A Growing Aging Population
The population of the United States is aging, and it will continue to do so as advances in medicine help Americans live longer.

A Growing Aging Population
The population of the United States is aging, and it will continue to do so as advances in medicine help Americans live longer. In 2014, life expectancy across the total US population was 76.4 years for men and 81.2 years for women. In light of this, oral health professionals are likely to treat older adults—defined as individuals age 65 or older—with increasing regularity. Dental hygienists must be prepared to meet the needs of this aging population, and to make dental visits easier by recognizing the challenges they face.
Photo Credit: SolStock / E+

Significant Oral Health Challenges
According to the US Centers for Disease Control and Prevention (CDC), in 2006, approximately 25% of the US population age 60 and older were edentulous. It also notes that 23% of individuals between age 65 and 74 have severe periodontal diseases, and that older Americans may experience caries at rates that surpass those found in children. The CDC reports that oral and pharyngeal cancers—which are diagnosed in 31,000 Americans each year—result in 7,400 deaths each year, and that these cancers are primarily found in older adults. As such, older adults should be encouraged to maintain recare intervals that allow dental professionals to monitor oral health and screen for precancerous and cancerous lesions.
Photo Credit: PeopleImages / E+

Barriers to Accessing Care
Lack of adequate dental insurance, either public or private, is a major consideration for older adults, who may be on Medicare or have a fixed income. Medicare does not cover routine dental services (eg, prophylaxis, restorations, or dentures) unless additional coverage, such as Medicare Advantage, is purchased. In addition, disabilities, illnesses, and logistics may affect the decision to seek dental care. Older adults may have transportation issues, which can be especially problematic if multiple appointments are needed. A wide range of medications can affect oral health, and individuals within this patient population typically use multiple medications to treat chronic conditions. Many prescribed medications inhibit salivary flow and, as a side effect, may cause xerostomia—which, in turn, can contribute to the caries process. These individuals may also have medical or physical conditions that make it difficult to perform effective self-care.
Photo Credit: Bill Oxford / iStock / Getty Images Plus

Difficulty With Oral Hygiene
The most common chronic conditions among this patient cohort are arthritis, hypertension, hearing loss, heart disease, and visual impairment. Other conditions that can affect these patients include limited manual dexterity, diminished peripheral circulation, loss of taste, and functional or organic mental disorders. Limited dexterity and diminished peripheral circulation can put patients at increased risk of caries and periodontal diseases due to difficulty with oral self-care. Devices, either homemade or commercially available, can assist patients by adapting the toothbrush or interdental cleaning aid so it is easier to use. As part of efforts to manage self-care, oral health professionals should be prepared to offer appropriate recommendations and encourage regular dental visits.
Photo Credit: Deagreez / iStock / Getty Images Plus

Hearing Loss
When treating patients with hearing impairments, oral health professionals should eliminate background noises whenever possible. Clinicians are advised to face the individual and talk slowly and distinctly. Some patients may be able to hear, but have difficulty distinguishing sounds. Because consonants are more difficult to hear than vowels, choosing words carefully or using alternate expressions can be helpful. It may also be necessary to repeat questions or instructions. When appropriate—and if not providing treatment—oral health professionals may remove their masks so patients can see their lips as they talk. If the procedure requires the removal of hearing aids (such as when taking a panoramic radiograph), issue instructions to the patient before the hearing aids are removed.
Photo Credit: Ridofranz / iStock / Getty Images Plus

Vision Loss
Multiple types of visual impairments can affect older adults, and it is important to understand these conditions and what can be done to help patients during a dental visit. Patients with glaucoma, for example, may have tunnel vision, so it is helpful for clinicians to remain in the patient’s central line of vision. The opposite effect occurs with macular degeneration. Although these patients can see peripherally, they cannot see well in the center of vision. Magnifying glasses may be helpful if patients with macular degeneration must read material, such as consent forms, during the dental visit. When possible, keep the lights low in the treatment area. Clinicians are also advised to remain in patients’ peripheral vision area, and not in the central line of vision. Another condition that can affect one or both eyes is hemianopia or hemianopsia. An individual with this condition has a lack of vision on one side. When addressing this patient, oral health professionals should stay out of the area that is blocked, and remain aware of obstacles in the patient’s way.
Photo Credit: Ljupco / iStock / Getty Images Plus
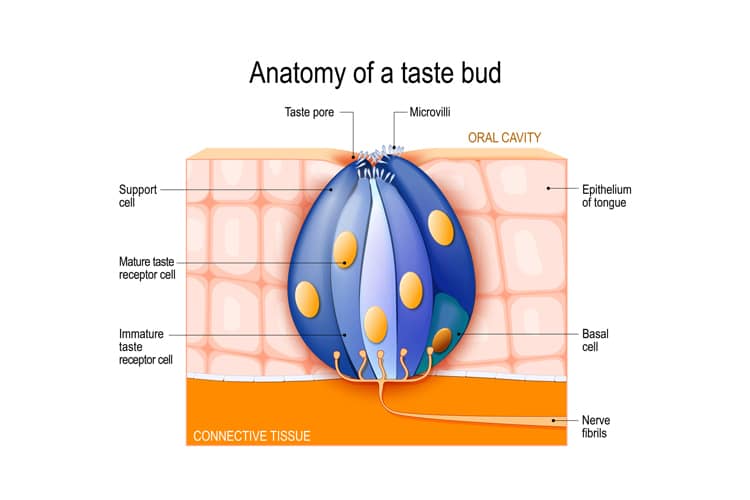
Taste
The loss of taste is another part of the aging process. A baby is born with 10,000 taste buds, but, by age 50, an adult will start losing taste buds. Contributing factors include medication usage, vitamin deficiencies, xerostomia, changes in salivary composition, diseases, and surgeries. Among older adults, the loss of taste can affect eating habits, potentially resulting in weight loss, poor nutrition, and vitamin deficiencies. It may be difficult for older adults to take medications.

