Oral Biofilm Disruption
Biofilms are composed of bacteria adhering to each other or to living or nonliving surfaces.

Biofilms are composed of bacteria adhering to each other or to living or nonliving surfaces. They form complex communities surrounded by extracellular polymeric substances. Cells within these biofilms have changing physiologic and metabolic properties that contribute to their persistence. If not removed regularly, a complex and mature biofilm develops, with up to 100 bacterial species at a single site. Oral biofilm exposed to an excess of carbohydrates contains mainly Gram-positive carbohydrate-fermenting bacteria that may cause demineralization, caries, pulpitis, and periodontitis. Supra- and subgingival oral biofilms dominated by Gram-negative anaerobic bacteria colonize and cause gingival inflammation. Subsequently, gingivitis, chronic and aggressive periodontitis, and peri-implantitis can ensue. There are two strategies for biofilm control: interfere with attachment, and remove or disrupt biofilm. Total removal is not possible; therefore, disruption is the most practical option.
Photo Credit: colematt / iStock / Getty Images Plus

Effects of Toothbrushing
Toothbrushing is the most powerful way to disrupt supragingival biofilm at home, preventing colonization of microbes subgingivally. Research shows that both manual toothbrushing and power toothbrushing result in a reduction of plaque scores. Power toothbrushes have different modes of action to improve efficacy, such as sonic, ultrasonic, rotating, counter-oscillating, oscillating rotation, back and forth, and side to side. Systematic reviews found that power and manual brushing are at least equally effective in removing plaque, reducing gingival inflammation, and preventing calculus formation.
Photo Credit: Hiraman / E+

Adding Antibacterials
Adding antibacterial ingredients within dentifrice is helpful for biofilm management. When combined with fluoride (for caries prevention), antibacterial pastes provide an efficacious option for combating oral diseases. Stannous fluoride has antibacterial effects against species associated with plaque, gingivitis, caries, and malodor, and it reduces plaque, gingival inflammation, and bleeding. Triclosan/copolymer fluoride dentifrices reduced gingival inflammation and gingival bleeding when compared with conventional fluoride dentifrices.
Photo Credit: Bet_Noire / iStock / Getty Images Plus

Interdental Care
Patients should be educated about interdental self-care. In fact, interdental biofilm is more prevalent, acidogenic, and readily forming than other oral biofilm. Evaluation of patients’ interdental space accessibility should be part of all routine oral examinations. Floss does not meet the intraoral and personal needs of all patients. Also, compliance with daily flossing is low. Nevertheless, dental floss is ideal for those who can use it effectively and patients with type I gingival embrasure spaces and shallow pockets. Flossing in addition to toothbrushing enhances interproximal biofilm disruption by 70% compared with 25% by brushing alone.
Photo Credit: RyanKing999 / iStock / Getty Images Plus

Mouthrinse Option
Evidence supports the use of antimicrobial mouthrinses in addition to mechanical biofilm disruption for most patients. These antiseptic rinses act on the oral biofilm’s ability to form, grow, and mature. Evidence supports the efficacy of chlorhexidine and essential oils. Benefits for plaque and gingivitis were also shown with cetylpyridinium chloride. Patients with orthodontic appliances, mental or physical disabilities, systemic diseases, and smokers may particularly benefit from antimicrobial mouthrinse use.
Photo Credit: AndreyPopov / iStock / Getty Images Plus
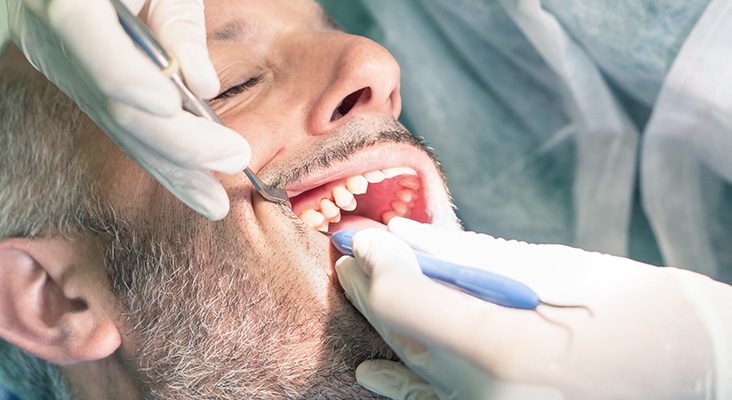
Mechanical Debridement
Mechanical biofilm disruption by the professional occurs both in the supragingival (oral prophylaxis/debridement) and the subgingival environment (scaling and root planing/debridement). Mechanical debridement of the subgingival environment remains the cornerstone of periodontal therapy. Although not a permanent solution to biofilm removal, mechanical therapy temporarily disrupts its aggregation.

