 Delmaine Donson / E+
Delmaine Donson / E+
A Free Gingival Graft Saves the Day
This case report details how this approach helped correct a complete lack of attached tissue thickness in a young woman.
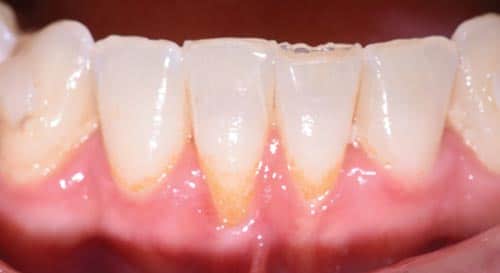
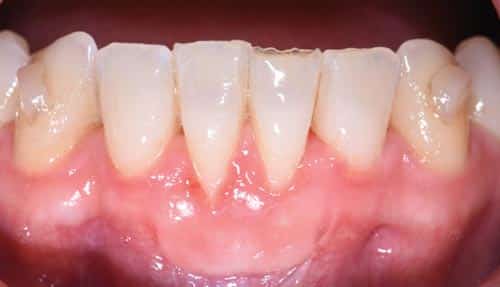
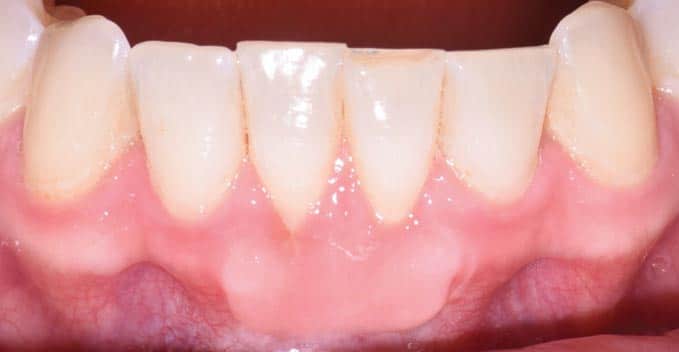
This case outlines the steps taken to correct a complete lack of attached tissue thickness and amount by means of a free gingival graft. A 29-year-old woman was concerned about worsening recession (Figure 1 to Figure 3). The patient had no significant medical history. After a thorough patient evaluation and review of varying techniques and materials, a surgical treatment plan was developed, and consents were obtained. The treatment plan included a free gingival graft #24, #25 area using an enamel matrix derived growth factor and a coronally repositioned flap to obtain root coverage as needed.1
After initial findings were charted both manually and with an intraoral scan, an increase in keratinized tissue width was determined to be the primary goal. The patient had a shallow vestibule, absent attached tissue around #24 and #25, thin phenotype, labial tooth position #25 due to ongoing orthodontic treatment, and fair oral hygiene. Complete root coverage was not initially guaranteed because of these site-related risk factors.
The recipient site was carefully prepared with partial-thickness dissection from #24-#25 and distal oblique vertical releases. A free gingival graft measuring 8 mm long x 10 mm to 12 mm wide x 1.5 mm thick was harvested from the right palate, trimmed to remove excess adipose tissue, and hydrated in an enamel matrix derived growth factor. EDTA root surface conditioner with a concentration of 24% was used over #24, #25 before applying the growth factor. The graft was secured and stabilized at the #24, #25 area with simple interrupted, nonresorbable sutures.
Gauze pressure was applied to the palatal wound and multiple layers of hemostatic gauze were placed and sutured along the donor site for profound hemostasis. A palatal stent was then delivered to further minimize her post-operative bleeding risk, and a periodontal dressing was placed over the recipient site. The patient was discouraged from looking at or manipulating the operated sites for at least 2 weeks.
The patient returned for weekly follow-ups and was initially maintained by the specialty practice. Proper oral hygiene techniques were demonstrated at each visit to establish better self-care. A power toothbrush with a pressure indicator was recommended. The recipient site was scaled and polished as needed.
Further root coverage can be appreciated during this time with the gradual and coronal reformation of the gingival sulcus. She will finish her orthodontic treatment and alternate prophylaxis every 6 months with her general dentist and periodontist. She denied any esthetic or sensitivity concerns following treatment.
Procedures to cover exposed roots or increase keratinized tissue width have evolved over time. Site- and patient-related risk factors should be discussed as part of the initial exam, especially if any interdisciplinary treatment is planned. Gingival recession can be treated successfully when identified early on. Esthetics, sensitivity, and worsening recession are important drivers for surgical treatment. Dental hygienists play an important role in the prevention and maintenance of mucogingival defects through patient education and regular prophylaxis.
Reference
- Bernimoulin JP, Lüscher B, Mühlemann HR. Coronally repositioned periodontal flap. Clinical evaluation after one year. J Clin Periodontol. 1975;2:1–13.
This information originally appeared in Saltz AE, Sirois V. The dental hygienist’s role in treating gingival recession. Dimensions of Dental Hygiene. May 2022; 20(5)32-35.

