
Bruxism in Children
Research on the etiology of bruxism is mixed and the prevailing treatment of bruxism in children is “wait and see.” This overview sheds some much-needed light on this common problem.
This course was published in the February 2011 issue and expires February 2014. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Define bruxism.
- Discuss the prevalence of bruxism in children.
- Explain the theories about the etiology of bruxism.
- List the symptoms of bruxism.
Derived from the Greek word “brychein,” bruxism means tooth grinding. The term was first introduced in 1931 when it was used to describe involuntary, excessive grinding, clenching, or rubbing of the teeth during nonfunctional movements of the masticatory system. More recently, it has been further defined as a diurnal (when it happens during the day) or nocturnal (when it happens at night) parafunctional activity. It refers to movements of the jaws that are outside of the normal functional activity of the teeth and jaws (eg, speaking, chewing, or swallowing).
Children are susceptible to habits conducted without consciousness, such as nail and cheek biting and non-nutritive sucking. In children, bruxing when awake, which manifests as clenching of the teeth, often occurs without any cognitive awareness, especially during stressful situations or intense concentration. When the child is made aware of the activity, the bruxism can be stopped or modified. On the other hand, sleep bruxism, which presents as grinding or clenching of the teeth during sleep, cannot be consciously stopped by the child. The International Classification of Sleep Disorders reclassified bruxism in 2005 as a sleep-related movement disorder, rather than its previous classification as a parasomnia, which is an undesirable movement occurring during sleep. This puts it in the same category as restless leg syndrome and sleep walking.
PREVALENCE
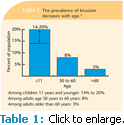
The prevalence of bruxism in children is difficult to determine because estimates are generally based on parental reporting or clinical finding of tooth wear. The occurrence of bruxism may be variable over time, so finding tooth wear is not necessarily indicative of current tooth grinding. The prevalence of bruxism in children varies greatly—from 7% to 88%.1 Children younger than 11 years are most affected with a reported prevalence of 14% to 20%.1 In healthy infants, sleep bruxism typically starts at about 1 year, soon after the eruption of the primary incisors. Bruxism appears in approximately 13% of 18- to 29-year-olds1 and then significantly decreases with age (see Table 1).2
The research is not definitive on the role of gender and the prevalence of bruxism. While some studies indicate there is no significant gender effect on the prevalence of bruxism, others report that girls are more frequently affected.1,3 It does appear to be more common in individuals with developmental disabilities, particularly those with profound mental retardation, autism spectrum disorder, and Down syndrome.4
The role of genetics in bruxism is also unclear, however, an association appears to exist between child and parental bruxism. Based on self-reports, 20% to 50% of sleep bruxism patients have an immediate family member who experienced tooth grinding in childhood.5 Bruxism shares a common genetic background with sleep talking, a parasomnia.6 Although recent publications favor the role of genetics in the etiology of bruxism, to date, neither genetic markers nor the exact genetic mechanism have been identified.
ETIOLOGY
The etiology of bruxism is a controversial phenomenon, but the consensus is that it is multifactorial. Basically two groups of etiological factors can be distinguished: peripheral (morphological factors), and central (pathophysiological and psychological) factors. Morphological factors include occlusal discrepancies and anomalies of articulation of the orofacial region, however, research shows the elimination of interferences in occlusion and articulation has no influence on bruxism activities.7 Moreover, experimentally-placed deflective occlusal contacts do not seem to elicit bruxism.7 Therefore, not every child with bruxism has occlusal interferences, and not all children with such interferences have bruxism.8
It is often difficult to determine in children whether tooth attrition is due to bruxism because the occlusal surfaces of primary teeth become ground physiologically. One theory about how bruxism starts in children is the occlusion instability created during the replacement of the primary teeth by the permanent dentition. Studies, however, have failed to show a significant role of occlusal discrepancies in the genesis of sleep bruxism with no evidence for a role of occlusion and articulation in its etiology.8
BRUXISM AND SLEEP
Pathophysiological factors are believed to play a role in the precipitation of bruxism. In younger children, bruxism may be due to the immaturity of the masticatory neuromuscular system. Current thinking is that bruxism is part of an arousal response. An arousal response is a sudden change in the depth of sleep during which a person either arrives at a stage of lighter sleep or wakes up. In young adults, more than 80% of sleep bruxism episodes occur during sleep stages 1 and 2 of nonREM (light sleep stages), and 5% to 10% in REM (deep stages).5 Many bruxism episodes lead to a shift in sleep stage, usually toward awakening or lighter sleep.
TABLE 2. SYMPTOMS OF BRUXISM16.
- Anxiety, stress, and tension
- Depression
- Earache
- Eating disorders
- Headache
- Hot, cold, or sweet sensitivity in the teeth
- Insomnia
- Sore or painful jaw
There appears to be a relationship with the autonomic nervous system in that there is increased cortical and autonomic cardiac activity preceding bruxism activity. Bruxism is often seen in patients with altered states of consciousness and is a common complication in children who have sustained traumatic brain injury. Resolution of the bruxism is often associated with improvement in consciousness in patients who were initially comatose and the return of sleep-wake cycles. Bruxism appears at several levels of consciousness but it usually only disappears after a substantial improvement in consciousness occurs.
The involvement of the dopaminergic system may play a role in sleep bruxism, but this idea remains controversial. The long-term use of medications that exert an indirect influence on the dopaminergic system— such as antidepressant medications, including selective serotonin reuptake inhibitors—may cause bruxism. The number of children taking this type of drug is growing, so this is an important factor to consider when treating children with bruxism. Hyperactivity is associated with bruxism and the am pheta mines used for managing attention deficit hyperactivity disorder can also cause bruxism.3
RESPIRATORY FACTOR
Bruxism and habitual snoring are closely related. Sleep bruxism is also a frequent complaint of parents of children who are mouth breathers. One theory suggests there is a correlation between bruxism and upper airway obstruction, with obstructive sleep apnea causing sleep bruxism. Bruxism does appear to be more prevalent when sleeping in a supine position, which correlates with a greater possibility of airway obstruction. A link has also been made between bruxism and tonsilar hypertrophy, which is strongly correlated to upper airway obstruction. Adenotonsillectomy surgery has been shown to improve bruxism in some children.9 Bruxism may also be caused by allergic processes such as asthma and respiratory airway infection.10
OTHER PATHOPHYSIOLOGICAL FACTORS
Pathophysiological factors implicated in bruxism among adolescents include smoking, alcohol, illicit drugs, trauma, disease, and medication. In addition, a host of diseases among children have been linked to bruxism such as basal ganglia infarction, cerebral palsy, Down syndrome, epilepsy, Leigh disease, meningococcal septicemia, multiple system atrophy, gastroesophageal reflux, and Rett syndrome.
In comatose patients, bruxism and clenching are common. These behaviors can inflict injuries to the teeth and soft tissues, often requiring some type of intervention that may include the use of various mouth props, prosthetic appliances, or botulinum-A injections intraorally to relieve muscle spasticity. These treatments can then be discontinued when consciousness is regained.
PSYCHOLOGICAL FACTORS
Stress and personality have been implicated in the etiology of bruxism. Bruxism, either clenching while awake or grinding during sleep, is associated with stress and anxiety. The exact mechanism by which these and other psychological factors contribute to the etiology of bruxism is still unknown. Emotionally stressful states are often manifested physiologically by an increase in the endogenous release of catecholamines (epinephrine, norepinephrine, and dopamine). Patients with bruxism have elevated levels of catecholamines in their urine in comparison to patients without bruxism.11 But the majority of data about the association between psychosocial disorders and bruxism come from studies that use clinical or self-reporting to achieve their diagnosis as opposed to sleep laboratory investigations.
One report12 studied bruxism as it relates to other factors such as aggression and somatization (the process by which psychological distress is expressed as physical symptoms). The report indicated that an increased amount of aggression and somatization can already be found in bruxing 5- and 6-year-olds. A study by Restrepo et al13 investigated the effectiveness of psychological techniques in children with bruxism. They used different psychological techniques including directed muscle relaxation for 6 months in children age 3 years to 6 years who had a history of bruxism. They found that the psychological techniques used were effective in the reduction of signs of bruxism in children with primary teeth. A case report by Antonio et al14 described two cases of children who had tooth wear attributed to bruxism. In both cases, the condition was believed to be triggered by psychological disturbances resulting from harrowing experiences. Based on the emotional problems of the children, they were referred for psychological monitoring.
Bruxism is found in those who suffer from post-traumatic stress disorder, further suggesting that a psychological etiology may be involved. A recent systematic review by Manfredini et al15 concluded that while wake clenching seems to be associated with psychological factors and a number of psychopathological symptoms, there was no evidence to support that these factors were implicated in sleep bruxism.
SYMPTOMS
Table 2 lists some common symptoms of bruxism.16 Assessment of bruxism is fraught with methodological problems, however. Methods such as questionnaires and interviews, observation of tooth wear, electromyography, and muscle symptoms are used but there are inherent problems with these methods. Questionnaires and interviews rely on recall and may lead to under or over-reporting. Dental wear may be evident, however, it may not indicate a current bruxism habit. Each method has inherent flaws and there still is no agreement on the ideal method of recording this parafunction. It is also difficult to determine if the wear found in children in the primary dentition is from bruxism alone or the involvement of other variables such as diet or endogenous factors. The rise of soft drink consumption in children has also contributed to the development of tooth wear and erosion in this population.
The relationship between temporomandibular disorder (TMD) and bruxism is controversial and unclear.3 Studies have demonstrated an association between bruxism and signs and symptoms of TMD in children and adolescents, whereas other studies have not. The unreliability of the clinical assessment of bruxism also reduces conclusions about this relationship. Bruxism in children and adolescents could be associated with muscular disorders but there is little evidence to link it with disk displacement or other joint pathologies.
TREATMENT
Bruxism is so common that it is often considered normal behavior. It is only when a child has severe tooth damage and reports pain, sleep is interrupted, or the noise is sufficient to disturb parents that it may become a pathological condition. Others assert that bruxism cannot be considered normal even during the beginning of the mixed dentition.17
The available literature does not provide adequate support to treat bruxism in children. The most common treatment for bruxism is the rigid occlusal splint, which has not been proven effective in the primary dentition. Because children generally outgrow the condition, treatment is not recommended. Children with upper airway obstruction or severe psychological problems should be referred to a specialist. In children or adolescents who are taking medications for conditions that may cause bruxism, other options should be discussed with the patients’ primary care provider.
Treatment of bruxism in children with developmental disabilities may be more challenging. Given the negative impact and high prevalence of bruxism in developmental disability populations, treatment for this disorder is a priority. According to Lang et al, intervention approaches for this population may include prosthodontics, dental surgery, behavior modification, music therapy, massage, and the injection of botulinum-A toxin.4 However, Lang et al concluded that the evidence base is extremely limited and no definitive statements regarding treatment efficacy can be made.
CONCLUSION
Until the etiology of bruxism is definitely determined, treatment options will remain based on anecdotal evidence. There is also not much of an evidence base to support the management of bruxism in children. Clearly, well-designed studies on the management of bruxism in children are needed.
REFERENCES
- Cheifetz AT, Osganian SK, Allred EN, Needleman HL. Prevalence of bruxism and associated correlates in children as reported by parents. J Dent Child (Chic). 2005;72:67-73.
- Macedo CR, Silva AB, Machado MA, Saconato H, Prado GF. Occlusal splints for treating sleep bruxism (tooth grinding). Cochrane Database Syst Rev. 2007;(4):CD005514.
- Barbosa TDS, Miyakoda LS, Pocztaruk RDL, Rocha CP, Gavião MBD. Temporomandibular disorders and bruxism in childhood and adolescence: Review of the literature. Int J Pediatr Otorhinolaryngol. 2008;72:299-314.
- Lang R, White PJ, Machalicek W, et al. Treatment of bruxism in individuals with developmental disabilities: A systematic review. Res Dev Disabil. 2009;30:809-818.
- Lavigne Gj, Khoury S, Abe S, Yamaguchi T, Raphael K. Bruxism physiology and pathology: an overview for clinicians. J Oral Rehabil. 2008;35:476-494.
- Hublin C, Kaprio J, Partinen M, Koskenvu M. Parasomnias: co-occurrence and genetics. Psychiatr Genet. 2001;11:65-70.
- Negoro T, Briggs J, Plesh O, Nielsen I, McNeill C, Miller AJ. Bruxing patterns in children compared to intercuspal clenching and chewing as assessed with dental models, electromyography, and incisor jaw tracing: Preliminary study. ASDC J Dent Child. 1998;65:449-458.
- Lobbezoo F, Naeije M. Bruxism is mainly regulated centrally, not peripherally. J Oral Rehabil. 2001;28:1085-1091.
- DiFrancesco RC, Junqueira PA, Trezza PM, de Faria ME, Frizzarini R, Zerati FE. Improvement of bruxism after T & A surgery. Int J Pediatr Otorhinolaryngol. 2004;68:441-445.
- Grechi TH, Trawitzki LVV, de Felício CM, Valera FCP, Alnselmo-Lima WT. Bruxism in children with nasal obstruction. Int J Pediatr Otorhinolaryngol. In Press.
- Vanderas AP, Menenakou M, Kouimtzis T, Papagiannoulis L. Urinary catecholamine levels and bruxism in children. J Oral Rehabil. 1999;26:103-110.
- Kuch EV, Till MJ, Messer LB. Bruxing and nonbruxing children: A comparison of their personality traits. Pediatr Dent. 1979;1:182-187.
- Restrepo CC, Alvarez E, Jaramillo C, Velez C, Valencia I. Effects of psychological techniques on bruxism in children with primary teeth. J Oral Rehabil. 2001;28:354-360.
- Antonio AG, Pierro VS, Maia LC. Bruxism in children: A warning sign for psychological problems. J Can Dent Assoc. 2006;72:155-160.
- Manfredini D, Lobbezoo F. Role of psychosocial factors in the etiology of bruxism. J Orofac Pain. 2009;23:153-166.
- Medline Plus. Bruxism. Available at: www.nlm.nih.gov/medlineplus/ency/article/001413.htm. Accessed January 17, 2010.
- Restrepo C, Gomez S, Manrique R. Treatment of bruxism in children: A systematic review. Quintessence Int. 2009;40:849-855.
From Dimensions of Dental Hygiene. February 2011; 9(2): 56-59.



