Is Estrogen Related to TMD?
Affecting the quality of life for more than 10 million Americans, temporomandibular disorders (TMDs) are musculoskeletal conditions associated with pain and dysfunction of the temporomandibular joint (TMJ) and muscles of mastication.
Affecting the quality of life for more than 10 million Americans, temporomandibular disorders (TMDs) are musculoskeletal conditions associated with pain and dysfunction of the temporomandibular joint (TMJ) and muscles of mastication. The pain and dysfunction associated with TMDs are more prevalent among women during reproductive years, suggesting estrogen plays a role in TMD pathophysiology. Studies describe the potential role of hormonal fluctuations as a contributing risk factor for TMD-related pain. Furthermore, evidence suggests estrogen is a prominent hormone, influencing both inflammatory and pain processes.
Photo Credit: Evgeny Gromov / iStock / Getty Images Plus

Role of Estrogen
Estrogen can produce inflammation through various mechanisms of action including stimulation of toll-like receptors (TLR) in the immune system, upregulation of voltage-gated sodium channels, expression of estrogen receptors, or due to genetic variations called polymorphism. Stimulation of TLR promotes inflammation by signaling leukocytes (monocytes and macrophages) and glial cells (immune cells in the central nervous system) to release pro-inflammatory messenger molecules known as cytokines. Estrogen acts by binding two types of steroidal estrogen receptors: estrogen receptor alpha (ERα) and estrogen receptor beta (ERβ). Found in both the peripheral nervous system and central nervous system, these receptors are present in TMJ muscles.
.
Photo Credit: Zerbor / iStock / Getty Images Plus

Women at Risk
Bueno et al proposed that women, compared with men, are more predisposed to TMDs, which suggests that gender disparities may play a role in the pathophysiology of this condition. Researchers have found estrogen may influence pain receptors, which may highlight the differences between male-female TMD-related pain. Fluctuation of estrogen levels occur before puberty, during menstruation, and after menopause, all of which may impact a woman’s pain threshold. Subsequently, pain onset occurs after puberty and peaks in reproductive years, but tapers after menopause. Evidence suggests that estrogen inhibits inflammatory processes associated with TMD-related pain. During periods of high estrogen concentration levels, the inflammatory process is inhibited and TMD-related pain decreases. Contrastingly, during the menstrual cycle, post-menopause, and following an ovariectomy, low levels of estrogen occur; consequently, lower levels of estrogen induce pro-inflammatory effects within the TMJ, resulting in higher pain levels.
Photo Credit: monkeybusinessimages / iStock / Getty Images Plus
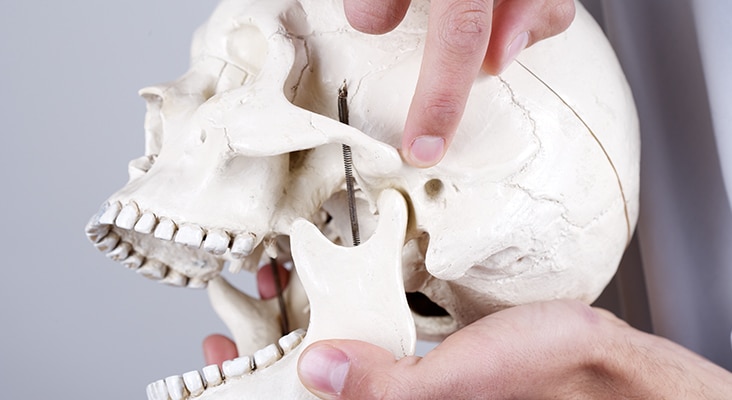
In the Dental Operatory
Treatment modalities for patients experiencing TMD-related pain include self-regulated strategies, anti-inflammatory medications, hormone therapy, botulinum toxin injections, acupuncture, occlusal splint therapy, and surgical interventions used to treat both peripheral nervous system and central nervous system components of TMD-related pain. Relaxation and biofeedback therapies are commonly used self-regulated strategies for patients with TMD-related pain. However, these therapies are still considered controversial. Multiple drugs may also be used for the management of TMD pain, such as nonsteroidal anti-inflammatory drugs (NSAIDs), corticosteroids, analgesics, muscle relaxants, anxiolytics, opiates, tricyclic antidepressants, gabapentin, and lidocaine patches. The risk of polypharmacy and/or patient dependency, however, must be considered. The use of NSAIDs, often used as a long-term treatment option, only alleviate the symptoms rather than effectively treating the TMD. Topical ointments or creams may be used as an alternative to oral medications that may cause adverse systemic effects.
Photo Credit: marvinh / iStock / Getty Images Plus

Hormone Replacement Therapy
The use of hormone replacement therapy (HRT) in menopausal women and its relationship on TMD-related care has previously been studied. In 1997, LeResche et al studied the prevalence of TMD-related pain among women who used exogenous forms of hormone replacement. They found that increases in the dosages of estrogen positively correlated with the number of women seeking referral for TMD-related care. Results suggested that women using a 185 mg annual cumulative estrogen dosage exhibited a 36% increased probability for receiving a referral for TMD-related care. Interestingly, the probability for receiving a referral for TMD-related care escalated to 84% likelihood among women using a 220 mg annual cumulative estrogen dosage.
Photo Credit: syahrir maulana / iStock / Getty Images Plus
Botox
The use of botulinum toxin-a, a biological exotoxin produced by Clostridium botulinum, has been suggested as a viable treatment for myogenous TMDs. Research suggests that regardless of type, number of injections, and dosage, botulinum toxin-a appears to be effective for TMJ-related muscle disorders. In 2019, Sipahi-Calis et al studied the efficacy of botulinum toxin injections for the treatment of TMD-related pain. Results show that 36% (n = 25) of study participants found beneficial effects, and no side effects, at the 6-month follow-up. Even though these results look encouraging, it also demonstrates that this treatment may not be effective for everyone.
Photo Credit: Ake Ngiamsanguan / iStock / Getty Images Plus
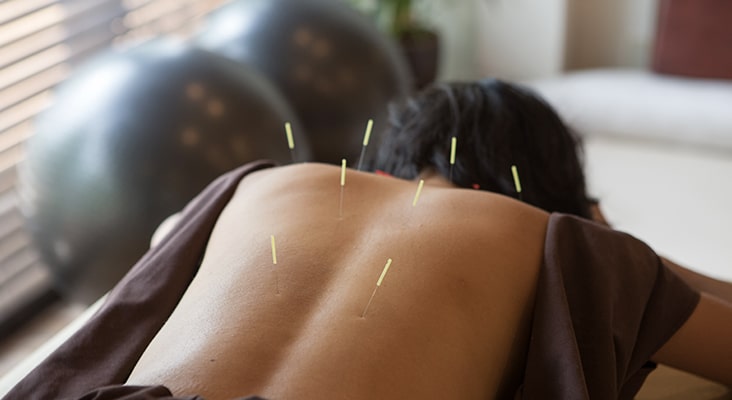
Alternative Therapies
Splint therapy and acupuncture are comparable in providing pain relief. These two therapies are more beneficial for myogenous TMDs affecting the muscles, rather than arthogenous TMDs that affect the joints. Splint therapy is also frequently used with TMDs associated with clenching or bruxism, to help correct occlusion and biting forces. Acupuncture can also serve as an alternative to managing chronic pain frequently associated with TMD. Acupuncture relieves pain by using needles at the appropriate acupuncture points. The therapeutic effects of acupuncture, such as needle placement and how deep the needle is inserted, can vary among therapists, and the probability of success may not be the same for all patients with TMDs.
Photo Credit: tekinturkdogan / E+
Missing Link
To date, there is no universally agreed upon gold standard intervention for treating patients with TMD-related pain. A variety of conservative and surgical treatment modalities exist; however, evidence-based oral health professionals are advised to provide treatment based on the unique needs of each individual patient. Current therapies for managing TMD-related pain focuses on alleviating symptoms, rather than addressing the root causes of TMDs. Future research should investigate the origin of TMD-related pain and determine the role estrogen receptors plays in targeting inflammation, including how estrogen may be integrated to alleviate pain associated with TMDs.

