Oral Health and Schizophrenia
Schizophrenia is a chronic brain disorder that causes acute cognitive deficits and abnormal emotional conditions manifested in thought, speech, and behavioral complications.

Schizophrenia is a chronic brain disorder that causes acute cognitive deficits and abnormal emotional conditions manifested in thought, speech, and behavioral complications. In turn, these contribute to social and occupational dysfunctions that impair the ability to live autonomously. Compared to the general population, patients with schizophrenia have higher decayed, missing and filled teeth scores, and are at increased risk of poor oral health. In addition, the side effects of prescribed treatment medications can adversely impact patients’ oral health.
Photo Credit: wildpixel / iStock / Getty Images Plus
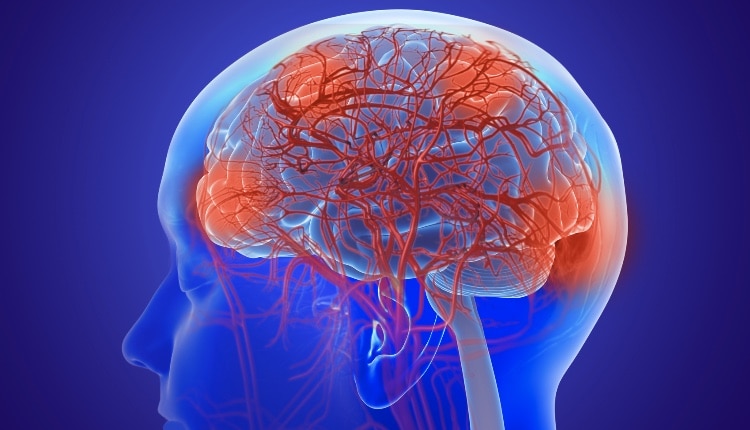
Age of Onset and Longevity
Although there is no specific age for onset, schizophrenia can occur as early as age 5. Generally, onset is between the ages of 10 and 25 for men, and 25 and 35 for women. Mortality risk among patients with schizophrenia is two times to three times higher than the general population. This increased mortality risk is multifactorial, and exacerbated by comorbidities. Some of the key causes of death among these patients include cardiovascular disease, respiratory diseases, suicide, and substance abuse.
Photo Credit: Lars Neumann / iStock / Getty Images Plus
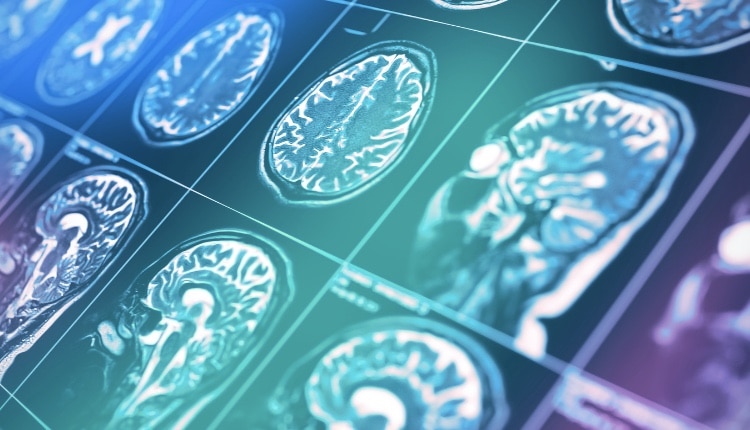
Three Phases
Although onset, severity, duration, and type of schizophrenia vary, generally, the disorder manifests in three phases—prodrome; active, or acute; and residual—preceded by a premorbid phase. Other than slight indications of social, cognitive, or behavioral deficits (with possible minor physical anomalies), there are no clear signs of schizophrenia in the premorbid phase. In the prodromal phase, although criteria for clinical diagnosis are unmet, there are manifestations of negative symptoms, along with the emergence of positive symptoms. Clinical diagnosis is the onset of the disorder’s acute phase, which can include behavioral complications. Patients who enter the residual phase—typically during adulthood and between middle and old age—see discernable reduction of positive and negative symptoms, as well as cognitive and social impairments—but relapses can occur. Behavioral issues can persist even in this phase.
Photo Credit: sudok1 / iStock / Getty Images Plus

Medication Usage
Pharmacological treatment of schizophrenia primarily relies on first-generation antipsychotics (FGA) and second-generation antipsychotics (SGA) to control positive symptoms. Common FGAs include chlorpromazine, thioridazine, perphenazine, fluphenazine, haloperidol, thiothixene and trifluoperazine. Commonly prescribed SGAs include aripiprazole, clozapine, olanzapine, quetiapine, risperidone, and ziprasidone. Both FGAs and SGAs cause xerostomia and hyposalivation—side effects that are also caused by tricyclic antidepressants and mood-stabilizing drugs (eg, carbamazepine and valproate) prescribed as part of the treatment. Dry mouth conditions may produce oral malodor. They may also increase risk for caries and other oral lesions (eg, candidiasis, glossitis or generalized stomatitis), and create difficulty eating, swallowing, and speaking.
Photo Credit: artisteer / iStock / Getty Images Plus
Oral Health Care
Oral care treatments are dependent on the state of the patient’s disorder and, to this end, an understanding and application of the phases of schizophrenia development will prove clinically useful. Oral health professionals should review the patient’s complete medical history and perform an oral examination. For patients clinically diagnosed with schizophrenia, the provider should note prescribed medications, allergies, contraindications, concurrent medical conditions, comorbidities, and recorded behavioral, emotional and cognitive impairments.
Photo Credit: AlexLMX / iStock / Getty Images Plus

Diagnosis and Treatment Planning
Based on the data collected during assessment, the provider determines the patient’s oral health status, which might include xerostomia, periodontitis, caries and other oral lesions. The diagnostic report should note any condition that can impact treatment, such as physical impairments, behavioral issues, emotional issues (such as anxiety), and cognitive dysfunctions. The diagnostic statement should assist in creating a treatment plan involving therapeutic and preventive therapies, as well as identifying oral health education targets. For example, with xerostomia the treatment approach should be based on cause and severity. When managing caries, an evidence-based approach, such as caries management by risk assessment, should be incorporated in the treatment plan.
Photo Credit: designer491 / iStock / Getty Images Plus

Evaluation and Documentation
Dental teams should monitor the patient’s progress during office visits and obtain updates from other healthcare providers (if deemed necessary) to ensure evaluation is based on current information. Reevaluation appointments should be scheduled as appropriate to monitor the patient’s oral health status and engage the patient in maintaining motivation and improving self-care techniques. Oral health professionals should ensure all documents are current, including medical and dental histories, oral assessment reports, diagnostic reports, oral care plans, evaluation statements, and emergency response plans. In addition, patient consent forms, disclosures and contact information (for all care team members) should be kept current. These written representations ensure that all oral health team members, including the patient, understand the diagnoses, care provided, and outcomes.

