the dental injection process. The type A nerve fibers respond to mechanical stimulation and relay the sensation of pain described as sharp or vivid, while type C nerve fibers respond to thermal or chemical stimuli and are associated with dull or burning sensations. The process of local anesthetic injection and nerve fiber activation includes the needle penetrating mucosa and advancing to the target area (type A); anesthetic deposition (type A and type C); and removal of the needle (type A and type C).
Photo Credit: aga7ta / iStock / Getty Images Plus
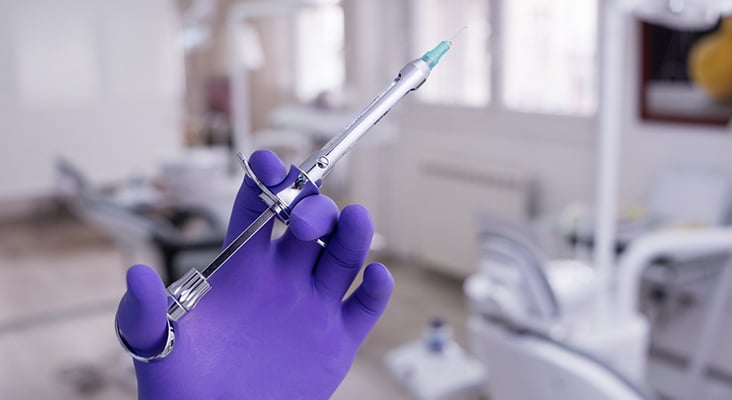
Pain Experience
Introduction of the needle into the mucosa is the first step of the injection pain experience. Previous analysis of pain perception during this stage demonstrated a 14% to 22% incidence of moderate to severe pain with standard injection protocols. Considered the more painful stage of an anesthetic injection, the deposition of solution elicits intense responses due to the expansion of tissue, the rich sensory innervation seen intraorally, and the chemical complexion and pH of the local anesthetic. Pain analyses for anesthetic deposition found an incidence of moderate to severe pain at 18% to 56%, during the anesthetic deposition stage. Additionally, needle withdrawal can be associated with post-operative pain due to tissue damage or an expedited removal of the anesthetic delivery device. Post-operative pain has also been associated with the pH of the anesthetic, multiple injections, inadequate needle design, and poor injection technique.
Photo Credit: milosljubicic / iStock / Getty Images Plus
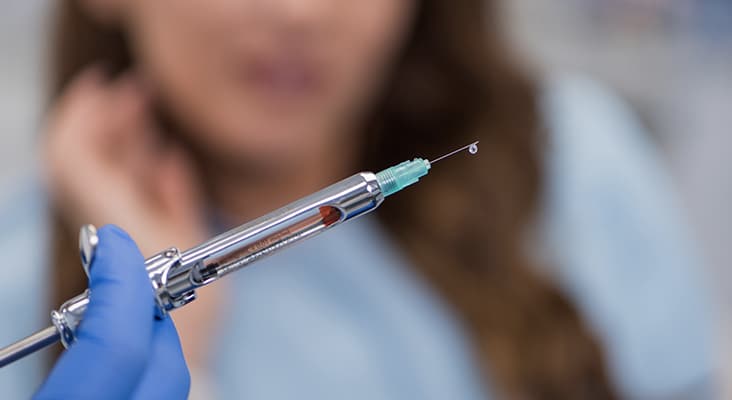
First Step in the Technique
The first step in the two-stage injection technique is to prepare the mucosa by thoroughly drying the area (gauze and air) and applying a topical anesthetic gel. The next step is to introduce the needle into the mucosa at a depth of 2.0 mm to 5.0 mm, depositing 0.3 mL to 0.5 mL of anesthetic. After 5 minutes, the delivery device is re-introduced at the previous puncture zone, advanced slowly to the target area for completed anesthetic deposition, and then withdrawn.
Photo Credit: bulatovic / iStock / Getty Images Plus
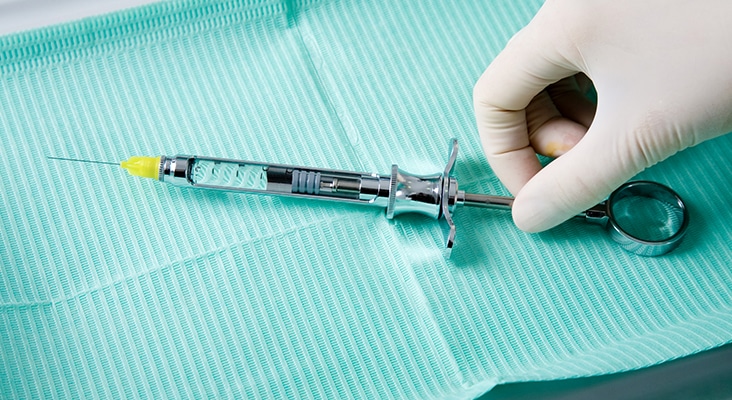
Expectation of Pain
Although it can be applied at several injection sites, the two-stage injection technique is most often used with inferior alveolar nerve blocks (IANB). Anecdotal reports suggest that the two-stage injection technique is a better alternative for IANB compared to the traditional Halstead method. These reports propose the two-stage injection technique as a solution to the unreliable effect of topical anesthetic for IANB injections. While current evidence points to an unreliability of topical benzocaine anesthetic for IANB injections, some reports have found a psychological connection with topical anesthetics as it relates to reducing the expectation of pain and a belief that the clinician is doing everything possible to reduce the pain.
Photo Credit: Brosa / iStock / Getty Images Plus

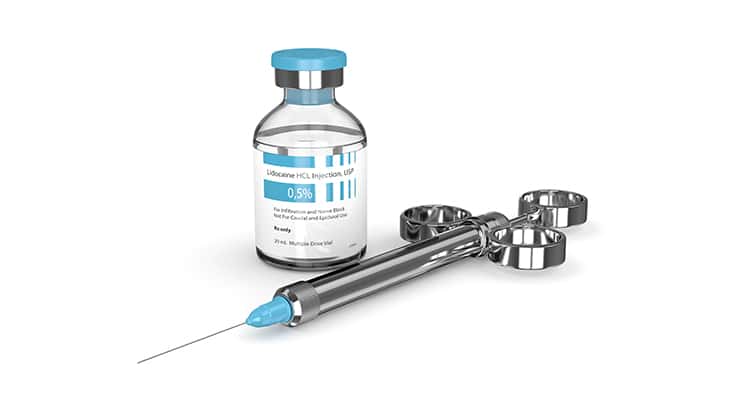
Anesthetic Selection
Anesthetic selection for the two-stage injection technique depends on provider preference and patient characteristics. The technique is often associated with 4% prilocaine plain as the primary agent used for the shallow injection, followed by lidocaine or articaine for the target site anesthetic deposition. Local anesthetics vary in their characteristics and effects. The use of 4% prilocaine plain is proposed as the primary agent for the two-stage injection technique because of the solution’s pH value of 6.0 to 7.0. Several authors have proposed that the more acidic the anesthetic solution, the more likely a patient will report a higher pain score. Anesthetics with vasoconstrictors have a lower pH value (3.0 to 5.0), while 4% prilocaine plain possesses the highest pH value (6.0 to 7.0), followed by 3% mepivacaine plain (4.5 to 6.8).
Photo Credit: Banannaanna / iStock / Getty Images Plus
Technique Tips
Many variables affect the success of the two-stage injection technique. Anesthetic selection should be a controllable variable; however, conclusive information on the best agent(s) is limited. The majority out of 24 studies found no significant difference between the anesthetics being tested 70.8%, (17 of 24 studies). Out of 17 studies that investigated different anesthetics with vasoconstrictors, 13 (76.5%) found no significant differences between the agents. Three of 14 studies (21.4%) that evaluated lidocaine found 2% lidocaine w/1:100,000 epinephrine to provide the least discomfort of the agents compared, and three of five (60%) analyses involving 4% prilocaine plain determined that the agent provided the least painful experience during injection. In one study comparing lidocaine 2% w/1:80,000 epinephrine and 4% articaine w/1:100,000, articaine was found to produce the least pain response. Additionally, some correlation was observed with vasoconstrictor presence and higher discomfort. The completion of a comprehensive meta-analysis is needed to evaluate these observations and expand the evidence base for best practice.
Photo Credit: ayo888 / iStock / Getty Images Plus
More Research Needed
Unfortunately, the available science on the two-stage injection technique, as well as the best anesthetic agents and pain response is limited. Visual Analog Scale for Pain scoring with anesthetic agent comparisons is usually a secondary finding, if evaluated. There are also too few studies and reviews to achieve professional consensus on the benefits, risks, and best practices of the two-stage injection technique, and no studies were found that evaluated all available United States anesthetics within one cohort.

