Ensure Oral Health During Pregnancy
Pregnant women experience an increase in progesterone and estrogen, which exacerbates the inflammatory response to gingival irritants, such as plaque biofilm.

Pregnant women experience an increase in progesterone and estrogen, which exacerbates the inflammatory response to gingival irritants, such as plaque biofilm. Simultaneously, changes in the oral microflora favor the pathogens associated with gingivitis. As a result, pregnant women are more susceptible to gingivitis, pregnancy granuloma, periodontal diseases, and dental caries.
Photo Credit: PeopleImages / E+
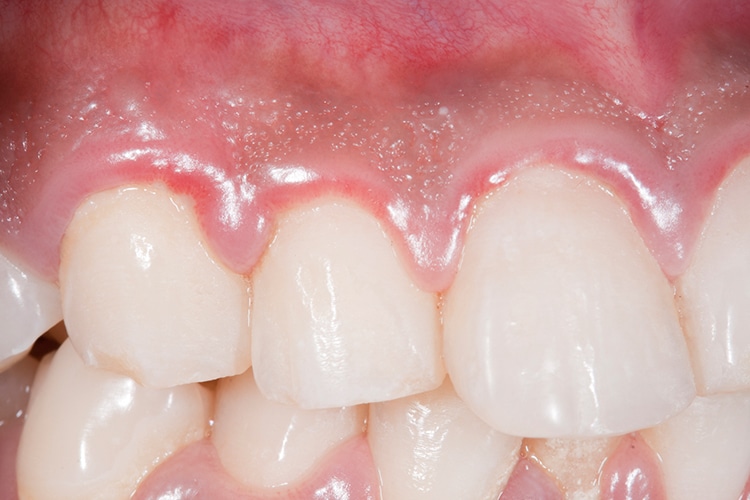
Gingivitis Is Common
Gingivitis is a common oral condition that affects up to 75% of pregnant women. Increased levels of estrogen and progesterone, changes in the oral flora, and a weakened immune system affect gingival tissue and cause inflammation. Poor oral hygiene and increased biofilm can exaggerate the gingival response. Pregnant women may experience gingivitis beginning in the second month and continuing throughout pregnancy. Although the severity may improve post-partum, most women who experience gingivitis during pregnancy will likely have some form of the disease after pregnancy.
Photo Credit: watanyou / iStock / Getty Images Plus
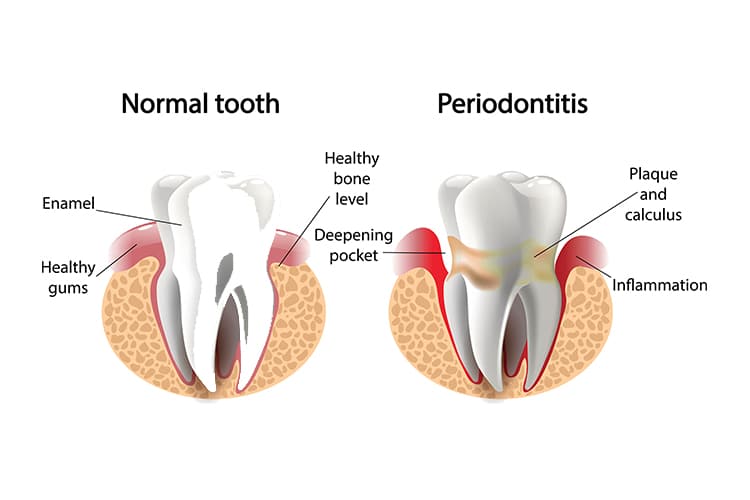
A Variety of Oral Health Issues
A pregnancy granuloma, sometimes called a pregnancy tumor, may form as the result of local irritants, such as plaque biofilm due to poor oral hygiene or forming on overhanging restorations. It is most commonly seen along the maxillary anterior labial aspect of the interdental papilla. The color ranges from dark red to bluish purple. It is usually no larger then 2 cm and bleeds easily. Pregnancy granulomas will often self-resolve. If surgical excision is required, it is best-performed post pregnancy, as recurrence during pregnancy is possible. The hormonal changes that occur during pregnancy increase a women’s susceptibility to periodontal pathogens and reduce the body’s ability to repair oral soft tissues. Periodontal diseases have been associated with adverse pregnancy outcomes.
Photo Credit: ElenBushe / iStock / Getty Images Plus
Caries Risk Increases
Changes in the oral environment during pregnancy can increase the risk for caries. Pregnant women tend to crave a diet high in sugar and fermentable carbohydrates, increasing the risk for caries. In addition, many pregnant women experience nausea and vomiting, which can compromise oral hygiene efforts. Vomiting also increases acidity in the oral cavity. At later stages of pregnancy, the upward pressure from an expanding uterus may cause acid reflux. This type of acidic environment favors cariogenic bacteria and can also cause erosion. Additionally, cariogenic Streptococcus mutans passes from mother to infant through vertical transmission. The bacterium is transferred by sharing utensils or toothbrushes, kissing on the lips, cleaning a dropped pacifier by mouth, or the prechewing of food. Pregnant women with untreated caries have high levels of S. mutans in their saliva and are thus likely to pass the bacteria onto their offspring. Children who acquire the bacterium at an early age have a greater risk of developing early childhood caries.
Photo Credit: M_a_y_a / E+

Impediments to Dental Care
Although the most common reason cited for not seeking care is lack of perceived need, research shows access to care also plays a role. The likelihood of low-income and uninsured women receiving such care is even lower. Oral health coverage for pregnant women varies by state, although states must cover pregnancy-related services. This means Medicaid-eligible pregnant women must receive oral health services if the oral condition is exacerbated by the pregnancy or could negatively impact the pregnancy. Access to care may also be hindered by low oral health literacy and language barriers. All health professionals should ensure patients understand the information presented and are given the opportunity to ask questions.
Photo Credit: Igor Alecsander / iStock / Getty Images Plus

Safe Treatment
The Oral Health Care During Pregnancy: A National Consensus Statement declares that comprehensive oral care—including necessary radiographs and use of approved local anesthesia—are beneficial during pregnancy and pose no fetal or maternal risk. Furthermore, treatment can be safely rendered any time during pregnancy, although pregnant women may be most comfortable being treated in the second trimester. Pregnant women may experience nausea and vomiting in the first trimester and any manipulation of oral tissues may worsen the symptoms.

