Supporting the Success of Sealants
Choosing the right sealant material depends on a variety of factors, including patient needs. Dental sealants were developed in the 1960s by Michael Buonocore, DDS, and dental scientists at the Eastman Dental Center in Rochester, New York.
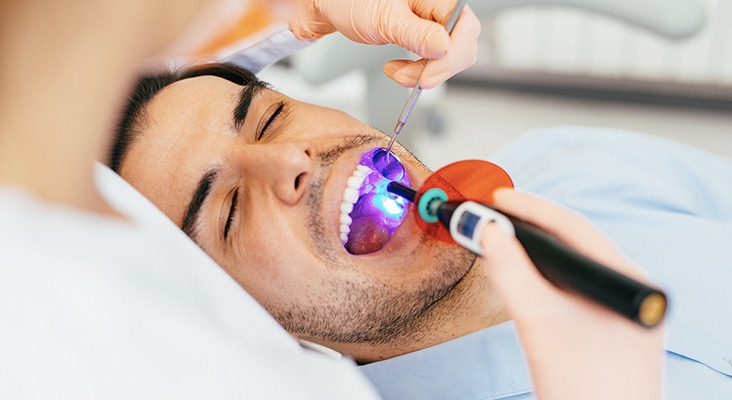
Selecting the Best Material
Choosing the right sealant material depends on a variety of factors, including patient needs. Dental sealants were developed in the 1960s by Michael Buonocore, DDS, and dental scientists at the Eastman Dental Center in Rochester, New York. A thin plastic coating of an organic polymer (resin), a sealant is placed into the pits and fissures of newly erupted molar teeth that are susceptible to dental caries. This placement acts as a physical barrier, sealing off the pit or fissure from caries-producing oral bacteria, thereby preventing decay. Sealants can help shield grooved areas of the tooth where fluoride toothpaste is not as protective. They can reduce caries by approximately 80% in 2 years after initial placement and may remain effective for nearly 5 years. Sealants cost one-third less than a restorative filling and can be placed after an initial assessment verifies no extensive decay is present. Some research shows that sealant placement in areas of early decay can help to control and manage caries on occlusal and approximal surfaces. There are two main types of sealants: resin and glass ionomer cements (GICs).
Photo Credit: filadendron / E+
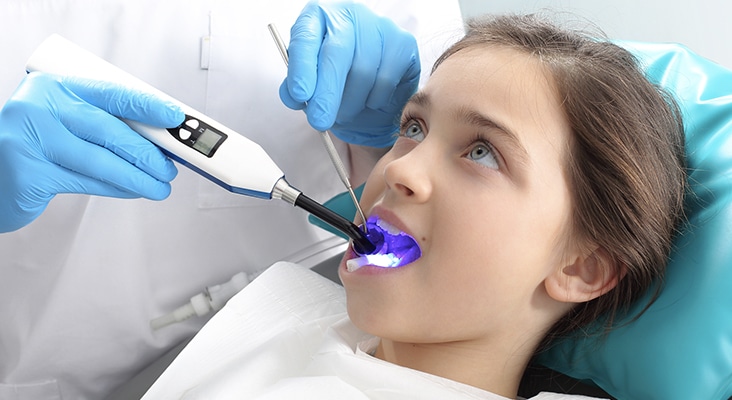
Resin-Based Sealants
Sealants are categorized by color, fluoride releasing or nonfluoride releasing, method of polymerization (hardening), and filler content (silica, glass, or quartz particles added to increase strength and resistance to occlusal wear). The variety of colors ranges from clear to tinted and opaque, which aid in the sealant’s application into pit and fissures and margin identification during retention checks. Sealants containing fluoride increase resistance to caries formation and remineralize incipient carious lesions. Many sealants are composed of dimethyacrylate monomers that may include bisphenol A-glycidyl methacrylate (Bis-GMA); they are classified as self-cured (autopolymerized) or light-cured (photopolymerized). Unfilled sealants are clear (making placement difficult to see), may not require occlusal adjustment, and are less resistant to wear over time. Filled sealants can be tinted, and may require occlusal adjustment after placement and light curing.
Photo Credit: robertprzybysz / iStock / Getty Images Plus
Application
Safety glasses should be donned by all patients to provide a barrier to the acid etch solution and cure light. The use of resin-based sealants that are photopolymerized shrink toward the source of the curing light, and therefore may be prone to marginal leakage. The phosphoric acid (etch) solution used when placing resin sealants should not contact the patient’s oral tissues. Resin sealants may require self-etching bonding agents, which may not provide as good retention as acid-etch techniques. Some sealant material retention is dependent on moisture control achieved by maintaining a dry field during etching and placement. However, some resin materials can be placed in a moist field. Overmanipulation of sealant material by the clinician may result in air bubbles and voids, decreasing the sealant’s effectiveness.
Photo Credit: ayo888 / iStock / Getty Images Plus
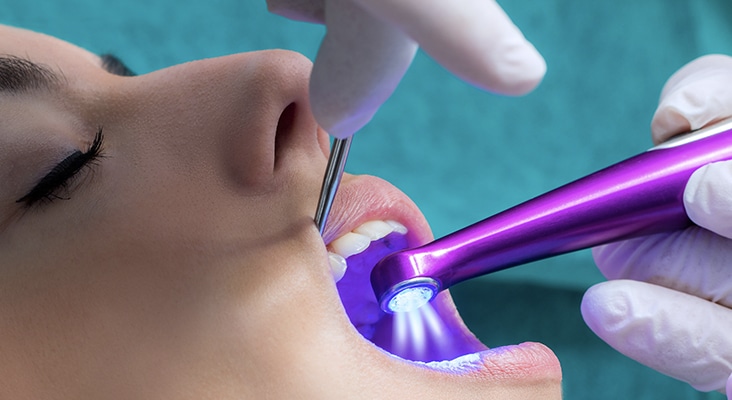
Glass Ionomer Sealants
GICs are composed of aluminosilicate glass (powder) and polymeric water-soluble acid (liquid) set through an acid-base reaction that is mixed to form a viscous paste. GICs are less acidic compared to zinc phosphate, more compatible with dental pulp, set within 2 minutes to 3 minutes, and can be hand-mixed using a spatula. The material can also be presented in a capsule separated by a membrane, which is broken prior to the capsule being vibrated in an amalgamator for a set time. GICs have been used in dentistry to repair cervical lesions (both carious and non-carious), cavity liners/bases, fissure sealants, orthodontic band and bracket materials, and as a luting cement since the early 1970s. Type I cements are luting and bonding materials used for cementing crowns, bridges, inlays, onlays, and orthodontic appliances. They are fast-setting and water resistant. RMGIs contain a polymerisable resin known as hydroxyethyl-methacrylate (HEMA) that may have the additional setting reaction of a resin, which may be self-curing and/or light curing. RMGIs can be used as interim therapeutic restorations (ITRs) and for application in the atraumatic restorative technique (ART).
Photo Credit: karelnoppe / iStock / Getty Images Plus

Fluoride Release
Due to their fluoride-releasing properties that may last several years, GICs and RMGIs are indicated for restoration of root caries; Class V abrasion and erosion lesions; and Class I, Class II, and Class III caries on primary teeth. RMGIs have increased strength, easy flow ability into pits and fissures, and improved wear and resistance compared with GIs. All glass ionomers can be placed in less than ideal clinical situations and enable chemical bonding to both enamel and dentin; thermal expansion similar to that of tooth structure; and reduction in hypersensitivity. Glass ionomers are also hydrophilic, meaning they have a tendency to absorb water and may be placed in the presence of moisture. Lastly, glass ionomers can act as a fluoride reservoir, with absorption occurring from the use of mouthrinses, dentifrices, and topic fluoride applications. This may provide protection from secondary decay formation.
Photo Credit: Paladjai / iStock / Getty Images Plus

Decision-Making Process
Deciding on which type of sealant material to use depends on myriad factors. The benefits of both materials are based on retention and integrity in pit and fissures and fluoride release over time. Resin sealants typically provide greater longevity than GICs. For instance, research shows that light-cured resin sealants were retained in pits and fissure of molar teeth longer than glass ionomers. Other studies, however, suggest that neither material was superior to the other in caries prevention. Glass ionomer sealants are recommended in ITR and ART. In the final determination of material selection, oral health professionals should assess the clinical situation, as well as individual patient factors/needs to obtain the ultimate goal—caries prevention.

