 STOCKBYTE/GETTY IMAGES PLUS
STOCKBYTE/GETTY IMAGES PLUS
Strategies for Managing Burning Mouth Syndrome
While its etiology is unclear, the symptoms of burning mouth syndrome can be effectively addressed with a personalized patient treatment plan.
This course was published in the April 2019 issue and expires April 2022. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Define burning mouth syndrome (BMS).
- Identify the symptoms of BMS.
- Differentiate between primary BMS and secondary BMS.
- List the current methods used to manage BMS.
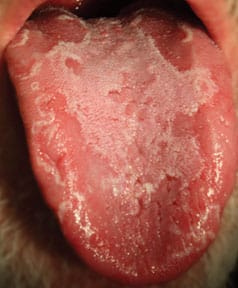
Burning mouth syndrome (BMS) is a condition characterized by severe, chronic pain in the oral cavity affecting the tongue and the mucosal tissue of the mouth lips and/or the palate.1 BMS can be considered a diagnosis of exclusion because there are numerous conditions—local or systemic—to which a burning sensation may be attributed.1–12 Conducting a comprehensive clinical examination is important to rule out all secondary causes to diagnose true idiopathic BMS. Local factors include parafunctional habits, candidiasis, geographic tongue (Figure 1), and xerostomia, the most common complaint associated with BMS. Systemic factors include but are not limited to gastroesophageal reflux, diabetes, and nutritional deficiencies.1,2,4–10,13 If a systemic or local condition cannot be identified, BMS is more specifically identified as primary BMS.2–6 Although poorly understood,2 oral health professionals should be familiar with the symptoms and possible causes of BMS to guide patients to the appropriate treatment.
Data on the prevalence of BMS vary due to the lack of consensus on diagnostic criteria among professionals.1,3,5,7,12,14 BMS has a reported prevalence between 0.7% and 15%,5,15 and may affect five out of every 100,000 individuals worldwide.7 Women of perimenopausal and post-menopausal age are the most commonly affected.1,3,5,7,8,12,16 Approximately 90% of women affected are going through menopause.17 Although less common, men and women younger than 40 can be impacted.5 Occurrence is rare among individuals younger than 30, and there is currently no documentation of children and adolescents presenting with symptoms.8,11 Studies have suggested a male to female ratio of 1:5 to 1:7.5, with prevalence increasing with age among both groups.5,11,12
CHARACTERISTICS
Primary BMS is defined as a severe, disabling, and chronic intraoral pain condition for which no local or systemic cause can be found with a traditional clinical exam.1,5 Manifestation of BMS varies, but, in most cases, the symptoms are not physical changes but changes in sensation. The sensations associated with BMS are described as burning, scalding, tingling, numb, or itching.5,8,12,14,16 The affected tissues, including oral mucosa, lip, and tongue, usually appear healthy with no lesions or physical changes in appearance; however, there are cases identified where patients present with a geographic tongue.14,18 The pain is typically bilateral occurring on the anterior two-thirds of the tongue with the tip and lateral borders being the most commonly affected sites (Table 1).5,8,12,16 The lips, palate, buccal mucosa, and floor of the mouth are also areas reported by patients with BMS but less common than the tongue.5,12,14
The duration of symptoms also varies. Onset of BMS may occur suddenly or gradually, increasing in intensity throughout the day.5 In 2010, Lopez et al8 proposed to classify BMS into three types according to the daily fluctuation of symptoms. Type I BMS affects approximately 35% of patients and is characterized by pain that increases in intensity throughout the day and may be associated with systemic diseases. Affecting approximately 55% of patients, Type II BMS is characterized by pain that is consistent throughout the day to the point of disrupting sleep. These patients may present with psychological disorders, as psychological factors may play a role in the etiology, progression, and severity of BMS. Type III BMS occurs in approximately 10% of patients and is characterized by symptoms that are intermittent occurring on atypical locations that may be the result of contact with allergens in the oral cavity. Symptoms may last for 6 months or several years, with only 3% of cases resolving over 5 years.1,14 The duration of BMS symptoms increases with the presence of secondary causes.
Xerostomia is a condition commonly reported by individuals with BMS.1,2,6 A study by Poon et al19 concluded that decreased unstimulated salivary flow was associated with BMS, suggesting that mild hyposalivation may cause the xerostomia commonly reported by this population.19 Among patients with BMS, between 11% and 69% have reported alterations in taste.1,2,5,8,14,16 Sour and bitter tastes are generally perceived to be stronger, sweet tastes perceived as weaker, and salty tastes are generally perceived as either weaker or stronger.5 Two-thirds of patients experience phantom tastes and smells described as bitter or metallic.5,14
ETIOLOGY
The exact etiology of BMS is not clear. Scientific evidence suggests that the hormonal fluctuations associated with stress and anxiety may cause neurodegenerative alterations in the small nerve fibers of the oral mucosa, triggering pain in the mouth and manifesting as a burning sensation, dysgeusia, and xerostomia.13,17 There are many conditions, both locally and systemically, in which BMS is a secondary condition.1–7 Local factors within the oral cavity include but are not limited to: localized allergic reaction; mucosal diseases; oral lesions; mechanical or chemical irritation; poorly fitting oral prosthesis that causes microtrauma or erythema; parafunctional habits, such as tongue thrust; continual rubbing of the tongue over the teeth or an oral prosthesis; buccal, labial, and lingual biting; and compulsive movements of the tongue.5,8 Various oral infections have been associated with BMS, most frequently Candida albicans infection.8 Oral infections with Klebsiella, Enterobacter, and Streptococcus aureus also frequently occur in patients with BMS.8
Materials used in dental care, such as mercury, amalgam, methyl methacrylate, cobalt chloride, zinc, and benzoyl peroxide, may cause an allergic reaction on a patient’s tongue or oral mucosa, resulting in BMS symptoms.1
In addition to the localized factors associated with the manifestation of BMS, systemic factors may play a role.1,2,5,7,8,14 These include diabetes mellitus, thyroid dysfunction, immunological disorders, and hormonal changes. Nutritional and vitamin deficiencies such as vitamin B12, B6, folate, iron, and zinc may also be underlying conditions in patients with BMS.5,8,13 The presence of any of the aforementioned conditions is not always the same in each individual, making diagnosis difficult.5,8 Allergies to certain foods, such as peanuts, sorbic acid, chestnuts, and cinnamon, may also be associated with the manifestation of BMS.1
Recent studies have revealed a connection between BMS and neuropsychiatric disorders.1,11,13 Approximately 85% of individuals with BMS have psychosocial and psychological characteristics, with depression and anxiety as the most common.2,3,5,8,11,13,14 However, the causal relationship between BMS and psychological disorders is not clear.14 The presence of anxiety, stress, and depressive disorders can either enhance or reduce the perception of pain.8 Based on results from their cross-sectional study, Rabiel et al15 surmised that a 60-year-old woman with psychological disorders is 25 times more likely to experience BMS compared with a 50-year-old man who has no psychological disorders.
Studies have been conducted to find an underlying physical manifestation of BMS. Some studies have cited evidence of a histopathological change in nociceptive nerves.1 Lopez et al8 reported that biopsies of the tongues of individuals with BMS revealed less dense epithelial and subpapillary nerve fibers compared with control subjects, indicating that axonal degeneration may occur. Feller et al14 reported a decreased number of small-diameter nerve fibers in the lingual mucosa, suggesting that BMS may result from trigeminal neuropathy. Miziara et al3 reported that neuropathic changes may be involved in the manifestation of BMS due to the presence of significant changes in thermal nociception. While it has been suggested that nerve dysfunction may be a factor in BMS, it is not known if the dysfunction originates in the peripheral or central nervous system.3 Other studies have suggested that the association between BMS and age, gender, and menopause could be due to hormonal changes.17 Although BMS typically does not present with visible changes in the tissues of the oral cavity, geographic tongue is currently the only visible physical change identified as a risk factor for the manifestation of BMS.14,18 Symptoms of BMS do not always manifest the same in every patient; therefore, patients with BMS will not always present with a geographic tongue and patients with a geographic tongue will not always exhibit symptoms of BMS.
The presence of any of the aforementioned local and systemic factors classifies the manifestation of BMS symptoms as secondary. BMS is considered idiopathic and can be classified as primary BMS when none of the local or systemic factors can be identified as the possible cause of oral discomfort.
MANAGEMENT![Oral cavity sites affected by burning mouth syndrome]()
If a patient presents with symptoms of BMS, oral health professionals should look at patients’ dental histories to see if they were exposed to dental materials that may cause an allergic reaction, evaluate the oral mucosa and look for erythema, or identify an oral prosthesis in areas affected. It is crucial to check for and rule out all possible factors within the oral cavity that may cause BMS. If a potential local factor is identified, treating the patient for that condition may provide relief. A thorough review of his or her medical history may reveal systemic conditions known to be associated with BMS. Oral health professionals should discuss this information with patients and provide a referral to see a physician for further evaluation and treatment.
Patients need to know that there is currently no cure for BMS, and that treatment is focused on managing BMS symptoms and any underlying conditions. Results vary for each person; what provides relief for one patient may not provide relief for the next patient.
Some medications may be potentially effective, but, more research in this area is still needed.2,3,13 Clonazepam, a benzodiazepine with an inhibitory effect on the central nervous system, shows promise in treating BMS symptoms by relaxing the muscles and providing pain relief.2,3,12 However, clonazepam can result in dependence and can cause xerostomia, lethargy, and fatigue; symptoms will return once use of this medication is discontinued.12 Capsaicin, a component of peppermint, is another medication used for management of BMS.3 Capsaicin is an analgesic that can desensitize peripheral nociceptors and control neuropathic pain; it has been reported to significantly reduce the burning sensation of BMS.3,12 Side effects are an increase in the burning sensation after topical application and gastric pain when taken systemically after long-term use.2,12 As such, patients with a history of gastric disorders should use caution with capsaicin or seek an alternative treatment.
Research has been conducted to evaluate the effectiveness of alpha lipoic acid (ALA) for treating BMS.2,12 ALA is a mitochondrial enzyme with neuroprotective properties that could assist with repair of neural damage.2,12 Further research is needed; some studies conclude that it is not effective,12 while others show promise in its ability to manage BMS.2,11 When used with ALA, the anticonvulsant medication gabapentin, was found to reduce pain in 70% of patients.2,11 The antidepressant amitriptyline has also shown promise in managing BMS due to its analgesic properties.2,12 Side effects include drowsiness and xerostomia.2,12
When medications are ineffective, some evidence suggests psychological/psychiatric intervention may be needed.14 Cognitive behavioral therapy (CBT) is an effective method for the management of BMS. CBT is traditionally used for treatment of depression and anxiety; in reference to BMS, CBT focuses on education, distraction, evaluation of harmful automatic thoughts, and the replacement of those thoughts with more beneficial ones.2 Ritchie et al2 reported that several studies demonstrated that CBT was effective in reducing pain after 12 sessions to 15 sessions and that CBT used in combination with ALA may be more effective than using either treatment alone, but further research in needed to explore their efficacy.
Other approaches to managing BMS include the use of the herbal supplement catuama, a Brazilian herbal product made of the extracts of four plants that exerts an analgesic and antidepressant effect when used.3,13 The topical application of aloe vera may protect the oral mucosa from repeated trauma.3,12 To treat pain, the ancient Chinese healing technique of acupuncture has been used for BMS management. Acupuncture studies showed significant improvement in pain manifestation; however, the studies were conducted in China with small samples in local populations, increasing the possibility of bias.3 Further research is needed to ascertain the effectiveness of acupuncture in managing BMS pain.
Patients presenting with BMS pain should be advised to avoid dental products with additives, flavoring agents, whitening agents, or anti-calculus ingredients, because they may irritate oral tissues.12 Patients should avoid spicy foods, mints, or gum because these may also aggravate the condition. For patients who present with parafunctional habits, fabricating a protective appliance may be beneficial. Patients who grind their teeth should use a night guard, and patients with a tongue thrusting habit or constant tongue rubbing may benefit from a soft plastic appliance that extends into the vestibule and floor of the mouth, or cover the palate to prevent the tongue from rubbing against these surfaces.12
CONCLUSION
Symptoms of BMS manifest differently for each individual.20 The lack of consensus on diagnostic criteria makes diagnosis difficult.20 Oral health professionals should know what to look for in regards to BMS. A thorough medical history review is needed to rule out systemic conditions that may cause the oral discomfort. Identifying the various local and systemic factors that can result in secondary BMS is the first step in managing this condition. Dental professionals can then advise patients on how to treat the local ailments in the oral cavity. If the oral examination is normal, but systemic conditions are present, the patient should be referred to a medical professional for further evaluation and treatment. Treating the local and systemic conditions may resolve oral discomfort. Although many treatments show promise, further research is needed to gain a better understanding of the etiology of BMS in order to provide more effective therapies. The available research on the management of BMS has provided inconclusive results.20 Further research is needed on managing symptoms with larger patient populations over longer time periods to determine the efficacy of the available therapies.20 Educating patients on the condition and management options may reduce anxiety. By listening to and working with patients to find the most effective management strategies, oral health professionals can significantly impact the success of BMS treatment.
REFERENCES
- Bookout GP, Short RE. Burning Mouth Syndrome. Available at: ncbi.nlm.nih.gov/books/NBK519529/. Accessed March 22, 2019.
- Ritchie A, Kramer JM. Recent Advances in the Etiology and Treatment of Burning Mouth Syndrome. J Dent Res. 2018;97:1193–1199.
- Miziara I, Chagury A, Vargas C, Freitas L, Mahmoud A. Therapeutic options in idiopathic burning mouth syndrome: literature review. Int Arch Otorhinolaryngol. 2015;19:86–89.
- Jääskeläinen SK. Pathophysiology of primary burning mouth syndrome. Clin Neurophysiol. 2012;123:71–77.
- Bender SD. Burning mouth syndrome. Dent Clin North Am. 2018;62:585–596.
- Ikeda-Miyagawa Y, Kobayashi K, Yamanaka H, et al. Peripherally increased artemin is a key regulator of TRPA1/V1 expression in primary afferent neurons. Mol Pain. 2015;11:8.
- de Souza IF, Mármora BC, Rados PV, Visioli F. Treatment modalities for burning mouth syndrome: a systematic review. Clin Oral Investig. 2018;22:1893–1905.
- Lopez-Jornet P, Camacho-Alonso F, Andujar-Mateos P, Sánchez-Siles M, Gómez-Garcia F. Burning mouth syndrome: an update. Med Oral Patol Oral Cir Bucal. 2010;15:e562–568.
- Patton LL, Siegel MA, Benoliel R, De Laat A. Management of burning mouth syndrome: systematic review and management recommendations. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103(Suppl):e1–13.
- Soto MA, Rojas GA, Esguep A. Association between psychological disorders and the presence of oral lichen planus, Burning mouth syndrome and recurrent aphthous stomatitis. Med Oral. 2004;9:1–7.
- Charleston L. Burning mouth syndrome: a review of recent literature. Curr Pain Headache Rep. 2013;17:336.
- Burkhart NW. Burning mouth syndrome. Available at: dentalcare.com/en-US/dental-education/continuing-education/ce434/ce434.aspx. Accessed March 22, 2019.
- Lewis AK, Prime SS, Cohen SN. An overview of burning mouth syndrome for the dermatologist. Clin Exp Dermatol. 2016;41:119–123.
- Feller L, Fourie J, Bouckaert M, Khammissa RAG, Ballyram R, Lemmer J. Burning mouth syndrome: aetiopathogenesis and principles of management. Pain Res Manag. 2017;2017:1926269.
- Rabiei M, Leili EK, Alizadeh L. Burning mouth syndrome: a comparative cross-sectional study. Contemp Clin Dent. 2018;9(Suppl 2):S256–260.
- Patton LL, Siegel MA, Benoliel R, De Laat A. Management of burning mouth syndrome: systematic review and management recommendations. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103(Suppl):1–13.
- Barbosa NG, Gonzaga AKG, de Sena Fernandes LL, et al. Evaluation of laser therapy and alpha-lipoic acid for the treatment of burning mouth syndrome: a randomized clinical trial. Lasers Med Sci. 2018;33:1255–1262.
- Grushka M, Su N. Burning mouth syndrome. In: Ferreira JNAR, Fricton J, Rhodus N, eds. Orofacial Disorders. Berlin, Germany: Springer International Publishing; 2017: 223–232.
- Poon R, Su N, Ching V, Darling M, Grushka M. Reduction in unstimulated salivary flow rate in burning mouth syndrome. Br Dent J. 2014;217:e14.
- Klasser GD, Grushka M, Su N. Burning mouth syndrome. Oral Maxillofac Surg Clin North Am. 2016;28:381–396.
From Dimensions of Dental Hygiene. April 2019;17(4):40–43.





Thank you, I have a patient suffering with this and this article was very informative,